Bleeding after menopause can be alarming, so alarming that many people immediately worry about cancer. That reaction is understandable, given the seriousness of such a diagnosis, but it’s important to know that postmenopausal bleeding (PMB) isn’t always a sign of something life-threatening. Any vaginal bleeding that occurs 12 months or more after your last period is classified as PMB, and while it always warrants medical evaluation, most causes are benign and often treatable.
Understanding PMB means recognizing that not all bleeding is equal. The amount, timing, and pattern of bleeding, along with other symptoms, can give important clues about the underlying cause. For many women, hormonal changes, thinning of vaginal tissues, or minor infections are responsible. But in some cases, bleeding can signal something more serious, such as endometrial cancer or other gynecologic conditions, making prompt evaluation essential.
This article will guide you through the key aspects of PMB: what qualifies as postmenopausal bleeding, the most common non-cancer causes, warning signs that suggest a more serious problem, and how doctors investigate and treat it. Drawing on expert guidance and the latest clinical evidence, it aims to help women and their healthcare providers navigate this concerning symptom with confidence and clarity.
What Counts as Postmenopausal Bleeding?

Clinically, postmenopausal bleeding (PMB) refers to any vaginal bleeding that occurs after a woman has gone 12 consecutive months without a menstrual period. This definition covers a wide range of bleeding patterns, from light spotting and brownish discharge to bleeding after sexual intercourse or heavier, more noticeable flow. Even a single episode qualifies as PMB and warrants attention; it’s not something to dismiss as minor or temporary.
“Any unusual bleeding or postmenopausal bleeding should always be investigated,” says Dr. Ross Berkowitz, William H. Baker Professor of Gynecology at Harvard Medical School. “Although most postmenopausal bleeding is not caused by cancer, investigating it gives doctors a way to catch endometrial cancer early when it is most treatable.”
Some women on hormone replacement therapy (HRT) may experience occasional light spotting or breakthrough bleeding, which can be considered normal within the context of treatment. Outside of HRT, however, any postmenopausal bleeding is abnormal and should be evaluated promptly.
The amount or frequency of bleeding doesn’t determine its significance; even minimal spotting can indicate an underlying condition. Early recognition and assessment are key to identifying the cause and ensuring timely treatment if needed.
Common causes of bleeding after menopause that are not cancer

While any postmenopausal bleeding should be taken seriously, it’s reassuring to know that most causes are benign. Understanding these non-cancerous reasons can help reduce unnecessary anxiety while still emphasizing the importance of timely evaluation. Recognizing the difference between normal changes, medication effects, or minor growths versus warning signs of more serious conditions allows women and clinicians to respond appropriately without delay.
A. Vaginal atrophy/Genitourinary syndrome of menopause (GSM)
When estrogen falls after menopause, the vaginal walls and vulvar tissues thin and dry; medical teams call this genitourinary syndrome of menopause. Thin, fragile tissue bleeds easily, especially after intercourse or minor friction; patients commonly complain of dryness, pain with sex, and spotting. Local (vaginal) estrogen or lubricants often resolve the problem.
“Vaginal tissues become less elastic and more fragile without estrogen, so light bleeding after sex is common in untreated atrophy,” notes experts at the Cleveland Clinic.
B. Polyps
Endometrial (uterine) or cervical polyps are small, usually benign growths that commonly cause irregular spotting or bleeding. They’re often easy to remove in an outpatient procedure and are not cancerous in the majority of cases, though pathology after removal confirms the diagnosis.
C. Hormone therapy (HRT)
Women starting or changing systemic HRT frequently experience breakthrough bleeding during the first several months. New or persistent bleeding beyond the initial 6 months of HRT, however, should prompt evaluation to exclude structural causes or hyperplasia.
D. Other noncancer causes
Infections (cervicitis, vaginitis), fragile vessels related to trauma or prior surgery, anticoagulant medications, and, less commonly, fibroids or endometrial hyperplasia can all cause PMB. A careful history and basic exam often suggest the next tests the clinician should prescribe.
When bleeding signals something more serious

The most worrisome cause is endometrial (uterine) cancer, but the relationship between PMB and cancer is nuanced.
- Large systematic reviews show that about 90% of women diagnosed with endometrial cancer reported vaginal bleeding beforehand, which makes bleeding an important early signal.
- At the same time, among women who present with PMB, the pooled risk of actually having endometrial cancer is approximately 9% (varies by region and HRT use). That means most women with PMB do not have cancer, but the symptom reliably flags cases that need testing.
Risk factors that raise the chance PMB is due to endometrial cancer include obesity, diabetes, late menopause, never having given birth, a history of unopposed estrogen (estrogen without a progestin), and a family history of hereditary cancer syndromes (for example, Lynch syndrome). All these factors influence how aggressively a clinician evaluates bleeding.
Other gynecologic cancers (cervical, vaginal, rarely ovarian) can also present with bleeding, so the evaluation usually includes tests that screen for those possibilities as well.
Read More: Perimenopause vs. PCOS: Overlapping Symptoms You Shouldn’t Ignore
When to see a doctor, and how urgently

Any vaginal bleeding after 12 months without a period warrants medical attention. In many health systems, PMB is treated as a priority referral: for example, the NHS recommends referral to a specialist quickly and states you should not wait more than two weeks to be seen in hospital or a dedicated clinic. If bleeding is heavy, accompanied by large clots, severe pain, fever, or fainting, seek urgent care.
At your appointment, expect a focused history and pelvic exam; the clinician will ask about HRT, medications (like anticoagulants), prior gynecologic problems, weight changes, and family cancer history, details that guide which diagnostic path to follow.
How doctors diagnose the cause
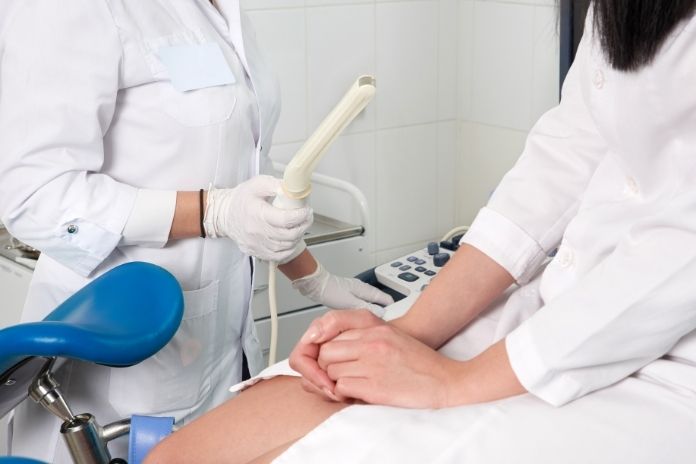
There are three core tests commonly used:
- Transvaginal ultrasound (TVUS) to measure the endometrial thickness and look for polyps or fluid. A thin lining (≤4 mm) in a woman with a single episode of bleeding has a very high negative predictive value for endometrial cancer and may reduce the need for immediate biopsy in low-risk patients.
- Endometrial biopsy (office sampling) is a quick, often in-office procedure that collects tissue for pathology. Many guidelines recommend a biopsy whenever suspicion is higher or if the ultrasound is indeterminate.
- Hysteroscopy (direct view of the uterine cavity) and removal of polyps or targeted sampling when imaging or blind biopsy is non-diagnostic. Additional blood tests or cultures may be used if infection or bleeding disorders are suspected.
Treatment depends on the cause

- Vaginal atrophy (GSM): first-line therapy is local vaginal estrogen (creams, rings, or tablets) or nonhormonal moisturizers and lubricants; symptoms and bleeding usually improve. Energy-based devices are being studied, but are not first-line.
- Polyps: typically removed hysteroscopically; pathology confirms benign versus malignant tissue.
- HRT-related or structural bleeding: dose adjustment, switching formulations, or temporary pauses in HRT are common management steps, always under clinician supervision.
- Endometrial cancer: treatment most often starts with surgery (hysterectomy with removal of fallopian tubes and ovaries), sometimes followed by radiation, chemotherapy, or hormone/targeted therapy depending on stage and tumor type. Early detection yields very high cure rates.
The good news: many causes of PMB are treatable, and cancers detected because of bleeding are often found early, when outcomes are best.
Read More: Perimenopause: Symptoms to Watch and Lifestyle Strategies to Ease the Transition
Frequently Asked Questions (FAQs)
Is light spotting after menopause “normal”?
No, any bleeding after 12 months without a period is abnormal and should be evaluated, even if it’s a single, light episode. HRT can cause early spotting, but persistent bleeding still needs assessment.
Can stress cause bleeding after menopause?
Stress alone is an unlikely explanation for postmenopausal bleeding. Always check with your clinician; stress may affect other body systems, but PMB needs diagnostic evaluation.
How common is cancer in postmenopausal bleeding cases?
Meta-analyses show roughly 9% of women who present with PMB are diagnosed with endometrial cancer, though this varies by region and hormone use. Remember: a very high proportion (~90%) of endometrial cancers present with bleeding, so the symptom is valuable for early detection.
Does one episode mean cancer?
No, most single episodes are benign causes. But one episode should prompt evaluation; it’s the only realistic way to rule cancer in or out early.
Conclusion
Bleeding after menopause is always considered abnormal and should never be ignored, but it’s important to remember that it is not always a sign of cancer. Most episodes arise from treatable conditions such as vaginal atrophy, benign polyps, or temporary hormonal effects, which can often be managed effectively with simple interventions. At the same time, postmenopausal bleeding is the most common early symptom of endometrial cancer, making it a critical warning sign that demands timely attention.
Prompt evaluation, typically including a pelvic exam, transvaginal ultrasound, and, if necessary, an endometrial biopsy, offers the best chance for early detection and successful treatment. Early diagnosis not only improves outcomes but can also mean the difference between simple, minimally invasive treatments and more complex interventions later on.
The key message is clear: never dismiss postmenopausal bleeding as “minor” or “normal.” Even a single episode warrants a call to your gynecologist. Being proactive, informed, and attentive to your body can save lives, give peace of mind, and ensure that any underlying issue, whether benign or serious, is addressed promptly. Early action is your strongest tool for safeguarding health after menopause.
References
- https://my.clevelandclinic.org/health/diseases/21549-postmenopausal-bleeding
- https://www.ncbi.nlm.nih.gov/books/NBK562188/
- https://www.yalemedicine.org/conditions/postmenopausal-bleeding
- https://kangaroocareindia.com/blogs/postmenopausal-bleeding-causes-symptoms-and-when-to-worry/203
- https://www.healthdirect.gov.au/bleeding-after-menopause
- https://ajbm.net/wp-content/uploads/2019/09/Assessment-of-postmenopausal-bleeding-a-cohort-case-study.pdf
- https://www.thewomens.org.au/health-information/periods/periods-overview/bleeding-after-menopause
- https://www.webmd.com/menopause/postmenopausal-bleeding
- https://www.acog.org/womens-health/experts-and-stories/the-latest/bleeding-after-menopause-could-be-a-problem-heres-what-to-know
- https://www.mayoclinichealthsystem.org/hometown-health/speaking-of-health/postmenopausal-bleeding-should-you-be-concerned
- https://www.mayoclinic.org/diseases-conditions/menopause/expert-answers/bleeding-after-menopause/faq-20058396
- https://www.mayoclinichealthsystem.org/hometown-health/speaking-of-health/postmenopausal-bleeding-should-you-be-concerned
- https://www.nhs.uk/symptoms/post-menopausal-bleeding/
- https://www.foxchase.org/blog/5-things-know-about-postmenopausal-bleeding
- https://drroomasinha.in/solution/postmenopausal-bleeding/
- https://continentalhospitals.com/diseases/postmenopausal-bleeding/
- https://www.medicalnewstoday.com/articles/317624
- https://utswmed.org/medblog/postmenopausal-bleeding/
- https://www.cancer.gov/news-events/cancer-currents-blog/2018/endometrial-cancer-bleeding-common-symptom
- https://www2.hse.ie/conditions/postmenopausal-bleeding/
In this Article





















