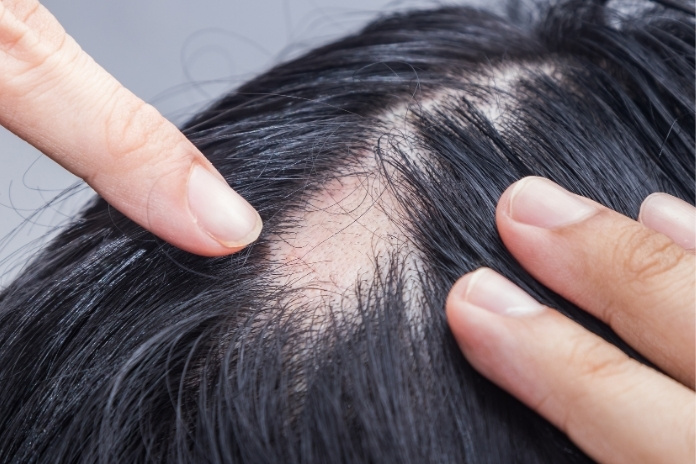
Scarring alopecia, also known as cicatricial alopecia, is an uncommon but serious form of hair loss. This is when the hair follicle is destroyed and replaced with scar tissue. This condition is different from temporary forms of hair loss, where the follicles can recover. Scarring alopecia may lead to permanent hair loss when not treated early.
Although scarring alopecia may affect anyone, it mainly shows in adults. The condition often has a rather quiet course before the development of noticeable hair thinning. Early awareness is important, as timely medical attention may significantly slow down or even prevent further damage to hair follicles.
In this article, you’ll learn what causes it, how to recognize the early warning signs, how doctors diagnose it, the treatment options available, and realistic expectations for long-term management.
What is Scarring (cicatricial) Alopecia?

Scarring alopecia represents a group of disorders characterized by inflammation that gradually destroys the hair follicle, including the stem cell niche and sebaceous gland, and replaces it with fibrous scar tissue. Once such scar tissue has formed, the follicle loses its capacity to regrow.
Scarring alopecia is quite different from the nonscarring hair loss, such as androgenetic alopecia. In this type of alopecia, the follicle shrinks but does not die. In such cases, regrowth is still possible with proper treatment.
You might wonder, ‘why does hair loss become permanent?’ Hair is permanently lost when the “bulge” region of the follicle is damaged. This is the section that contains the stem cells from which hair regenerates, which is destroyed. Once this happens, smooth and shiny patches without follicular orifices develop on the scalp.
Read More: Is It Normal to Lose Hair in the Shower? Here’s When to Worry
Causes & Risk Factors — What Triggers Follicle Destruction

Primary vs Secondary Types
Primary Cicatricial Alopecia
In primary cicatricial alopecia, the inflammation directly attacks the hair follicle, resulting from autoimmune or chronic inflammatory processes. The body’s own immune system mistakenly attacks the follicle, causing slow and progressive loss.
Secondary Cicatricial Alopecia
In secondary cicatricial alopecia, follicles get damaged because of an external event such as severe burns, infections, radiation, or trauma.
Here, scarring does not develop as a result of an internal immune attack but from an external injury that destroys the follicles.
Common Subtypes & Demographics
Here are a few common subtypes of scarring alopecia, including:
Central Centrifugal Cicatricial Alopecia (CCCA):
- CCCA is most common in African women and usually begins at the crown and progresses centrifugally.
- While genetics play a role, certain hair practices may worsen inflammation and progress quickly.
Frontal Fibrosing Alopecia (FFA):
- FFA involves progressive recession of the front hairline and eyebrows, usually affecting post-menopausal women.
- It has a slow-moving but persistent and band-like pattern.
Other Subtypes:
- Lichen Planopilaris is an autoimmune inflammation that can lead to patchy hair loss.
- Folliculitis decalvans is a chronic infection-driven destruction with pustules and crusting.
Risk & Trigger Factors
Genetic Predisposition:
Genetic predisposition occurs especially in CCCA. Genetics make the baseline vulnerable, making the follicles more prone to inflammation. When you reduce lifestyle triggers, this underlying predisposition continues to progress, making early monitoring important.
Hair Care:
Certain hair care practices include tight hairstyles, chemical relaxers, and heat appliances. These are not direct causes of scarring alopecia, but they can promote inflammation in the already genetically predisposed individuals. Repeated traction may irritate the scalp and increase the chances of follicle damage over time.
Underlying Diseases:
Long-term inflammation, diseases, or neglected scalp infections are another cause. Over time, inflammation from lichen planus, lupus, or long-standing folliculitis will slowly damage the structures of the follicle. Early treatment can prevent the chance of permanent hair loss.
Signs & Symptoms — How to Recognize It Early

Early Signs
Itching, Burning, and Stinging:
Symptoms include itching, burning, stinging, or tenderness on the scalp. These sensations often mean an early warning that inflammation is brewing beneath the skin. Consistent discomfort, especially if limited to the same general area, shouldn’t be ignored.
Thinning or Small Bald Patches:
The early thinning may mean stress-related shedding or androgenetic alopecia, but scarring alopecia typically starts with irregular, patchy areas that do not improve despite changes in hair care.
Advanced Signs of Scarring
Smooth, Shiny Scalp:
This could indicate that scar tissue has replaced the follicles, leaving the skin looking polished with little or no texture.
No Visible Follicular Openings:
Dermatologists look for visible follicular openings because they’re one of the clearest ways to distinguish scarring from non-scarring alopecia.
Permanent and Large Bald Patches:
Local follicles are destroyed due to inflammation in the absence of treatment. As more tissue is impacted, lesions begin to grow in the affected region.
Why Timing Matters
Timing is important, as we can easily reduce inflammation at an early stage. Once scarring sets in, follicles cannot be regenerated. Therefore, prompt medical attention is important in saving the remaining hair.
Diagnosis & Evaluation
Clinical Examination & History
Dermatologists take note of scalp symptoms, patterns of progression, and associated diseases such as autoimmune diseases and chronic infections. This helps them differentiate scarring alopecia from temporary or hormonal alopecia.
Dermoscopy & Scalp Biopsy
A biopsy is often essential, which can aid doctors in determining not only the type of inflammatory cells involved but also the stage of disease. This helps guide both diagnosis and treatment choices.
Imaging & Lab Work
These tests may include blood tests to rule out lupus, infections, thyroid disease, or metabolic problems. Imaging is less common but can be performed when deeper tissue involvement is suspected.
Distinguishing from Other Hair Loss Types
This step is critical because missing the diagnosis allows scarring to advance. Non-scarring hair loss preserves follicular openings and has different treatment pathways. Hence, accurate diagnosis can help determine the entire course of management.
Treatment & Management — What Can Be Done
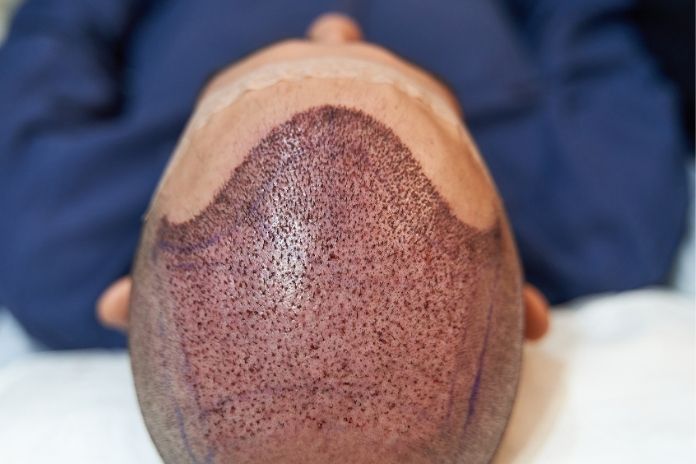
Goals of Treatment
The main goal is preserving what remains, since lost follicles can not regrow. Early and consistent therapy reduces inflammation before permanent scarring has set in.
Hair loss may be a psychologically overwhelming process. Combining medical therapies with cosmetic strategies helps an individual feel more confident while treatment works to stabilize the condition.
Medical Therapies
Anti-inflammatory treatments include topical or injected corticosteroids and topical calcineurin inhibitors. These reduce immune activity around hair follicles, thereby reducing burning, pain, and itch. Steroid injections are particularly helpful for small active patches since medication is delivered directly where the inflammation is strongest.
Systemic medications include hydroxychloroquine, doxycycline, and immunosuppressants.
These are used when there is an extensive inflammation or an aggressive follicular destruction. They act by reducing immune overactivity, slowing further scarring, and are specific to the subtypes.
Hair Restoration & Cosmetic Options
Hair transplant can be considered once the disease has been inactive for 1–2 years. It can restore density in stable cases, but requires careful evaluation since transplanted follicles can fail if inflammation is still active. Due to these possible complications, surgeons look for stability before proceeding.
Wigs, toppers, and scalp micropigmentation provide fast cosmetic results. Many people utilize these in addition to medical treatment to maintain confidence as their symptoms stabilize.
Ongoing Monitoring & Lifestyle Adjustments
Regular dermatology follow-up is essential. Scarring alopecia may flare up unpredictably. Consistent follow-up allows your doctor to catch the inflammation and make treatment adjustments quickly to help prevent new patches from forming.
Avoid practices that irritate or inflame the scalp. Tight braids, heavy friction, or strong chemicals can further exacerbate the tenderness and inflammation, mainly in CCCA.
Switching to a more gentle and low-tension style helps protect fragile follicles. Mild cleansers and non-irritant products care for the scalp. A calm and healthy scalp environment promotes better treatment outcomes. Gentle shampooing, avoiding heavy oils on areas of inflammation, and protection from sunburn can help reduce triggers.
Read More: Healthy Hair, Happy You: Top 8 Hair Growth Supplements for Stronger Locks
Prognosis & Living With Scarring Alopecia: What to Expect
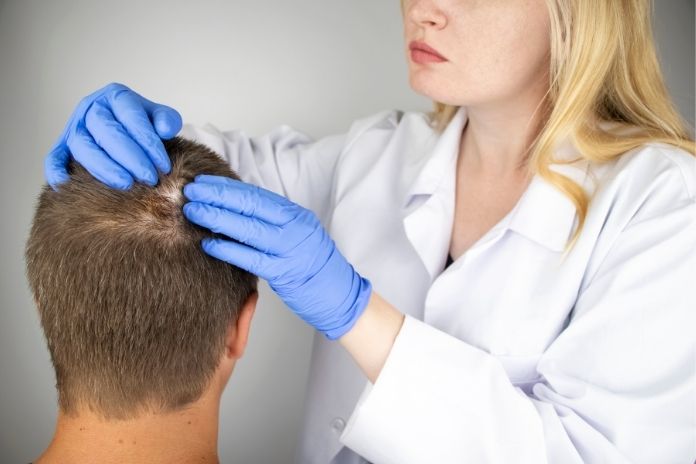
Early treatment may slow or stop the progression, but regrowth is limited once scarring occurs. Some individuals experience stabilization with minimal loss, while others have faster progression depending on the subtype and severity of inflammation.
Emotional & Quality-of-Life Considerations
Permanent hair loss can affect self-esteem, self-assurance, and even social interactions. Reaching out for counselors or support groups may help make the journey smoother.
Prevention & Protective Measures
Although scarring alopecia is not always preventable, the key to keeping as much hair as possible involves early detection. Early recognition of symptoms, prompt evaluation, scalp hygiene, and avoidance of known triggers protect remaining hair.
Read More: How to Naturally Slow Down Age-Related Hair Loss
Quick Summary
Scarring (cicatricial) alopecia is the permanent loss of follicles, so early diagnosis is essential. Treatment is mainly based on halting further loss, with lesser emphasis on the regrowth of hair.
Such conditions may often progress more slowly with timely treatment, and appearance can be maintained through medical and cosmetic options.
FAQs
1. Is scarring alopecia hereditary?
There would seem to be a genetic element in some types, particularly CCCA, where patterns do tend to run in families. However, genes alone don’t guarantee the condition. The onset of alopecia usually needs a combination of genetic predisposition and environmental or inflammatory triggers.
2. Is it possible to regain my hair if I have scarring alopecia?
Hair grows back only in areas where follicles are not yet fully destroyed. Once scarring has already replaced the follicle, regrowth is not possible. Therefore, it is so important to catch the condition early.
3. How long should I wait before considering a hair transplant?
Most specialists recommend a waiting time of at least 1–2 years of complete disease inactivity. This way, the transplanted follicles will not be attacked by ongoing inflammation.
4. Are there certain hair-care practices that I should avoid?
Yes. Avoid tight traction hairstyles, chemical relaxers, frequent heat styling, or anything that causes chronic scalp tension or irritation, especially if you have CCCA or FFA risk factors.
5. What are the signs that my scarring alopecia is “active”?
Burning, itching, stinging, redness, tenderness, and increased shedding near the affected patch generally indicate that there is still underlying inflammation. Dermatologists can confirm this with either dermoscopy or biopsy.
6. Does scarring alopecia affect other body hair?
It’s usually limited to the scalp, but some subtypes, like FFA and LPP, may involve eyebrows, eyelashes, or body hair.
7. Can lifestyle changes help?
Changing one’s lifestyle will not halt scarring alopecia, but it can lessen the triggers. Gentle hair care, avoidance of scalp trauma, early management of autoimmune conditions, and maintaining scalp health help with the treatment results.
References
- https://pmc.ncbi.nlm.nih.gov/articles/PMC12010142/
- https://www.drdivyasharma.com/Scarring-alopecia/
- https://www.mountsinai.org/care/dermatology/services/alopecia-areata/cicatricial
- https://pmc.ncbi.nlm.nih.gov/articles/PMC3855115/
- https://www.aad.org/public/diseases/hair-loss/types/ccca
- https://emedicine.medscape.com/article/1073559-overview
- https://hairfreehairgrow.com/cicatricial-alopecia/
- Al Aboud, A. M., & Tosti, A. (2013). An overview of primary cicatricial alopecia. International Journal of Dermatology, 52(8), 999–1010.
- American Academy of Dermatology Association. (n.d.). Central centrifugal cicatricial alopecia.
- HairFree HairGrow. (n.d.). Cicatricial alopecia.
- Mirmirani, P. (2023). Cicatricial alopecia: Overview. Medscape.
- Mount Sinai. (n.d.). Cicatricial alopecia.
- Sharma, D. (n.d.). Scarring alopecia. Dr. Divya Sharma Dermatology.
- Sulaiman, N., & Bin Saif, G. (2024). Scarring alopecia: Advances in diagnosis and management. Journal of Dermatological Research, 12(3).
In this Article