Many people with anxiety make common anxiety mistakes. They try stress management mistakes, like quick stress relief tips. But these often trigger the fight or flight response. Instead of feeling calmer, they end up more on edge, restless, and discouraged due to chronic stress.
Anxious nervous systems need nervous system regulation first. They do not need more effort or techniques that lead to cortisol imbalance, burnout, and anxiety. Poor anxiety coping strategies and avoidance behavior make stress habits that worsen anxiety even harder to break.
Why does stress management not work for you? Discover better ways to manage anxiety, along with mistakes to avoid and simple fixes ahead.
Why “Trying Harder” Backfires
Anxiety sensitizes the stress response, so strategies that soothe others can overwhelm those with heightened reactivity. Pressure, punishment, or generic advice keeps the body locked in fight-or-flight, amplifying chronic worry.
Common signs stress management isn’t working:
- Constant anxiety or worry dominates daily life.
- Trouble sleeping due to racing thoughts.
- Frequent headaches, stomachaches, or fatigue.
- Difficulty focusing or concentrating.
- Feeling like a failure if calm doesn’t come “on command.”
- Tense body despite journaling or meditating.
- Wellness tasks lead to burnout, not relief.
“If you’re experiencing [restlessness, irritability, insomnia, hypervigilance] all the time, it feels dangerous… Regulating the nervous system doesn’t mean being calm all the time. It means reacting flexibly to stress without getting stuck.”
Dr. Emily Kostelnik, Clinical Psychologist.
1. Trying to Eliminate Stress Completely
Stress-free living sounds ideal, but unrealistic stress aids adaptation, focus, and safety. Aiming for zero stress turns every anxiety spike into failure, boosting self-criticism and worry.
How avoidance reinforces anxiety:
- Avoiding triggers such as conversations, deadlines, or decisions may signal to the brain that daily life is dangerous.
- It shrinks your world, spikes anticipatory anxiety, and links to chronic stress/low mood.
- Example: Skipping public speaking prevents skill-building and creates a fear cycle.
What helps instead:
- Focus on regulation: Notice stress early, return to baseline.
- Build “tolerance reps” with manageable challenges and include breathing, movement, or breaks to teach safety.
Read More: How Quality Sleep Supports Diabetes Management: Tips for a Healthier Life
2. Using Relaxation Only in Crisis

Reaching for apps or music during panic floods the body with hormones, making tools feel useless or irritating.
Why consistency matters more:
- Daily calming practices (slow breathing, gentle stretching) build resilience, shift baseline arousal.
- The brain learns safety cues through repetition, like daily guitar practice, rather than sporadic sessions.
Daily habit tips:
- Pair with routines: 3 slow breaths before email; 5-minute walk after lunch.
- Aim for “good enough” most days; predictability enables reliable downshifts.
3. Forcing Mindfulness or Meditation
These help many, but intensify distress for those with chronic worry, trauma, or racing minds; sitting still amplifies thoughts/sensations without safety.
When it backfires:
- Silent sessions surface intrusive memories or fears too quickly.
- Expecting to “empty the mind” breeds self-blame when thoughts return.
Movement-based grounding first:
- Start with walking, light yoga, or somatic exercises to discharge energy.
- Use short, guided practices emphasizing curiosity/self-compassion over perfection.
Read More: Stress Management Tools: 7 Relaxation Aids for Calming the Mind and Body
4. Ignoring Physical Stress Signals
Anxiety hits the body first and leads to tight shoulders, jaw clenching, shallow breathing, and GI issues. Dismissing them keeps the nervous system revved.
Why somatic awareness matters:
- Chronic stress raises cortisol, risking sleep issues/mood disorders.
- Early cues allow rest, stretching, or boundaries before spikes.
Simple body check-ins:
- Scan head-to-toe daily: “Where am I clenching or holding breath?”
- Gentle fixes: uncross your legs, relax your jaw, and lengthen your exhales to signal safety.
5. Replacing Rest with “Productive” Self-Care

Wellness culture turns self-care into to-do lists (perfect routines, habit tracking), keeping the brain in control mode.
How it worsens anxiety:
- “Am I doing this right?” fuels perfectionism/evaluation stress.
- Over-scheduling “relaxation” crowds out unstructured rest/play/sleep for repair.
Redefining rest:
- Low-effort breaks: Lie down, stare out of the window, listen to music with no goals.
- Pick 1-2 anchors:Consistent wind-down, short walk over ideal routines.
Read More: Balance Your Stress: The Top 6 At-Home Cortisol Tests for Stress Management
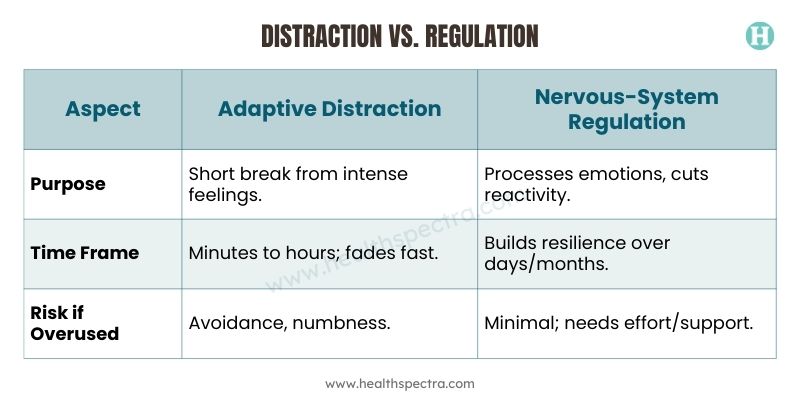
6. Using Distraction Instead of Regulation
Short-term distraction aids overwhelm, but constant scrolling/bingeing skips processing, letting anxiety rebound.
Healthy distractions build safety and learning:
- Play a game or call a friend during anxiety spikes. Then reflect on the activities and try to get good sleep.
- Take a short walk in nature when chronic stress hits. Follow with deep breathing and observe your emotions rising and falling safely.
Unhelpful habits block progress:
- Auto-numbing with endless scrolling. This discomfort block stops you from learning how emotions rise and fall safely.
- Binge-watching to escape the fight or flight response. It worsens the cortisol imbalance over time.
7. Avoiding Professional Support

Many people delay therapy for anxiety. They think it “is not bad enough yet.” Or they fear judgment or medication. So they stick to self-help instead.
Why guided support accelerates relief:
- Therapists spot patterns that self-help misses. These include perfectionism and people-pleasing.
- Evidence-based tools (CBT, exposure, trauma care) rewire threat responses.
When to reach out:
- Anxiety disrupts sleep/work/relationships for weeks.
- Panic attacks, unexplained symptoms, or feeling stuck despite self-care.
Why These Mistakes Are So Common
One-size-fits-all advice ignores anxiety’s brain-body tweaks; social media pushes quick fixes over personalization.
Key background factors:
- Chronic stress dysregulates the HPA axis, heightening reactivity/anxiety/mood issues.
- Regulation needs lifestyle shifts/therapy, not instant calm.
Read More: Stress Management Techniques for Expectant Mothers
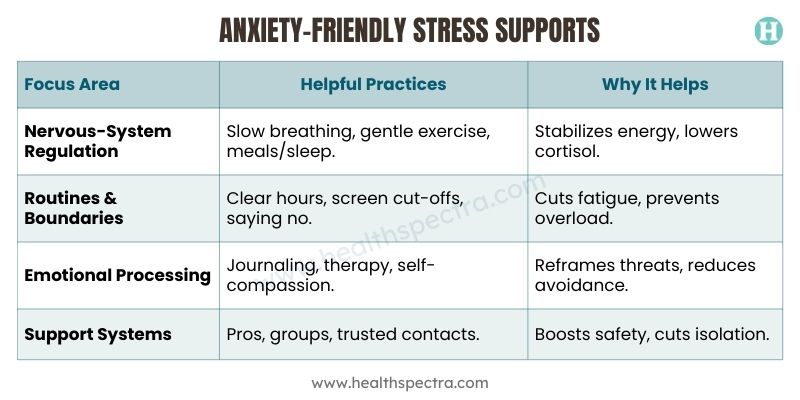
What Actually Supports Anxiety-Driven Stress
Prioritize safety signals, predictability, and reliable support instead of total control. Small daily practices outperform big overhauls.
 When Stress and Anxiety Need Professional Help
When Stress and Anxiety Need Professional Help

Self-guided strategies often fall short when anxiety and stress symptoms persist beyond a few weeks, turning manageable discomfort into chronic patterns that disrupt daily life.
Seek early intervention from qualified professionals, such as therapists, psychologists, or primary care providers who can prevent escalation, reduce long-term risks such as depression or burnout, and equip you with personalized tools for lasting regulation.
In the U.S., options include in-person therapy, telehealth via platforms like BetterHelp or Talkspace, or employee assistance programs (EAPs) for confidential support.
Key signs it’s time to reach out:
- Persistent worry, panic, or irritability: Racing thoughts or panic attacks most days for more than two weeks, interfering with work, relationships, or enjoyment.
- Unexplained physical symptoms: Chest tightness, chronic headaches, stomach pain, muscle tension, or fatigue without a clear medical cause that often causes anxiety, manifesting somatically.
- Sleep issues or substance reliance: Insomnia, nightmares, or using alcohol/caffeine to cope, leading to a vicious cycle of exhaustion and heightened reactivity.
- Daily dysfunction: Struggling to focus, meet deadlines, maintain hygiene, or engage socially; feeling “stuck” despite consistent self-care efforts.
- Self-harm thoughts or total overwhelm: Any suicidal ideation, hopelessness, or inability to function should be considered and treated as an emergency.
For immediate crises, dial 988 (Suicide & Crisis Lifeline) helplines, which are available 24/7 for free, confidential support via call, text, or chat. It connects to local responders trained in de-escalation. Other resources: National Alliance on Mental Illness (NAMI) helpline at 1-800-950-6264 or Crisis Text Line (text HOME to 741741).
Professionals use evidence-based approaches like Cognitive Behavioral Therapy (CBT) to reframe anxious thoughts,
Exposure Therapy to build tolerance for triggers, or EMDR for trauma-related stress. Medication (e.g., SSRIs) may be chttps://newsinhealth.nih.gov/2013/04/benefits-slumberonsidered short-term by psychiatrists if symptoms are severe, but therapy often forms the core.
Read More: Poop Anxiety: Why It Happens and How to Overcome It
Key Takeaways
- Stress tips that aren’t anxiety-friendly can keep you stuck: Zero-stress goals create failure loops; crisis-only tools miss daily regulation; forced meditation amplifies distress; ignoring body signals prolongs activation; “productive” self-care adds pressure; distraction delays processing; skipping pros leaves root causes untouched.
- Shift to nervous-system-friendly habits: Prioritize regulation through consistent routines (e.g., fixed sleep/wake times), gentle movement (walks, yoga), breath awareness, the 4-7-8 breathing technique, and honest emotional processing like journaling without judgment.
- Professionals accelerate real change: They identify hidden patterns (such as perfectionism and avoidance) and retrain responses when symptoms disrupt life. Therapy isn’t failure, it’s efficient support.
- Progress means working with stress: Understand your body’s signals, build safety through small reps, and embrace compassion over control. Relief builds gradually, not perfectly, and starts with one pro contact or 988 if overwhelmed today.
References
- Hoge, E. A., Bui, E., Mete, M., Dutton, M. A., Baker, A. W., & Simon, N. M. (2023). Mindfulness-based stress reduction vs escitalopram for the treatment of adults with anxiety disorders: A randomized clinical trial. JAMA Psychiatry, 80(1), 13–21.
- van Dis, E. A. M., van Veen, S. C., Hagenaars, M. A., Batelaan, N. M., Bockting, C. L. H., van den Heuvel, R. M., Cuijpers, P., & Engelhard, I. M. (2020). Long-term outcomes of cognitive behavioral therapy for anxiety-related disorders: A systematic review and meta-analysis. JAMA Psychiatry, 77(3), 265–273.
- Majid, S. A., Seghatoleslam, T., Homan, H. A., Akhvast, A., & Habil, H. (2012). Effect of mindfulness based stress management on reduction of generalized anxiety disorder. Iranian Journal of Public Health, 41(10), 24–28.
- Carlbring, P., Nilsson-Ihrfelt, E., Waara, J., Kollenstam, C., Buhrman, M., Kaldo, V., & Andersson, G. (2005). Randomized controlled trial of internet-based stress management. Cognitive Behaviour Therapy.
- Leichsenring, F., Steinert, C., & Kruse, J. (2020). Long-term outcomes of cognitive behavioral therapy for anxiety-related disorders. JAMA Psychiatry.
- Goldberg, S. B., Tucker, R. P., Greene, P. A., Davidson, R. J., Wampold, B. E., Kearney, D. J., & Simpson, T. L. (2020). Mindfulness-based interventions for psychiatric disorders: A systematic review and meta-analysis. Clinical Psychology Review.
- Kriakous, S. A., Elliott, K. A., Lamers, C., & Owen, R. (2018). A stress reduction program adapted for the work environment: A randomized controlled trial. Frontiers in Psychology, 9, 668.
- Carpenter, J. K., Andrews, L. A., Witcraft, S. M., Powers, M. B., Smits, J. A. J., & Hofmann, S. G. (2018). Cognitive behavioral therapy for anxiety and related disorders: A meta-analysis of randomized placebo-controlled trials. Depression and Anxiety.
- Hoge, E. A., Bui, E., Mete, M., Simon, N. M., & Dutton, M. A. (2013). Randomized controlled trial of mindfulness meditation for generalized anxiety disorder: Effects on anxiety and stress reactivity. The Journal of Clinical Psychiatry.
- Jeffries, F. W., & Davis, P. (2013). What makes mindfulness-based stress reduction effective? A randomized controlled trial. Stress and Health.
- Springer, K. S., Levy, H. C., & Tolin, D. F. (2018). Cognitive behavioral therapy for anxiety and related disorders: A meta-analysis of randomized placebo-controlled trials. Depression and Anxiety.
- Arch, J. J., Wolitzky-Taylor, K. B., Eifert, G. H., & Craske, M. G. (2013). Randomized clinical trial of adapted mindfulness-based stress reduction versus group cognitive behavioral therapy for heterogeneous anxiety disorders. Behaviour Research and Therapy.
- Leichsenring, F., Steinert, C., & Loibl, M. (2022). Efficacy of cognitive behavioral therapy for anxiety-related disorders: A meta-analysis. Psychotherapy and Psychosomatics.
- Hofmann, S. G., Sawyer, A. T., Witt, A. A., & Oh, D. (2010). The effect of mindfulness-based therapy on anxiety and depression: A meta-analytic review. Journal of Consulting and Clinical Psychology.
- Querstret, D., Cropley, M., & Fife-Schaw, C. (2023). Improving stress management, anxiety, and mental well-being in medical students using a smartphone app: A randomized controlled trial. Scientific Reports, 13, Article 8543.
In this Article