Cervical cancer is one of the most preventable cancers in women today, and that’s largely because we have powerful tools to catch it early or stop it before it even develops. The two most common tools you’ll hear about are the Pap smear and the HPV test. At first glance, they may sound interchangeable, but they serve different purposes and give doctors different information about your cervical health.
Knowing how these tests work, when each is recommended, and what the results actually mean can take a lot of the fear and confusion out of screening. Instead of just showing up for whatever test is ordered, you’ll understand why it’s being done, what your options are, and how it fits into long-term prevention.
In this guide, we’ll break down Pap smears versus HPV tests, how often you need them, what happens if results are abnormal, and how vaccination plays into the bigger picture of protecting yourself against cervical cancer.
What Is a Pap Smear?
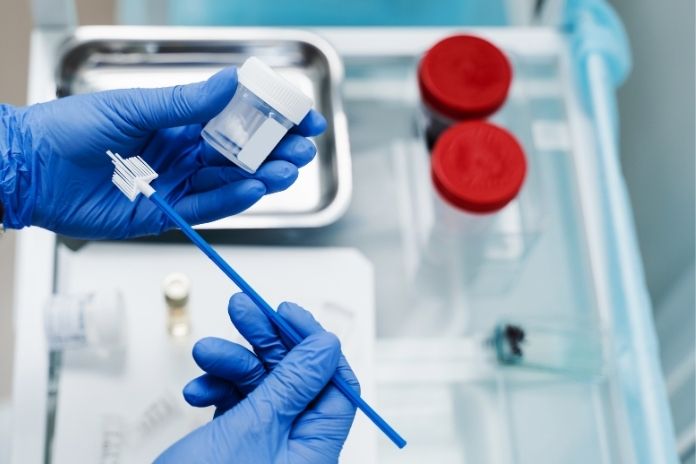
A Pap smear, also known as a Pap test, is one of the most important tools in women’s health. It is a screening procedure designed to detect abnormal or precancerous cells on the cervix, the lower, narrow end of the uterus that opens into the vagina. The goal is not only to find cancer early but also to identify cell changes long before they become dangerous. This makes the Pap smear a powerful method of prevention, not just detection.
How it’s performed
The test is typically done during a routine pelvic exam at your doctor’s office. Your provider will insert a speculum into the vagina to gently separate the vaginal walls and provide a clear view of the cervix. A small brush or spatula is then used to collect a sample of cells from the surface of the cervix.
These cells are preserved and sent to a laboratory, where specialists examine them under a microscope for any signs of abnormal changes. The entire procedure takes just a few minutes. For most women, it may feel slightly uncomfortable or cause mild pressure, but it is generally not painful.
What the results mean
Pap smear results fall into different categories:
- Normal (negative): No abnormal cells were found, and no further testing is needed until your next scheduled screening.
- ASC-US (Atypical Squamous Cells of Undetermined Significance): Mild changes are present. These may be caused by irritation, inflammation, infection, or human papillomavirus (HPV).
- LSIL (Low-Grade Squamous Intraepithelial Lesion): Early changes in cervical cells, often linked to HPV infection. These are usually mild but may need follow-up.
- HSIL (High-Grade Squamous Intraepithelial Lesion): More serious changes that have a higher risk of progressing into cancer if not treated.
- Atypical glandular cells or cancer cells: Less common findings but more concerning, requiring additional testing such as a colposcopy or biopsy.
Why it matters
The Pap smear has been one of the greatest public health achievements in women’s healthcare. According to the National Cancer Institute (NCI), widespread Pap testing has reduced cervical cancer rates in the United States by more than 50% since the 1950s.
In fact, most cervical cancers can be prevented or detected at a very early stage with regular screening. For women, staying up-to-date with Pap smears is one of the simplest and most effective ways to protect long-term reproductive health.
Read More: How Regular Screenings Can Save Your Life: The Importance of Pap Smears
What Is an HPV Test?
The HPV test is another important screening tool, but instead of looking at cervical cells under a microscope, it detects the presence of the human papillomavirus (HPV) itself. HPV is the most common sexually transmitted infection worldwide, and while most infections clear naturally within one to two years, some strains can linger.
Persistent infection with high-risk HPV types, especially HPV 16 and HPV 18, is the primary cause of cervical cancer. Because of this, HPV testing has become a crucial part of cervical cancer prevention strategies.
How it’s performed
The HPV test is usually performed alongside a Pap smear during a routine pelvic exam, though it can also be done separately. Often, the same cervical cell sample collected for a Pap test is used for HPV testing, which means no additional procedure is needed.
In the laboratory, specialists run molecular tests to detect the DNA of high-risk HPV strains. Some clinics may even offer primary HPV testing, where only the HPV test is done without a Pap smear, particularly for women over 30, since HPV results are highly predictive of future cervical risk.
Why HPV matters
Almost all cervical cancers are caused by persistent HPV infections. According to the World Health Organization (WHO) and the Centers for Disease Control and Prevention (CDC), identifying high-risk HPV types allows healthcare providers to detect women at risk long before cell changes occur.
This makes the HPV test an early warning system that complements, and in some cases may replace, the Pap smear. By catching infections that don’t go away, doctors can monitor, intervene, and prevent progression to precancer or cancer. In short, HPV testing adds another layer of protection, making cervical cancer one of the most preventable cancers today.
Key Differences Between Pap Smear and HPV Test
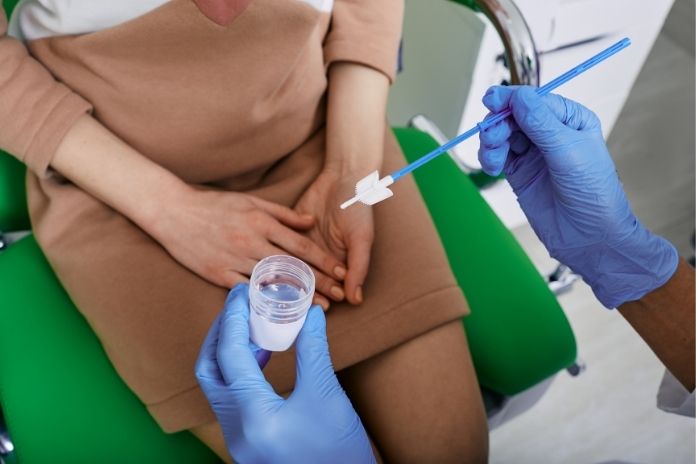
Although the Pap smear and HPV test are often performed together, they serve different purposes. Both involve collecting a sample of cells from the cervix, but what happens in the lab, and what the results mean, is not the same.
 When Should You Get a Pap Smear or HPV Test?
When Should You Get a Pap Smear or HPV Test?

Cervical cancer screening isn’t one-size-fits-all. The right schedule depends on your age, medical history, and risk factors. Here’s how leading organizations like the USPSTF, ACOG, and the American Cancer Society outline it:
Ages 21–29
- Pap smear every 3 years.
- HPV testing is not recommended as a routine test in this age group, since HPV infections are extremely common and most clear up without causing problems.
- The focus is on detecting early cell changes rather than the virus itself.
“Women age 21 to 29 should get a Pap test every three years OR get an HPV test every 5 years starting at age 25.” – Kathleen Schmeler, M.D., MD Anderson Cancer Center.
Ages 30–65
At this stage, you have three options:
- Pap smear alone every 3 years.
- HPV test alone every 5 years.
- Co-testing (Pap + HPV) every 5 years (often considered the most thorough approach).
Your provider may recommend one over the other depending on your personal health history and what’s available.
After 65
- Screening may stop if:
- You’ve had consistent, adequate prior screening, and
- You have no history of serious abnormal results.
- If you’ve had precancerous changes or cervical cancer in the past, your doctor may recommend continued screening beyond 65.
Exceptions to the General Guidelines
Certain situations call for earlier, more frequent, or prolonged screening:
- History of abnormal results.
- If you’ve ever had a Pap smear or HPV test that showed abnormalities, your provider may shorten the interval between tests.
- Weakened immune system
- Conditions such as HIV, organ transplant, or long-term steroid use can increase risk. These women typically need more frequent screening.
- Post-hysterectomy
- If your hysterectomy removed the cervix for non-cancer reasons, you may not need further screening.
- If the surgery was done because of cancer or precancer, regular screening is usually still required.
The key takeaway: don’t assume your schedule is identical to your friend’s. Age, medical history, and risk factors all shape the right plan for you.
What Happens If Results Are Abnormal?
Getting an abnormal Pap smear or a positive HPV test result can feel alarming, but it doesn’t mean you have cancer. These tests are designed to catch early changes long before they turn into something serious. Here’s what different results usually mean and what happens next.
Abnormal Pap Smear Results
- ASC-US (Atypical Squamous Cells of Undetermined Significance): Mild, often temporary changes. Your doctor may recommend repeating the Pap test in a year or doing a reflex HPV test to check if a high-risk HPV infection is present.
- LSIL (Low-Grade Squamous Intraepithelial Lesion): Early, mild changes often linked to HPV. These are usually monitored closely and may resolve on their own, but follow-up testing or colposcopy could be suggested.
- HSIL (High-Grade Squamous Intraepithelial Lesion): More concerning changes with a higher risk of progressing to cancer if untreated. Colposcopy and biopsy are typically recommended.
- Atypical glandular cells or more severe findings: These results are less common but more significant. They usually require immediate colposcopy and further diagnostic testing.
Jenell Coleman, M.D., M.P.H., Medical Director of the Women’s Health Center at Johns Hopkins and Co-Director of the Colposcopy Clinic, says: “The good news is that we can actually prevent people from getting cancer because these cellular changes happen over several years. With a Pap test, we can treat abnormal cells before they progress to cancer.”
Positive HPV Test
- High-risk HPV detected (other than 16 or 18): Often managed with repeat testing in 12 months, since many infections clear naturally.
- Persistent HPV infection: If the virus doesn’t clear or if cell changes are seen, your provider may recommend Pap + HPV co-testing or colposcopy.
- HPV types 16 or 18 detected: These are the highest-risk strains. Your provider will likely recommend immediate colposcopy for closer examination.
Emotional Reassurance
- The CDC emphasizes that most HPV infections clear naturally within 1–2 years, especially in younger women.
- Abnormal results are signals for closer monitoring, not a cancer diagnosis.
- Early detection is the reason cervical cancer rates have dropped so significantly over the past decades. Treatment is most effective when changes are caught early.
The bottom line: abnormal results mean it’s time for closer follow-up, not panic. With proper care and timely monitoring, most issues are treatable long before they become dangerous.
Preventive Care Beyond Screening
Cervical cancer prevention doesn’t stop at Pap smears and HPV tests. A comprehensive approach includes vaccination, regular checkups, and lifestyle choices that lower risk and support long-term health.
HPV Vaccination
The HPV vaccine (Gardasil 9 in the U.S.) is one of the strongest tools we have against cervical cancer. It protects against the high-risk HPV strains responsible for about 90% of cases, as well as other cancers linked to HPV.
- Routine vaccination: Recommended for all children from ages 11–12, though it can start as early as age 9.
- Catch-up vaccination: Available up to age 26 for those who missed earlier doses.
- Adults 27–45: May also benefit depending on risk factors and should discuss options with their provider.
Even if you’re already sexually active, the vaccine can still protect against strains you haven’t encountered.
Regular Gynecological Checkups
Screening is one piece of the puzzle. Routine gynecological visits help keep the bigger picture of women’s health in focus. These appointments are a chance to:
- Review reproductive health and contraception options.
- Discuss menstrual or menopause concerns.
- Address symptoms like pelvic pain or abnormal bleeding early.
- Stay updated on broader preventive care.
Consistent checkups create opportunities to catch issues before they escalate.
Lifestyle Support
Your daily habits also play a powerful role in lowering cervical cancer risk and supporting your body’s ability to clear HPV naturally.
- Quit smoking: Tobacco weakens the immune system and doubles the risk of cervical cancer in women with HPV.
- Practice safer sex: Condoms and limiting sexual partners reduce HPV transmission, though not completely.
- Support your immune system: A balanced diet, regular physical activity, stress management, and good sleep all help the body fight off infections more effectively.
Put together, these steps, vaccination, screening, checkups, and healthy habits, form a strong defense against cervical cancer and support overall reproductive health.
Read More: Post-Treatment Care for Cervical Cancer Survivors: Tips for a Healthy Life
When to Talk to Your Doctor
See your provider if:
- You’re unsure which test is recommended for your age group.
- You have symptoms such as unusual vaginal bleeding, foul-smelling discharge, or persistent pelvic pain.
- You’ve had abnormal results in the past and need clarity on follow-up timing.
- You’re due for screening and want to discuss HPV vaccination or co-testing.
Remember: cervical cancer screening is preventive, not reactive. The earlier cell changes are caught, the easier they are to treat.
Conclusion
Both the Pap smear and the HPV test are cornerstones of cervical cancer prevention, but they serve different purposes. The Pap smear looks for abnormal cell changes on the cervix, while the HPV test detects the virus responsible for nearly all cervical cancers. When combined, they create a safety net that can catch risks early, long before cancer develops.
The most important step is not choosing one test over the other, but staying consistent with your screening schedule. Pair that with HPV vaccination (if you’re eligible) and regular gynecological care, and you’re giving yourself the best possible protection.
Here’s the bottom line: cervical cancer is one of the most preventable cancers we know of. With modern tools, early detection, and healthy habits, thousands of cases are avoided every year. Prioritize your screening, talk to your provider, and remember, these simple tests have the power to save lives, including yours.
References
- https://www.mayoclinic.org/tests-procedures/pap-smear/about/pac-20394841
- https://my.clevelandclinic.org/health/diagnostics/4267-pap-smear
- https://www.cancer.gov/publications/dictionaries/cancer-terms/def/pap-smear
- https://en.wikipedia.org/wiki/Pap_test
- https://medlineplus.gov/lab-tests/pap-smear/
- https://emedicine.medscape.com/article/1947979-overview
- https://www.cancer.org/cancer/types/cervical-cancer/detection-diagnosis-staging/screening-tests/pap-test.html
- https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/pap-test
- https://www.scripps.org/news_items/7193-pap-test-vs-hpv-test-what-s-the-difference
- https://www.cloudninecare.com/blog/pap-smear-vs-hpv-test-whats-the-difference
- https://www.cdc.gov/cervical-cancer/screening/index.html
- https://careerhospital.in/difference-between-hpv-and-pap-smear-test
- https://womenshealth.gov/a-z-topics/pap-hpv-tests
In this Article