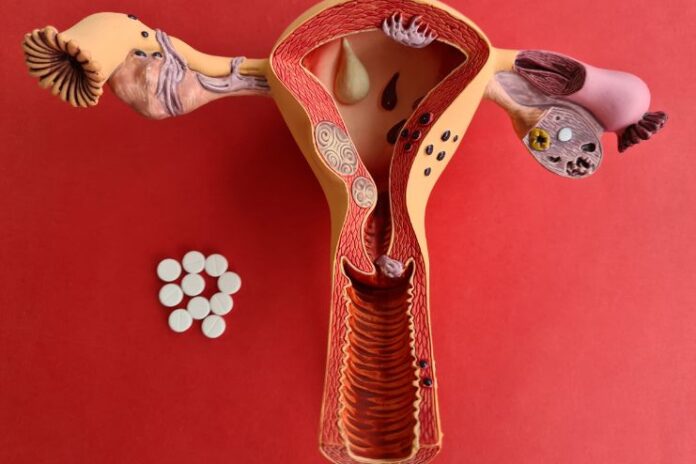
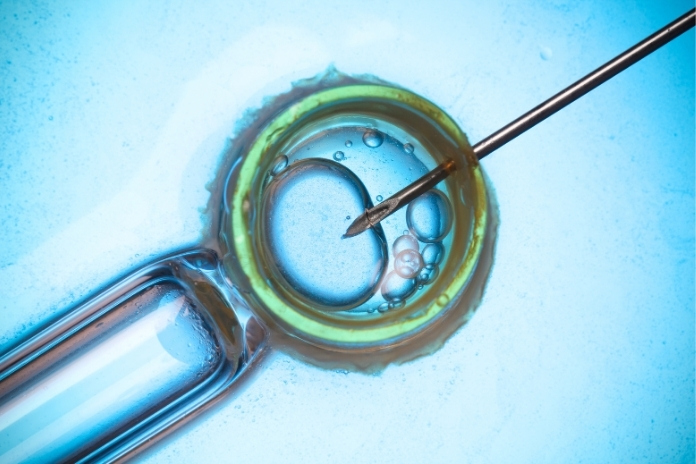
Trying to conceive can be challenging, and more so if you do not know certain basics about fertility. We all know that with age, the number of eggs goes down, and this might be scary. However, we often forget to consider the quality of eggs while just focusing on the quantity. You might be doing everything correctly. You monitor your cycle, you eat well, take your prenatal vitamins, and still, month after month, you’re greeted with disappointment. And then there are the fertility tests. Perhaps your AMH is low. Perhaps “diminished ovarian reserve” is mentioned by your doctor. And now you’re riddled with fear. Do I even have enough eggs to get pregnant?
But here’s what they don’t always make clear: you don’t need a hundred eggs—you need one good one.
Though a woman is indeed born with all the eggs she will ever have, and the number and quality of eggs do decrease with age, quality, and not quantity, is usually a determining factor in whether an egg will form a healthy baby.
So, what counts more for getting pregnant: egg quality or quantity? In this article, we’ll understand the science, dispel popular myths, and detail exactly how your egg health affects fertility—and what you can do to boost your chances, regardless of age.
Read More: Can You Get Pregnant During Your Period? What You Need to Know
Understanding the Basics of Female Fertility
To know the right way that helps conceive faster, we must first understand female fertility. Female fertility depends on two key factors:
- Egg quantity (how many eggs are remaining in your ovaries)
- Egg quality (how healthy and genetically normal those eggs are)
Women are born with 1 to 2 million eggs. By the time they reach puberty, that number comes down to around 300,000–400,000. Every menstrual cycle, hundreds of eggs start maturing, but only one is usually released through ovulation. With time, both the quantity and quality of these eggs decrease, particularly after age 35.
This is why so many physicians encourage women to get pregnant before age 35, but it’s not merely about having no eggs left to spare. It’s the higher risk of chromosomal defect, miscarriage, or failure to implant as the quality of the eggs decreases.
What Is Egg Quantity (Ovarian Reserve)?
Egg quantity, or ovarian reserve, is the number of remaining eggs a woman possesses. It is generally measured with:
- AMH (Anti-Müllerian Hormone): Greater AMH indicates a bigger reserve
- Antral Follicle Count (AFC): AFC is an ultrasound that measures small follicles in the ovaries
- FSH and Estradiol: Tested on day 2-4 of the cycle, high FSH can be a sign of lower reserve
Common Misconception: More Eggs = Greater Fertility
Even though it makes sense to think that more eggs equal greater fertility, that’s not always true. You might have lots of eggs (particularly with PCOS) but poor-quality ones. Others with a lower egg count get pregnant easily because their few remaining eggs are good.
Ovarian reserve aids in establishing your conception timeline and directs treatment solutions such as IVF, but egg number does not determine the potential for pregnancy alone.
Read More: Trying to Conceive? The Link Between Vitamin D Deficiency and Infertility
What Is Egg Quality (and Why It’s Crucial)?
Egg quality is the capability of the egg to mature normally, fertilize, grow into a healthy embryo, and implant correctly.
High-quality eggs:
- Have the proper number of chromosomes (euploid)
- Have healthy mitochondria (energy-producing units)
- Can divide and develop into a blastocyst after fertilization
How Age Affects Egg Quality
With age, mitochondrial function decreases, and chromosomal mistakes are more frequent. Over the age of 40, over half of a woman’s eggs can be aneuploid (contain the incorrect number of chromosomes), raising the risk for miscarriage or failed implantation.
Egg Quality and IVF Success
Even with IVF, the quality of the eggs is the single most important factor determining if an embryo will implant and result in a healthy baby. That’s why older women can release more than one egg with IVF, but still have fewer success rates if those eggs are not of high quality.
Egg Quality vs. Quantity: Which Matters More?
Health professionals agree: egg quality wins over quantity when it comes to getting pregnant.
For natural conception, a single healthy egg is enough. Women with poor ovarian reserve but high-quality eggs can conceive naturally.
For IVF, quantity is a plus since more the eggs, greater the chances of getting at least one good one. Even if there are many eggs, pregnancy remains uncertain if their quality is poor.
Read More: Struggling to Conceive? Your Thyroid Could Be the Missing Piece in Your Fertility Puzzle
Age Comparison: 30s vs. 40s

- Early 30s: Egg quantity and quality are usually good; pregnancy rates are optimum.
- Mid-to-late 30s: Egg quality deteriorates; number may start to fall.
- 40+: The Number is low, and the majority of remaining eggs carry chromosomal defects. But here again, a single good-quality egg can lead to a healthy pregnancy.
Can You Improve Egg Quality?
You cannot control how many eggs are left, but studies indicate that you might be able to enhance egg quality with lifestyle, diet, and medical interventions.
Diet and Supplements

- CoQ10: CoQ10 helps fuel mitochondria—the energy source of cells, which may improve egg energy production and development.
- Antioxidants (vitamin C, E, and A): Antioxidants protect eggs from oxidative damage that can impair chromosomal health.
- Prenatal Vitamins: Taking prenatal vitamins during conception and even during pregnancy helps with adequate folate, iron, and B12.
- Omega-3s: Including omega-3-rich foods or supplements lowers inflammation and aids in hormonal balance, making it easier to conceive. You can find omega-3 in flaxseeds, walnuts, and fish oil, an easier option to add to your diet.
Lifestyle Changes

Taking good care of your general health can have a direct influence on egg quality. These are particular ways to do so:
- Sleep Well: Get 7–9 hours of good sleep. Poor sleeping patterns can throw your circadian rhythm into disorder, which causes hormonal problems that disrupt ovulation.
- Take Less Stress: Stress causes constant cortisol spikes, which can interfere with reproductive hormones such as estrogen and luteinizing hormone.
- Avoid Toxins: Smoking and alcohol are both established reproductive disruptors. Toxins in the environment, like BPA (in plastics) and phthalates, can also damage egg quality.
- Moderate Exercise: Regular exercise promotes blood flow to reproductive organs, but too much exercise (particularly without proper nutrition) can reduce fertility. Try 30–45 minutes of moderate activity 4–5 times a week.
Medical Options

If lifestyle and diet modification fail to get you results, or if age and test results need you to take quicker action, medical interventions can be used:
- IVF with PGT (Preimplantation Genetic Testing): This permits physicians to test embryos for chromosomal disorders before implantation, raising the chances of a successful pregnancy.
- Egg Freezing: Women in their 30s may freeze eggs while quality remains good, to use later.
- Hormonal Therapy: DHEA or growth hormone supplements are occasionally used to supplement egg growth in women with decreased ovarian reserve, although evidence is only just becoming available.
What to Do If You Have Low Reserve or Poor Egg Quality

Facing low ovarian reserve or concerns about egg quality can be incredibly disheartening, especially when you’re doing everything to conceive. But having less number of eggs or even diminished egg health doesn’t necessarily mean the end of the road. Today, we have advances in reproductive medicine and a better understanding of fertility science, but there are still multiple paths to parenthood.
The following are the signs that you need to see a fertility specialist, what your choices are, and how to emotionally and physically deal with this process.
When to See a Specialist:
If you are older than 35 and/or have:
- Irregular cycles
- History of miscarriage or unsuccessful IVF
- Low AMH or AFC
Treatment Options
- IUI: Intra-Uterine Insemination (IUI) has helped several couples conceive despite the low egg count. However, it can work if ovulation is consistent and the tubes are in good shape.
- IVF: In Vitro Fertilization (IVF) has become extremely popular, with millions of couples trying it for parenthood. It enables multiple egg retrieval and screening, ultimately helping you conceive.
- Donor Eggs: In women with significantly less egg reserve or low-quality eggs, donor eggs are used, which help them conceive.
Emotional Support:
Infertility struggles are emotionally draining. Counseling, support groups, or even just discussing with others who have been through it can prove to be invaluable.
Timing Ovulation:
Use LH kits to monitor ovulation and time sex during your fertile period—very critical when the number of eggs is low.
When to Consider Fertility Testing
You would want to test early if you:
- Are over the age of 35 and seeking to conceive
- Have irregular periods or PCOS
- Have had ovarian surgery earlier or have undergone chemotherapy
- Been trying for over 6 months with no results
Critical Tests to Know Egg Health:
- AMH: Gives ovarian reserve
- AFC: Assesses follicles present for that cycle
- FSH and Estradiol: Can show how much your body is struggling to ovulate
- Ultrasound and Hormone Panels: Evaluate cycle health and reasons for infertility
FAQs
Can you still have a natural conception with a low egg number? Yes—if your remaining eggs are of good quality and ovulation is normal.
- How do I know if my eggs are healthy?
There is no specific test, but age, AMH, AFC, and response to IVF can provide clues. IVF embryo development also indicates egg quality.
- Is IVF success related more to egg quality or quantity?
Both are important, but quality is more important. You only need one chromosomally normal embryo to conceive.
- How many eggs does a female need to become pregnant?
Just one good egg. IVF tries to achieve multiple eggs to raise the chances, but natural conception needs only one good ovulation.
Key Takeaway: It’s One Good Egg, Not a Dozen

Fertility is not a numbers game. Though egg number may influence your reproductive timeline, it’s egg quality that decides your capacity to conceive and carry a healthy pregnancy.
The better news? Most women with low ovarian reserve still get pregnant. The secret is early detection, lifestyle adjustment, and seeking proper medical counsel.
So if you’re concerned about your numbers, remember, you don’t require a dozen ideal eggs. You just need one good one.
References
- https://pmc.ncbi.nlm.nih.gov/articles/PMC7558284/
- https://fertilityfoundation.in/how-many-eggs-are-needed-for-ivf/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC3671549/
- https://www.cnyfertility.com/how-many-eggs-do-women-have/
- https://www.orangehealth.in/anti-mullerian-hormone-test
- https://www.careivfkolkata.com/Evaluation/AntralFollicleCount
- https://www.prathamivf.com/egg-quality-vs-embryo-quality-what-matters-more-for-ivf-success.php
- https://www.garbhagudi.com/blogs/the-role-of-ovarian-reserve-testing-in-fertility
- https://www.cloudninefertility.com/blog/natural-conception-with-low-amh-levels
- https://www.ayaanshhospital.com/egg-quality-vs-quantity-amh-isnt-everything/
In this Article