There’s a strange pattern in prenatal nutrition: some nutrients receive great attention, others are acknowledged briefly, and some, like choline, are barely mentioned unless you meet a nutrition researcher or a very detail-oriented obstetrician.
Most women know about folic acid even before pregnancy. Iron becomes mandatory. Calcium and vitamin D get enough emphasis. Omega-3 is discussed depending on who you ask.
But choline? How much choline for pregnancy? Is it really needed?
For many expecting mothers, the reaction is simply:
“I’ve never heard of it.”
This lack of awareness is not their fault. Choline wasn’t included in prenatal guidelines for years. The food industry rarely fortifies products with it. Even today, a surprising number of prenatal vitamins contain only 10–60 mg, nowhere close to what an expecting body needs.
Yet inside the body, quietly, choline is working as essential as oxygen supply and protein formation. It is part of building the baby’s brain, spinal cord, memory circuits, liver function, stress regulation, and even how genes express themselves.
So yes, it is the time when choline stopped being an invisible nutrient in pregnancy.
Key Takeaways: What You’ll Learn
- Choline is critical for the baby’s brain, neural tube, and long-term memory pathways.
- Pregnant women officially need 450 mg/day, but research suggests many benefit from a slightly higher intake.
- Most women don’t meet requirements through diet alone.
- Eggs, meat, fish, soy, beans, and certain vegetables provide useful amounts; vegetarians may need careful planning.
- Supplements are helpful for some, but not automatically necessary.
What Is Choline and Why Is It Important in Pregnancy?
If we simplify it, choline is a building material.
Dr. Taylor C. Wallace, Professor of Nutrition at George Mason University, explains that choline isn’t just “one more vitamin” on a list. “It’s woven into so many things the body does,” he says. “Your liver, your muscles, your brain, your mood, everything uses choline in some way. It’s part of the membranes of every cell, and it helps with repairing them too.”
His point is simple: choline quietly supports dozens of processes we don’t usually think about, which is why pregnancy increases the demand for it.
It helps create:
- cell membranes
- neurotransmitter acetylcholine (memory, focus, muscle movement)
- fat transport chemicals
- methyl groups that influence gene expression (gene activity)
During pregnancy, the demand increases because you are not just maintaining your cells; you’re building another human from the very earliest stage.
Two systems especially depend on choline:
- The baby’s brain and spinal cord
- Your liver and placenta
Without enough available choline, the body has to compromise at some level. The fetus usually receives greater importance, which means the mother’s metabolism bears the stress.
That’s why low choline intake in pregnancy has been linked with:
- Higher risk of fatty liver during pregnancy
- less optimal fetal brain development
- Higher neural tube defect (spine-brain issues) risk (especially when folate intake is borderline)
It’s not fear-based messaging. It’s physiology.
How Much Choline Do You Need During Pregnancy?
Here is how much choline is officially recommended during pregnancy:
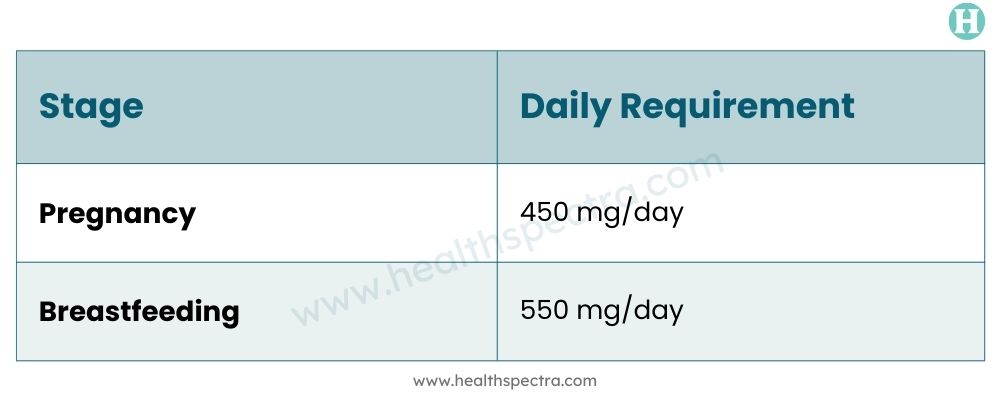 Dr. Wallace points out that the need doesn’t drop after the baby is born. “During breastfeeding, the body will pull from the mother’s own choline stores to make sure the baby gets what it needs,” he says. “So the demand actually goes up.”
Dr. Wallace points out that the need doesn’t drop after the baby is born. “During breastfeeding, the body will pull from the mother’s own choline stores to make sure the baby gets what it needs,” he says. “So the demand actually goes up.”
However, multiple controlled studies explored intakes around 900–930 mg/day. Babies of mothers consuming higher choline showed:
- better memory processing
- healthier stress response
- more efficient brain signaling markers (brain activity signs)
We don’t have enough long-term population data to rewrite official numbers yet—but many experts now say the ideal intake may be above the minimum threshold, especially in the second and third trimesters.
So a simple way to think about it:
- 450 mg/day means minimum.
- A dose of 550–900 mg/day is potentially optimal.
Best Food Sources of Choline

Most people never calculate nutrition while eating. Here’s the practical breakdown:
Top High-Choline Animal Sources
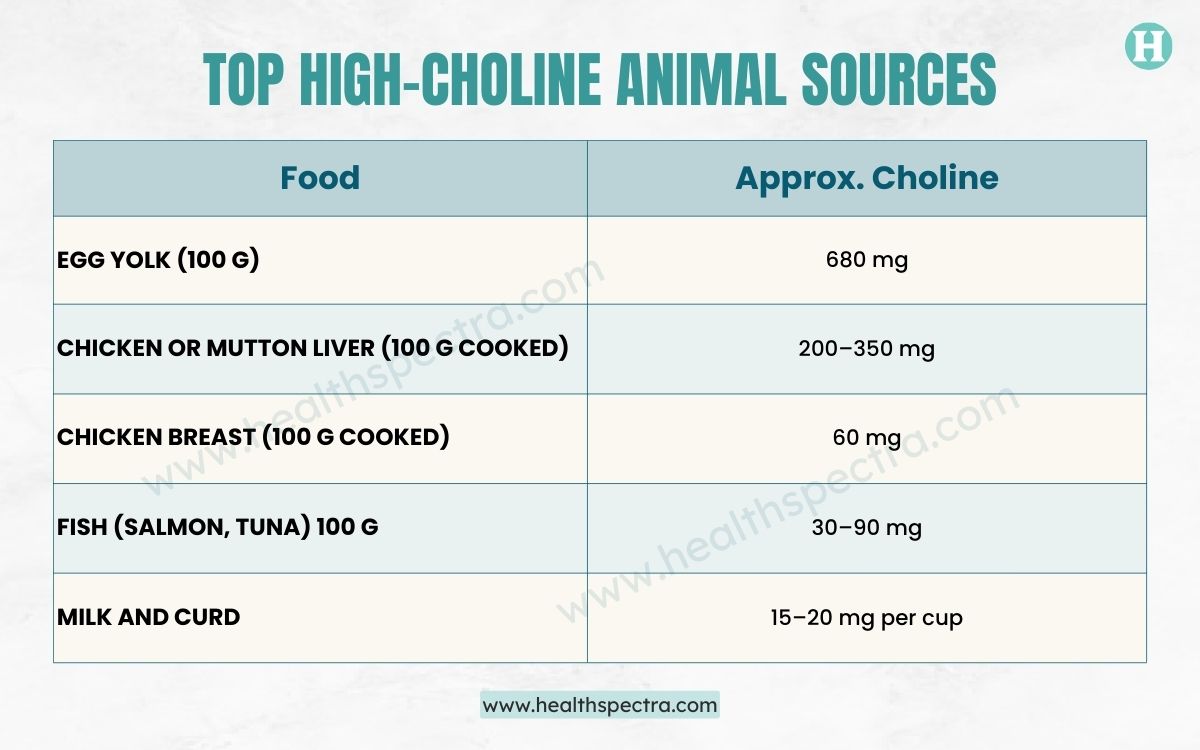 A pregnant woman eating 1–2 eggs a day, along with occasional fish or poultry, generally meets a large portion of the requirements.
A pregnant woman eating 1–2 eggs a day, along with occasional fish or poultry, generally meets a large portion of the requirements.
Plant-Based/Vegetarian Sources
Plant sources contain less amount, so consistency matters:
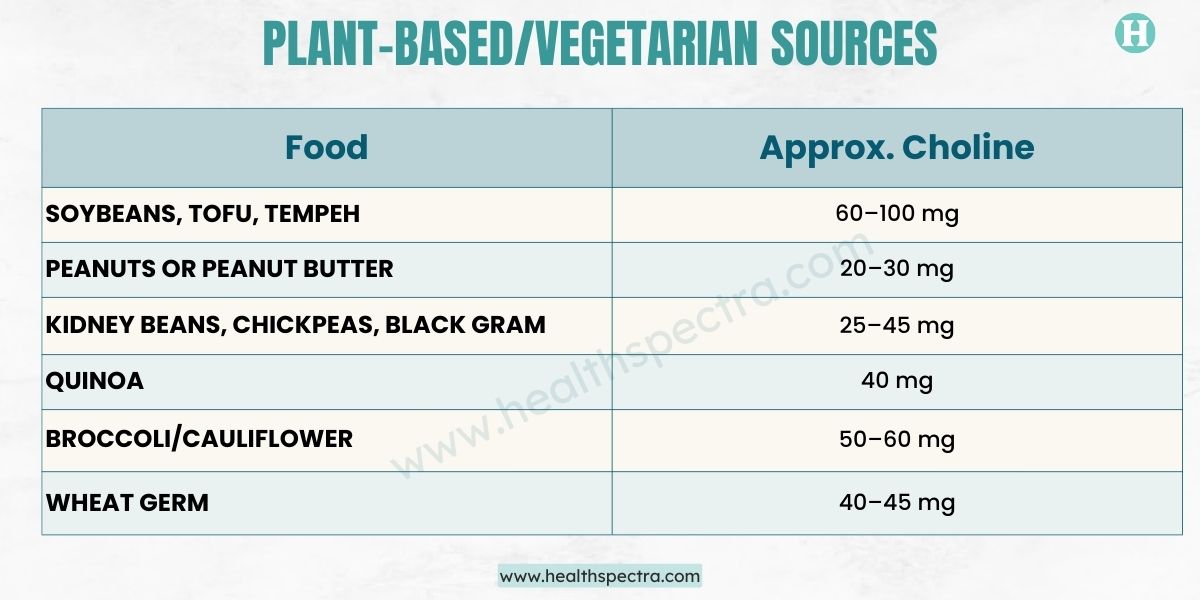 Vegetarians can meet the requirement, but need variety and awareness. Vegans often struggle unless they consciously add supplements or fortified foods.
Vegetarians can meet the requirement, but need variety and awareness. Vegans often struggle unless they consciously add supplements or fortified foods.
Read More: Dry Eyes in Pregnancy? Here’s Why It Happens and How to Relieve It
Should You Take a Choline Supplement During Pregnancy?
There’s no universal rule.
A supplement becomes reasonable if:
- You don’t eat eggs or animal foods.
- Food aversions limit protein-rich meals.
- You already take a prenatal multivitamin without choline.
- You have gestational diabetes, fatty liver, or prior neural tube defect risk.
Dr. Varsha Gorey, Senior Clinical Dietitian, puts it simply: “Try to get choline from food first. Most women can do that without much effort if they’re eating eggs, pulses, curd, or soy.”
Then she adds, “Supplements are only for people who genuinely need them, like vegetarians, women with food aversions, or if your diet is very limited. And don’t assume your prenatal has enough choline; many don’t. Always check the label and ask your doctor before starting extra.”
Some prenatal products label it as:
- Choline bitartrate
- Phosphatidylcholine
- Alpha-GPC (less common)
Supplements typically offer 100–300 mg per serving, so food still plays a major role.
Before supplementing, reviewing actual intake is smarter than blindly adding pills.
Dr. Wallace adds that women who don’t eat much meat, eggs, or dairy should continue paying attention to choline even after pregnancy and lactation. “If your diet is mostly plant-based, a small supplement can still help,” he says. “But honestly, don’t stress about hunting for the ‘perfect’ choline supplement for pregnancy. The bigger focus should be on getting choline-rich foods during pregnancy, into your meals every day.”
Read More: Pregnancy Guilt and Emotional Overwhelm: What’s Normal and What’s Not
Benefits of Adequate Choline During Pregnancy

1. Supports Baby’s Brain and Memory
Choline contributes to the development of synapses and the hippocampus (memory center). Research suggests that adequate choline intake may improve attention span and learning ability later in childhood.
2. Aids Neural Tube Development
Choline works alongside folate in pathways influencing neural tube closure. It does not replace folate; it complements it.
3. Protects Maternal Liver and Placenta
Choline helps transport fats properly. Without enough fat accumulation may increase the risk of fatty liver during pregnancy, which can affect both the mother and the fetus.
4. May Reduce Stress Hormones in the Fetus
Some studies indicate that choline influences cortisol response. Babies exposed to adequate choline may have a healthier stress response, meaning lower reactivity and better regulation.
Read More: Missed Period but Negative Pregnancy Test: What Could It Mean?
Signs You May Not Be Getting Enough Choline

Choline deficiency during pregnancy does not show dramatic symptoms at first. But possible indicators include:
- Persistent fatigue
- Muscle cramps or weakness
- Poor appetite or slower weight gain during pregnancy
- Elevated liver enzymes
- Memory or concentration issues
- Fatty liver diagnosed on scan
These symptoms can overlap with other conditions, so they are not diagnostic; they are only clues.
Read More: Dark Chocolate During Pregnancy: Benefits, Risks, and How Much Is Safe
Safety and Possible Risks of Too Much Choline
Very high amounts (usually above 3,500 mg/day) may cause:
- Fishy body odor
- Excessive sweating
- Low blood pressure
- Digestive discomfort
Such levels are unlikely unless taking large doses of supplements. Food-based intake rarely leads to excess.
- Choline is essential during pregnancy, especially for fetal brain and neural development.
- Minimum recommended intake is 450 mg/day, but higher intakes may offer additional benefits.
- Eggs, meat, fish, soy, legumes, and broccoli are meaningful sources.
- Supplements may help if dietary intake is insufficient.
- Too much choline is rare but possible with excessive supplementation.
Final Thoughts
Choline does not require overstatement. And you don’t need a perfect diet or complicated planning. Choline only needs recognition.
Not as a trend, but as a nutrient with solid evidence supporting its role in pregnancy and early development.
If you are expecting, planning a pregnancy, or breastfeeding, take a moment to review your diet. Even a small adjustment, such as including an extra egg, a serving of beans, or soy, may help close the nutrient gap.
Small shifts always add up.
FAQs
1. Can I meet my choline needs without eggs?
Yes, but you may need soy products, legumes, fortified foods, or supplements to cover the gap.
2. Is choline the same as folate?
No. They work in related pathways but are separate nutrients, and both are needed.
3. Does cooking reduce choline?
Not significantly. Choline is stable through most cooking methods.
4. Can I take choline supplements with prenatal vitamins?
Yes, but dosage should be reviewed to avoid unnecessary excess.
5. When should I start increasing choline intake?
Preferably before conception or as early in pregnancy as possible—but benefits continue throughout.
References
- CDC. (2024, February 9). Maternal diet and breastfeeding. Breastfeeding Special Circumstances
- Jaiswal, A., Dewani, D., Reddy, L. S., & Patel, A. (2023). Choline Supplementation in Pregnancy: Current Evidence and Implications. Cureus, 15(11), e48538
- National Institutes of Health. (2017). Office of Dietary Supplements – Choline. Nih.gov
- Patterson, K., Bhagwat, S., Williams, J., Howe, J., Holden, J., Zeisel, S., Dacosta, K., & Mar, M.-H. (2008). USDA Database for the Choline Content of Common Foods Release Two Prepared by In collaboration with
In this Article
























