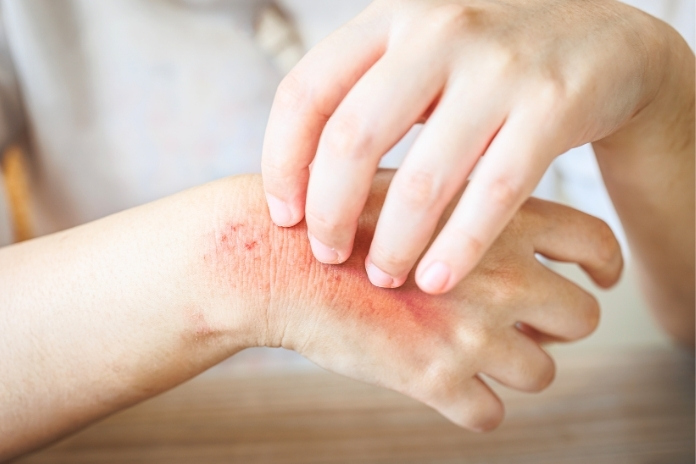
Fungal infections rank among the most common skin and mucous membrane conditions worldwide. And for many, they are not a one-time issue. It can be a recurring athlete’s foot every rainy season, a vaginal yeast infection every few months, and that stubborn nail fungus. It always seems impossible to resolve these fungal infections.
The truth is clear: fungi love warm, moist, and enclosed environments. The human body offers the right conditions for development. Infections return because one or more of the deep-seated triggers have remained in place, allowing the fungus to take hold, re-infect, or resist treatment.
This article breaks down why fungal infections keep coming back, the medical reasons behind the causes of chronic fungal infections, and the symptoms of recurrence. We will also learn about the most effective evidence-based treatments and practical lifestyle steps to finally break the cycle.
Common Types of Recurrent Fungal Infections

Not all fungal conditions tend to return repeatedly. However, these six are especially known for recurrence:
Tinea Pedis (Athlete’s Foot):
This fungus grows well in sweaty socks, tight shoes, locker rooms, and moist floors. The athlete’s foot usually recurs because the shoes have not been disinfected or the feet may be wet for a long time. Reinfection from socks, bathroom floors, and unwashed mats is very common.
Tinea Cruris (Jock Itch):
This fungal infection usually affects the inner thighs and groin. It does tend to recur, as this area tends to trap heat and sweat, particularly if synthetic underwear or tight-fitting clothes are worn consistently.
Tinea Corporis (Ringworm):
Despite the name, ringworm has nothing to do with worms. It is easily spread via clothes, bedding, pets, and gym surfaces. Recurrence usually points to incomplete treatment or continued environmental contamination.
Yeast Infections (Candida):
Yeast infection is associated with the use of antibiotics, blood sugar malfunctions, hormonal changes, and weak immunity. Candida tends to flourish whenever there is moisture that remains entrapped.
Onychomycosis (Nail Fungus):
Nail fungus often becomes chronic, since nails grow slowly and treatment is long and cumbersome. Shoes and socks sometimes act as reservoirs, frequently reintroducing the fungus.
Fungal Scalp Infections (Tinea Capitis)
Fungal scalp infection is more common in children, but it may also affect adults. It is spread by combs, hats, pillows, and close contact. Recurrence may be due to treatment failure or reinfection from hair tools.
Read More: At Home Fungal Skin Infection Treatment – 10 Natural Remedies That Work
Why Fungal Infections Become Chronic or Recurrent

Recurring fungal infections don’t just pop up out of the blue. They usually indicate a combination of biological, lifestyle, and environmental factors at play. Let’s take a closer look at why they keep coming back:
Moisture, Sweat & Heat
Fungi thrive in conditions of warmth and moisture. Certain parts of the body, such as the feet, groin, armpits, folds of the skin, and underneath the breasts, are ideal for fungal growth. These regions have a natural tendency to accumulate sweat. If the sweat stays for long, here’s what can happen:
- The skin becomes softer, allowing fungi to easily enter the skin.
- Fungus grows with moisture.
- Skin folds create a closed environment where the fungus multiplies rapidly.
That is why athlete’s foot, jock itch, and skin fold fungal infections keep recurring, especially in humid climates.
Not Completing Treatment

A common cause for fungal infection recurrence is stopping the oral or topical antifungal once the symptoms go away. The visible rash may go away, but the microscopic fungal spores remain alive underneath.
Incomplete treatment results in:
- Hidden fungal reservoirs
- Temporary relief followed by flare-ups
- Treatment-resistant strains over time
Reinfection From the Environment

You can treat the fungal infection on your body, but if fungal spores remain in the environment, they can lead to an infection.
Common sources of reinfection include:
- Unwashed socks or sweaty shoes
- Towels that are reused more than they should be
- Sheets not washed in hot water
- Gym equipment
- Loofahs that are damp host
- Nail clippers, pumice stones, or combs
This environmental cycle is one of the top reasons why chronic fungal infections become difficult to eliminate.
Poor Immune System
A weak immune system makes fighting the fungal organisms more difficult. Risk factors include:
- Diabetes
- HIV
- Cancer therapies such as chemotherapy and radiation
- Steroid medications
- Autoimmune disorders
These conditions weaken the body’s ability to control fungal overgrowth, resulting in persistent or recurrent fungal infections and requiring prolonged treatment.
Diabetes & High Blood Sugar

Fungus, especially Candida, prefers high-sugar environments. High blood sugar results in increased moisture and a very conducive environment where fungus can thrive, especially between folds of skin and the genital area.
Poorly controlled diabetes also delays the healing of skin, delaying healing.
Antifungal Resistance
Like bacteria, fungi can develop resistance when:
- Antifungals are used incorrectly.
- There is an inconsistent treatment.
- Topical and oral medications are overused.
Resistance to antifungal agents makes the infection difficult to treat and can lead to relapse time after time.
Tight Clothing & Low-Breathability Fabrics

Synthetic fabrics can trap heat and moisture, creating fungal-friendly environments around the groin, thighs, and feet.
Hormonal Factors
Estrogen fluctuations affect vaginal flora. Recurrent yeast infections often spike during:
- Pregnancy
- Perimenopause
- While taking high-estrogen birth control
- Hormone replacement therapy
High Antibiotic Use
Antibiotics kill off good bacteria from your gut and vagina. Your natural microbiome gets imbalanced, allowing Candida to take over. This leads to the recurrence of yeast infection.
Read More: What Happens to Your Body When You Wear Tight Clothes Every Day
Symptoms That Suggest a Recurrent or Persistent Fungal Infection
You may suspect a fungal infection is recurring if:
- Symptoms improve initially but return within weeks
- Itching or burning continues despite treatment
- Skin redness, peeling, cracking, or circular rashes
- Nails become thick, brittle, yellow, or crumbly
- The feet or groin develop a persistent odor
- Vaginal discharge recurs repeatedly
- Appear cyclically or flare with increased sweating
You must visit your doctor if recurrence is more than 3–4 times a year. That is a sign of an underlying issue that needs evaluation.
How to Break the Cycle — Evidence-Based Strategies
Let us learn how to finally put a stop to fungal infections through treatment, change in lifestyle, and environmental control.
Fully Treat The Infection
Most fungal infections require:
- At least 2–6 weeks of topical treatment.
- Longer treatment for nails, scalp, and chronic cases.
- Oral antifungals for when topical therapy isn’t enough.
For the therapy of nail and scalp infections, repeated doses or long-term treatment are usually needed, as the fungus is deeply embedded within the tissue.
Keep Skin Clean, Dry & Cool
It interrupts the exact conditions that the fungus requires to survive.
Best practices include:
- Shower after much sweating or workouts.
- Dry thoroughly, especially between toes and in skin folds.
- Use antifungal powders when very sweaty, especially in shoes or groin areas.
- Apply medicated powders in humid weather.
Improve Hygiene Habits
Hygiene habits can significantly impact treatment success.
You must:
- Change socks daily, or twice a day if sweaty.
- Use cotton towels and wash them often.
- Replace loofahs every 3–4 weeks.
- Avoid sharing personal items.
Try to avoid:
- Reusing damp towels
- Wearing sweaty socks or shoes from the previous day
- Ignoring sweaty garments after working out
Treat the Environment
You need to get rid of the fungal spores in your environment in order to avoid re-infection. Steps that make a significant difference:
- Wash bed sheets in hot water every week.
- Sun-dry towels and bed linens whenever possible.
- Air out shoes for 24–48 hours.
- Spray the interior of shoes with antifungal solutions.
- Disinfect nail tools, razors, and shower floors.
Clothing Choices Matter
Clothing is one of the leading causes of excessive moisture, more than most individuals could imagine. Here are a few tips to opt for the right kind of clothes to prevent recurrent fungal infections.
Choose:
- Loose, breathable cotton underwear
- Moisture-wicking fabrics for workouts
- Socks made from cotton or bamboo
Avoid:
- Nylon, polyester, or tight fitness leggings
- Tight jeans or underwear that retain heat
Manage Blood Sugar
Managing blood sugar is key for individuals with diabetes. Good glycemic control can:
- Reduce recurrent yeast infections
- Improve healing
- Reduce moisture in skin folds
- Help restore normal immunity
Enhancing Immunity
A strong immune system protects your skin barrier. Focus on:
- Balanced nutrition
- Adequate protein
- Good sleep
- Managing stress
- Exercising regularly
These are not medication substitutes but are crucial to prevent relapse.
Avoid Triggering Products
Harsh chemical products disrupt the skin microbiome.
Avoid:
- Feminine washes
- Scented soaps
- Powerful detergents
- Peroxide-based cleansers, unless medically advised
Mild, pH-balanced cleansers maintain healthy skin flora.
Read More: Rotating Your Shoes: Why Switching Pairs Can Improve Foot Health and Performance
Treatment Options-Medical and OTC
Here are a few doctors’ recommendations, based on the type of infection and the severity:
Topical Antifungals
Common over-the-counter antifungal options include:
- Clotrimazole
- Terbinafine
- Ketoconazole
These work well for mild to moderate infections.
Oral Antifungals
Prescribed for stubborn, deep, or recurrent cases:
- Fluconazole
- Itraconazole
- Terbinafine
It must be used under a doctor’s supervision because it can adversely affect the liver.
Probiotics for Yeast Infections
Although evidence is mixed, some people find relief after using the following:
- Lactobacillus strains
- Probiotic vaginal suppositories
They can help restore healthy vaginal flora.
When Combination Therapy Is Needed
Nail fungus, scalp infections, and chronic ringworm often need:
- Topicals, along with oral medications
- Treatment of the environment
- Longer treatment cycles
Always consult with your health provider before starting any antifungal medication.
When to See a Doctor (Red Flags)

Dr Vijay Zawar, the immediate past national president of the Indian Association of Dermatologists, Venereologists and Leprologists (IADVL), emphasized the importance of early consultation. “Fungal infections are a common occurrence in summer. However, people often delay seeking professional help from a dermatologist, leading to potential complications,” said Dr Zawar.
Fungal infections are common, and sometimes they recur as well. However, you must consider visiting a doctor if:
- The infection lasts for more than 3–4 weeks despite treatment.
- You develop severe cracking or open wounds.
- There are signs of bacterial infection, such as pus, fever, and spreading redness.
- You have ‘’uncontrolled diabetes.’’
- You get more than four vaginal yeast infections in a year.
- Medication causes reactions.
- Nails become painful or distorted.
- The rash spreads rapidly.
These could indicate a deeper issue that requires medical intervention.
Quick Review
Recurring fungal infections are due to:
- Moisture and heat
- Incomplete treatment
- Poor hygiene habits
- Environmental contamination
Your fungal infections keep coming back due to several factors. These include diabetes and hormonal changes, poor immunity, and antifungal resistance. Breaking the cycle requires a full treatment plan, better hygiene practices, environmental cleaning, and attention to underlying risk factors. If infections persist, seek out immediate medical attention. You must consult a healthcare professional to rule out deeper causes and start the right treatment strategy.
References
- Tata AIG. (n.d.). Fungal diseases: Types, symptoms, and treatment. Tata AIG
- McGraw-Hill Education. (n.d.). Topical antifungals. In AccessMedicine
- Efficient Labs. (n.d.). Can your clothes cause skin fungus? Here’s what you need to know
- Author(s) not listed. (2024). Fungal infections: A comprehensive clinical update. National Center for Biotechnology Information (NCBI)
- Max Healthcare. (n.d.). Fungal infection: Types, symptoms, and causes. Max Healthcare
- Interpod Orthotics. (n.d.). What is tinea pedis (athlete’s foot)? Diagnosis, treatment, and pain relief
- World Health Organization. (n.d.). Ringworm (tinea)
In this Article