When people hear palliative care for dementia patients, many still assume it means “nothing more can be done.” In dementia, this misunderstanding causes real harm. Care is often delayed until the very end, even though dementia is a long, progressive illness where comfort, dignity, and decision-making matter years before the last stage.
Dementia does not behave like cancer or heart failure. There is no clear turning point. Decline is uneven, unpredictable, and emotionally exhausting for families. As the disease progresses, people with dementia face pain they cannot explain, fear they cannot name, sleep that becomes broken, and behaviours that look “difficult” but are actually distress signals.
Palliative care fits this reality, not because death is near, but because life is changing.
This article looks at palliative care in dementia from a practical, grounded lens: what it really is, when it actually helps, and why waiting “until later” is often the biggest mistake.
What Is Palliative Care?

Palliative care is specialised medical care focused on comfort, function, and quality of life for people living with serious illness. It runs alongside ongoing treatment. It does not replace doctors, neurologists, or medications.
In dementia, palliative care is less about machines and more about everyday suffering that often goes unnoticed:
- Pain that cannot be described
- Agitation without a clear cause
- Repeated hospital visits that worsen confusion
- Feeding difficulties
- Emotional burnout of caregivers
Importantly, palliative care is not limited by prognosis. It is based on need, not timelines.
Why Dementia Patients May Benefit From Palliative Care
Dementia is a progressive and life-limiting condition. But unlike cancer or heart failure, it progresses slowly and unevenly. Dementia slowly removes the patient’s ability to explain discomfort. As language fades, suffering often increases, not because symptoms worsen, but because they are missed.
Dementia palliative care helps bridge this gap.
1. Hidden suffering in dementia
Many of the ways dementia patients suffer are not accidental. They are shaped by how dementia itself is viewed.
“The ways in which dementia is stigmatized are not exclusive to long-term care,” says geriatrician Dr. Allen Power. “They reflect broader societal paradigms and patterns.”
As a result, many dementia-related problems are mistaken for “just part of the disease”:
- Restlessness may be due to untreated pain
- Refusal to eat may be due to swallowing difficulty
- Aggression may be fear or overstimulation
- Repeated infections may reflect care burden, not weak immunity
Palliative teams are trained to interpret behaviour as communication, not misbehaviour.
2. Dementia affects the whole system
Dementia is not only memory loss. It affects:
- Mobility
- Bladder and bowel control
- Sleep cycles
- Emotional regulation
- Family dynamics
Many of these symptoms are treated reactively, after they cause a crisis. Dementia supportive care through a palliative lens focuses on anticipation rather than reaction.
Instead of asking, “What medicine can we add now?” the question becomes, “What is causing distress, and how can we reduce it safely?”
When Should Palliative Care Start in Dementia?
The honest answer: earlier than most people think. Because there is no fixed stage when palliative care in dementia must begin.
Palliative care is useful once dementia begins to interfere with daily life, not only when the patient is bedridden or non-verbal.
Appropriate times to consider palliative care
- Diagnosis of moderate dementia
- Frequent agitation or distress
- Repeated hospital admissions
- Unexplained weight loss
- Swallowing difficulties
- Caregiver exhaustion or conflict
- Uncertainty about future medical decisions
Waiting until the final stage often means missed chances for comfort, clarity, and planning.
How Palliative Care Helps Dementia Patients
Palliative care in dementia works quietly. It is not dramatic. But its impact is deep.
1. Better symptom control
Pain in dementia is commonly under-treated. Palliative teams assess pain using behavioural symptoms, posture, sleep, and facial cues, not words alone.
They also manage:
- Breathlessness
- Constipation
- Pressure sores
- Anxiety
- Sleep disturbances
Small adjustments often bring disproportionate relief.
2. Fewer harmful interventions
Hospital environments are disorienting for dementia patients. Palliative care helps reduce:
- Unnecessary ICU admissions
- Repeated IV lines and tests
- Aggressive treatments with minimal benefit
The goal is not “doing less,” but doing what actually helps.
3. Preserving dignity
As abilities decline, dignity becomes fragile. Palliative care focuses on:
- Respectful hygiene care
- Privacy
- Gentle handling
- Avoiding restraints whenever possible
These details matter deeply, even when patients cannot express them.
How Palliative Care Supports Families and Caregivers
Dementia does not affect one person. It slowly reshapes the entire household.
Caregivers often struggle with:
- Guilt over decisions
- Confusion about disease progression
- Emotional fatigue
- Fear of “doing the wrong thing”
Palliative care provides structured guidance. Palliative care supports caregivers in ways routine care often ignores.
1. Emotional validation
Families are allowed to say:
- “I am tired.”
- “I don’t know what is right anymore.”
- “I feel guilty.”
These feelings are normal, not failure.
2. Decision support
Palliative professionals help families navigate questions like:
- Should we hospitalise again?
- Is tube feeding helping or harming?
- When is comfort more important than prolonging life?
These are not medical decisions alone. They are value decisions.
3. Reducing conflict
Disagreements between siblings or relatives are common. A neutral palliative team often helps align everyone around the patient’s best interest.
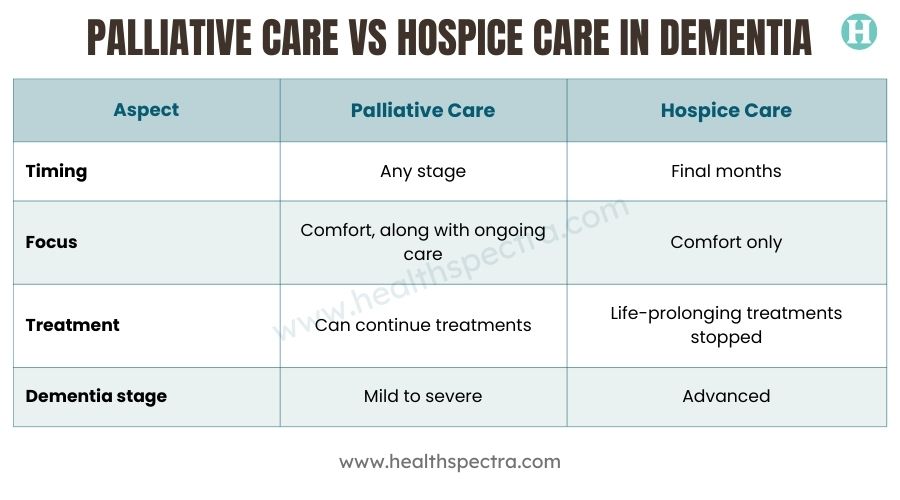
Palliative Care vs Hospice Care in Dementia
This confusion delays care more than anything else. Many families worry that accepting palliative care means abandoning treatment, when in reality, the shift is guided by quality of life, not by labels or timelines.
“It’s really about focusing on someone’s quality of life and having the best number of good days possible alongside getting ongoing treatment,” says Dr. Alexis Drutchas, a palliative care physician. “When patients reach a point where treatment-directed therapies are no longer helping, or are causing more harm than benefit, and their quality of life is no longer acceptable, that’s when the focus may shift fully to comfort, which is the transition to hospice.”
Many dementia patients receive hospice care too late. Palliative care fills the long gap before that stage.
What a Palliative Care Team Looks Like

Palliative care is not one doctor. It is a team approach.
Typically includes:
- Doctors and nurses trained in symptom management
- Social workers to address family and care planning issues
- Mental health professionals for emotional support
- Spiritual care providers, if the family wishes
Their role is coordination as much as treatment, making sure care aligns with reality, not just protocols.
Advance Care Planning and Dementia
Dementia removes decision-making capacity gradually. This makes early planning essential.
1. Why early planning matters
Once advanced dementia sets in, the patient can no longer express:
- Treatment preferences
- Comfort priorities
- Acceptable quality of life
Families are then forced to guess, often under stress.
2. What should be discussed early
- Hospitalisation preferences
- Feeding options
- Resuscitation decisions
- Comfort-focused care goals
Palliative care facilitates these conversations before crisis forces them.
Read More: 15 Engaging Activities for Dementia Patients That Stimulate Memory and Boost Mood
Common Concerns About Palliative Care in Dementia
1. “Does this mean we are giving up?”
No. It means shifting focus from cure to care.
2. “Will medications be stopped?”
Only those causing harm or offering no benefit.
3. “Is palliative care only for the last stage?”
Absolutely not. In dementia, it is most effective before the last stage.
4. “Will this reduce life expectancy?”
Evidence suggests that appropriate palliative care may actually reduce complications and improve overall stability.
Read More: Do People with Dementia Know They Have It? What Awareness Looks Like at Different…
How to Access Palliative Care for a Dementia Patient
Access varies, but common routes include:
- Referral from a neurologist or a physician
- Hospital-based palliative clinics
- Home-based palliative services
- Long-term care facilities
If you are unsure, simply asking “Is palliative care appropriate now?” is often enough to start the process.
Read More: Early Signs of Dementia in Women: What to Watch for and When to Seek…
When to Seek Additional Medical Help
Palliative care does not replace urgent care. Immediate medical attention is needed if there is:
- Sudden change in consciousness
- Severe breathing difficulty
- Uncontrolled pain
- New neurological symptoms
Palliative teams work alongside emergency services when required.
Read More: Vascular Dementia End-of-Life Symptoms: What to Expect and How to Provide Comfort
Final Thoughts
Dementia changes life slowly, then suddenly. Palliative care helps families adapt to this reality without losing compassion, dignity, or clarity. It is not about preparing for death. It is about protecting life as it is lived now, even when memory fades.
Earlier involvement does not shorten the journey. It often makes it gentler.
- Dementia-related suffering is often invisible; palliative care helps interpret it.
- Waiting until advanced stages delays meaningful comfort.
- Behavioural symptoms are often distress signals, not “just dementia.”
- Families need as much care as patients
- Palliative care reduces unnecessary medical interventions.
- There is limited long-term data on early palliative integration in non-cancer dementia, especially in community settings; this remains an underexplored area.
FAQs
1. Is palliative care suitable for early dementia?
Yes. Early involvement helps with planning and symptom management.
2. Can palliative care be given at home?
Often yes, depending on service availability.
3. Does palliative care stop dementia medications?
Not automatically. Each medication is reviewed individually.
4. Who pays for palliative care?
Coverage depends on the healthcare system and provider. Many services are included under standard medical care.
5. Can palliative care continue for years in dementia?
Yes. Dementia is a long illness, and palliative care can be long-term.
References
- Charly, D., Bhardwaj, S., & Issac, T. G. (2025). Integrating Palliative Care in Dementia in India: How Long Can We Afford to Wait? Indian Journal of Psychological Medicine.
- Malhi, R., McElveen, J., & O’Donnell, L. (2021). Palliative Care of the Patient with Dementia. Delaware Journal of Public Health, 7(4), 92–98.
- MedlinePlus. (2018). What is palliative care?: MedlinePlus Medical Encyclopedia. Medlineplus.gov.
- World Health Organization. (2020, August 5). Palliative Care. World Health Organization.
In this Article