Thinking of IVF? Exercise, weight, and everyday habits can strongly support your chances with IVF, but they can never guarantee a positive result, because IVF is a powerful tool, not a magic bullet.
Aligning your lifestyle with your treatment simply helps your body become more receptive to assisted reproductive technology (ART).
How lifestyle factors influence IVF
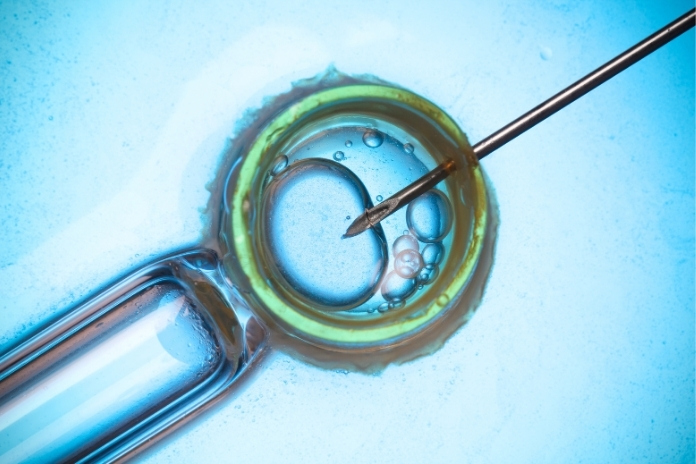
IVF involves stimulating the ovaries to grow multiple follicles, retrieving mature eggs, fertilising them with sperm in the lab, and transferring embryos into the uterus for implantation.
Each stage is influenced by metabolism, hormones, inflammation, sleep, and stress, which together affect ovulation, egg and sperm quality, endometrial receptivity, and pregnancy outcomes.
Key lifestyle variables that support IVF success and fertility care:
- Better insulin sensitivity and weight can enhance ovarian response, fertilisation, and embryo implantation.
- Regular moderate exercise and stress management may lower cortisol and are linked with higher implantation and live‑birth rates in some patients.
- Nutrient‑dense diets, good sleep, and avoiding smoking and excess alcohol protect hormones and reduce inflammation that may interfere with ART outcomes.
Read More: How Many Eggs Do You Have at 20, 30, and 40? What Fertility Science Says
Exercise and IVF: helpful or harmful?
What research says about exercise and fertility
Moderate physical activity before and during IVF is associated with improved metabolic health, hormone regulation, and cardiovascular fitness, all of which support reproductive function.
Some studies report that women who are regularly active can have nearly double the clinical pregnancy and live‑birth rates compared with inactive women undergoing IVF.
Ways exercise supports IVF success and ovulation:
- Increased blood flow helps deliver oxygen and nutrients to the uterus and ovaries.
- Balanced training helps combat stress, anxiety, and inflammation, indirectly supporting hormonal balance and egg quality.
- Maintaining a healthy BMI through movement and diet can improve the effectiveness of fertility medications and lower complication risk.
Best exercise types during IVF
For IVF success and lifestyle, the goal is steady, moderate movement rather than intense, high‑impact training.
Most health organisations suggest at least 150 minutes per week of moderate aerobic activity, tailored to your fertility specialist’s advice.
Supportive exercise options for ART cycles:
- Brisk walking, gentle cycling on flat ground, or swimming to boost circulation without overheating or jarring the pelvis.
- Light to moderate resistance training 2–3 times weekly to maintain muscle, improve insulin sensitivity, and protect bone health.
- Gentle movement yoga, stretching, mobility work, or slow dancing to ease stress and regulate the nervous system.
When exercise can backfire
Excessive high‑intensity or endurance exercise can over‑stress the body and may reduce IVF success, especially in women with a normal BMI.
Overtraining can disrupt ovulation, alter luteal‑phase hormones, and cause energy deficiency that makes implantation less likely.
Signs your routine may be too intense for IVF:
- More than 4–7 hours of vigorous exercise per week, with frequent breathless, exhausting sessions and little recovery.
- Missed or irregular periods, extreme fatigue, poor sleep, or repeated injuries, suggesting energy imbalance and hormonal disruption.
- Feeling unable to reduce training despite medical advice, which may signal the need for professional support.
Body weight, BMI, and IVF success

Why weight matters; but isn’t everything
Body fat acts as an endocrine organ, influencing estrogen production, insulin sensitivity, and inflammatory pathways. Both underweight and overweight BMI ranges can affect ovulation, egg quality, uterine lining, and response to IVF medications, but IVF success is seen across a wide range of body sizes.
Weight is therefore a modifiable risk factor, not a personal verdict on worth or “deserving” parenthood.
Interaction between BMI and fertility treatment:
- Higher BMI is linked with reduced ovarian responsiveness, fewer eggs retrieved, and lower implantation and live‑birth rates in many studies.
- Underweight women often have irregular menstrual cycles and hormonal imbalances that affect egg development and endometrial growth, even when IVF is used.
- Thoughtful weight loss or gain can improve metabolic health and outcomes, but crash diets tend to harm hormones and IVF response.
Underweight vs overweight: evidence summary
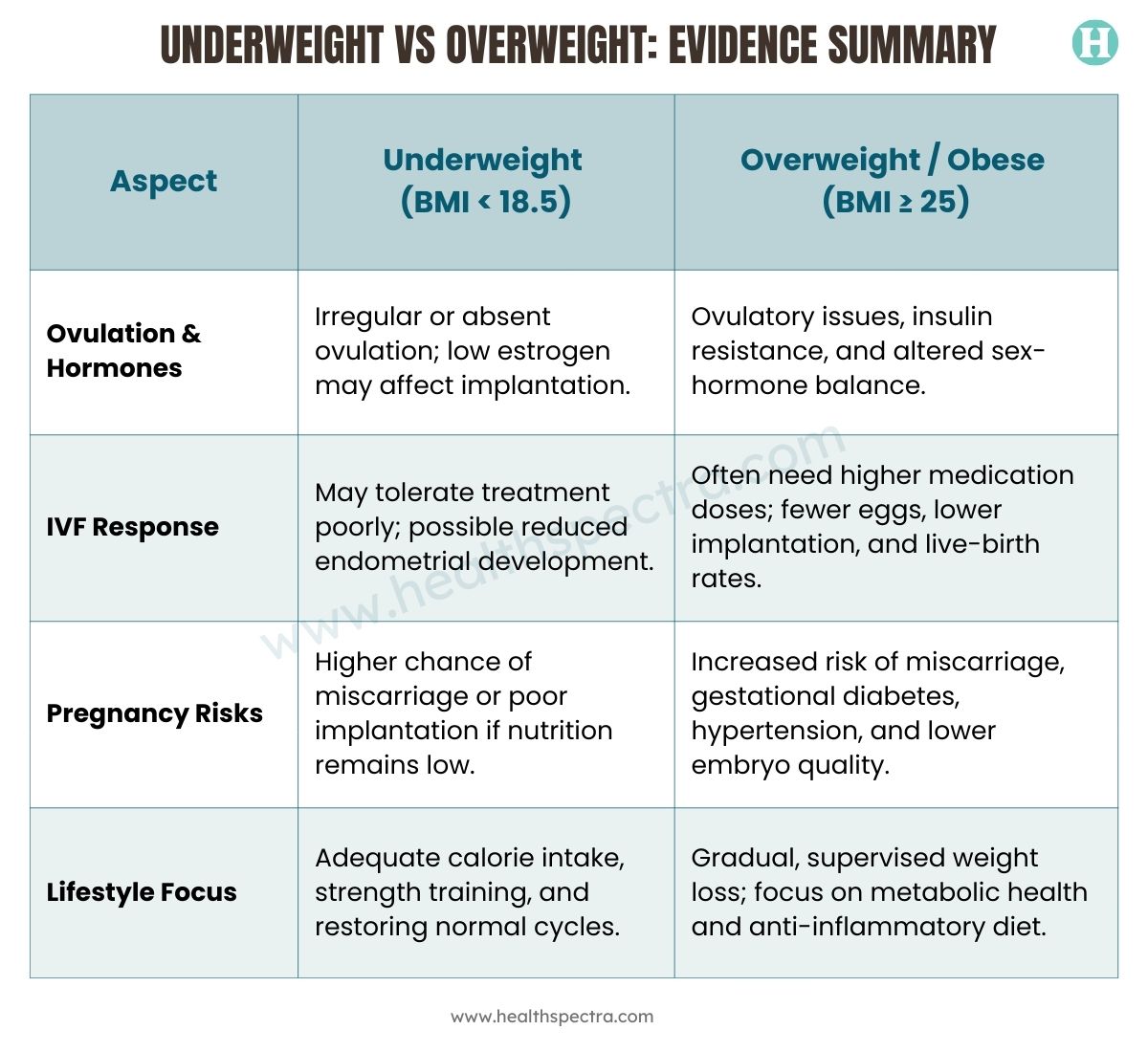 Even modest, sustained weight changes and better fitness can strengthen ovulation patterns and IVF response, particularly in people with obesity or insulin resistance.
Even modest, sustained weight changes and better fitness can strengthen ovulation patterns and IVF response, particularly in people with obesity or insulin resistance.
Still, rapid weight loss programmes immediately before IVF have not consistently improved live‑birth rates, so gradual, realistic changes are preferred.
Read More: Fertility Myths Women Still Believe (and What Science Actually Says)
Daily habits that support IVF

Nutrition, blood sugar, and metabolic health
A balanced diet helps maintain hormone balance, regular ovulation, and healthy embryo development during ART.
Mediterranean‑style eating, emphasizing vegetables, fruits, whole grains, legumes, lean protein, and healthy fats, are linked with better IVF outcomes in several studies.
Fertility‑friendly nutrition and metabolic health practices:
- Build meals around protein, fibre, and healthy fats to keep blood sugar steady and reduce insulin resistance.
- Include folate‑rich leafy greens, iron sources, omega‑3 fats (fatty fish, flaxseeds, walnuts), and antioxidant‑rich foods that support egg and sperm quality.
- Aim for adequate vitamin D, from safe sun exposure or supplements if recommended, and reduce added sugars and saturated/trans fats that drive inflammation.
Sleep, circadian rhythms, and stress
Short or irregular sleep can disrupt reproductive hormones such as LH, FSH, and melatonin, which may influence ovulation and implantation.
Night‑shift work and erratic bedtimes are linked with higher rates of menstrual irregularities and subfertility, making sleep hygiene a key lifestyle change before IVF.
Helpful sleep and stress strategies:
- Aim for 7–9 hours of regular sleep with consistent bed and wake times, even during treatment.
- Wind down with light stretching, reading, guided breathing, or mindfulness to lower stress hormones and ease anxiety.
- Consider counselling, support groups, or mind‑body programmes, which can reduce distress and may indirectly support IVF outcomes.
Alcohol, caffeine, and smoking
Pre‑IVF lifestyle changes tend to focus on modification, and sometimes abstinence, rather than rigid rules. Heavy alcohol, tobacco, or high caffeine intake are broadly linked with reduced fertility, poorer ART outcomes, and higher miscarriage risk, while moderate caffeine appears safer for most women.
Evidence‑based tips on habits that affect IVF success:
- Quit smoking and vaping where possible; stopping can improve egg and sperm quality and support implantation within months.
- Keep alcohol to minimal intake or avoid it during IVF stimulation and early pregnancy, as many clinics recommend.
- Limit caffeine to roughly 200 mg per day (about one to two small cups of coffee) unless your doctor suggests stricter limits.
Habits linked with lower IVF success
Certain habits can quietly work against your efforts to prepare for IVF naturally, even when other changes are in place. The goal is not flawless behaviour but steady, compassionate course correction away from patterns that over‑tax your body.
Habits to reconsider before or during IVF:
- Chronic dieting, very low‑calorie intake, or cutting entire food groups, which can suppress hormone production and ovulation.
- Overtraining without adequate rest, leading to high stress hormones, menstrual issues, and injuries.
- Frequent heavy drinking, smoking, or second‑hand smoke exposure, all of which damage sperm and egg quality.
- Irregular sleep, late nights, and high exposure to endocrine‑disrupting chemicals from certain plastics, pesticides, and personal‑care products.
Read More: Fertility Nutrition: What to Eat (and Avoid) When Trying to Conceive
Timing lifestyle changes for IVF

Egg and sperm development spans several weeks to months, so today’s habits can shape IVF cycles in the near future. Many fertility clinics suggest starting key lifestyle changes, around exercise, diet, weight, smoking, and alcohol, about 3–6 months before IVF when possible.
Even if your IVF cycle is starting soon, small changes still matter:
- Improving sleep, reducing alcohol, and cutting cigarettes or vaping can benefit hormonal balance within weeks.
- Gentle exercise, stress‑management, and nourishing meals can support both ovarian stimulation and embryo transfer.
- Focusing on realistic steps for your current timeline protects you from all‑or‑nothing thinking and burnout.
What lifestyle changes can’t do
Lifestyle interventions are powerful but cannot fully overcome age‑related declines in ovarian reserve, structural issues like blocked tubes or severe endometriosis, or genetic abnormalities in embryos.
Some patients with excellent lifestyles need several ART cycles, while others conceive despite high BMI or less‑than‑ideal habits, underscoring that many factors lie beyond personal control.
A compassionate, realistic mindset helps reduce guilt and self‑blame:
- IVF outcomes also depend on egg number, sperm DNA quality, embryo genetics, and uterine factors that are not fully modifiable.
- Lifestyle modification is best viewed as supportive care, strengthening resilience and emotional well‑being regardless of the final result.
Working with your fertility team
Customised advice from your fertility specialist is essential for safely adjusting fitness, weight, and daily habits during IVF. Your team knows your diagnosis, hormone levels, age, and previous cycle history, and can shape realistic targets for BMI, exercise, and timelines.
How to co‑create an IVF success and lifestyle plan:
- Ask clear questions about safe exercise intensity, your personal weight goals, and how long lifestyle changes might need to show benefits.
- Request referrals to fertility‑aware dietitians, physiotherapists, or mental‑health professionals if food, movement, or stress feel overwhelming.
- Including your partner, improving their sleep, exercise, and alcohol or smoking habits can also enhance sperm quality and embryo development.
When to be cautious and seek extra support
In some situations, additional professional support is important to keep lifestyle changes safe and sustainable before IVF. Ignoring warning signs and pushing through alone can worsen both physical and emotional health during an already demanding treatment.
Consider extra help if you notice:
- A history of eating disorders, extreme dieting, or obsessive monitoring of weight, calories, or exercise, especially when asked to “lose weight for IVF.”
- Persistent fatigue, burnout, exercise‑related injuries, or difficulty cutting back on intense workouts despite medical advice.
- Ongoing emotional distress, anxiety, or relationship strain during IVF therapy, group support, or mind‑body programmes can make a meaningful difference.
Read More: How Soon Should You See a Fertility Specialist? Signs It’s Time to Get Help
Final Summary
Fitness, body size, and lifestyle habits can meaningfully support natural fertility and IVF, but they will never guarantee success.
Small, sustainable improvements in exercise, nutrition, sleep, and substance use can positively influence metabolic and hormonal health across body sizes, while keeping expectations grounded in the reality that IVF outcomes depend on many factors beyond lifestyle alone.
References
- Al-Hasani, S., & Diedrich, K. (2023). Effects of body mass index on IVF outcomes in different age groups. PMC, PMC10410781.
- Bellver, J., Busnelli, A., Pellicer, A., Remohí, J., & Meseguer, M. (2004). The impact of female obesity on the outcome of fertility treatment. PMC, PMC2970793.
- Zhang, Y., & Wang, L. (2023). The association between body mass index and live birth and cumulative live birth rates following frozen embryo transfer. PMC, PMC10520462.
- Khan, M. J., & Al-Dhahir, Z. (2025). Impact of obesity on in vitro fertilization (IVF) outcomes. PMC, PMC12450106.
- Tamer, E. (2005). Overweight and obesity significantly reduce pregnancy. PMC, PMC8312282.
- Legro, R. S., & Barnhart, H. X. (2025). The effect of weight loss before in vitro fertilization on reproductive outcomes. PMC, PMC7618032.
- Li, X., & Zhang, Y. (2022). The association between caffeine and alcohol consumption and IVF/ICSI outcomes: A systematic review and dose–response meta‐analysis. PMC, PMC9812114.
- Wang, J., & Liu, H. (2025). Impact of sleep characteristics on IVF/ICSI outcomes. PubMed, 39672092.
- Chen, L., & Zhao, Y. (2025). Effect of body mass index on pregnancy outcomes in IVF. PMC, PMC11929203.
- Ata, B., & Urman, B. (2018). Maternal physical activity before IVF/ICSI cycles improves pregnancy. PMC, PMC5803901.
- Simmons, C. E., & Steiner, A. Z. (2017). Weight reduction intervention for obese infertile women prior to IVF. Human Reproduction, 32(8), 1621.
- Waylen, R., & Jones, G. L. (2019). Smoking and clinical outcomes of assisted reproductive technologies. PMC, PMC6420368.
- Fu, J., & Shen, H. (2017). Discrete survival model analysis of a couple’s smoking habits on IVF. PMC, PMC5416813.
- Sengupta, P., & Dutta, S. (2020). Effect of yoga on psychological distress among women undergoing IVF. PMC, PMC7336944.
- Gaskins, A. J., & Chavarro, J. E. (2021). Evaluating in vitro fertilization outcomes of patients with low BMI. PubMed, 33368250.
- Augood, C., & Duckitt, K. (2015). The effect of cigarette smoking, alcohol consumption on IVF. PMC, PMC4681150.
- Li, Y., & Zhang, Q. (2023). The impact of sleep on in vitro fertilization embryo transfer outcomes. PubMed, 36435629.
In this Article