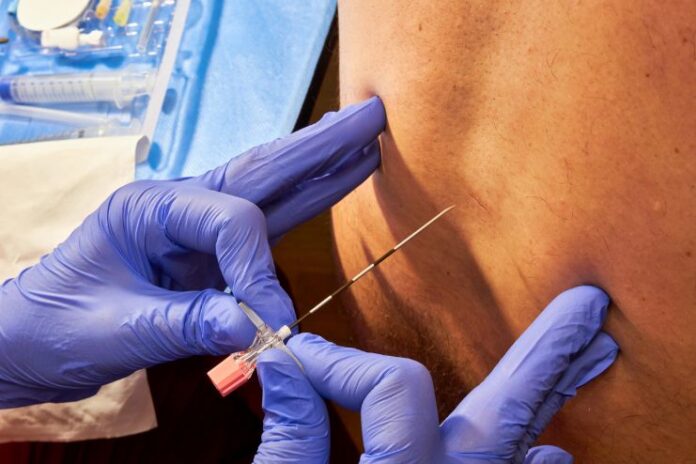
If you’re expecting a baby and weighing your pain relief options, you’ve probably found yourself circling one key question: When should I ask for the epidural?
You’re not alone. This is one of the most common, and sometimes most emotionally loaded, questions pregnant women and birthing people face as they prepare for labor. And it’s no wonder. The decision to get an epidural isn’t just about pain; it’s about control, comfort, timing, and feeling empowered in one of life’s most intense moments.
For some, the idea of an epidural offers immense relief, a beacon of reassurance that pain doesn’t have to define their birth experience. For others, it brings hesitation, fueled by worries about side effects, timing, or whether it might slow labor down.
But here’s the truth: What’s “right” depends on your body, your birth plan, your medical situation, and how labor unfolds in real time.
That said, understanding the science, the guidelines, and the real-world scenarios can help you feel more confident in making the choice when the time comes.
In this guide, we’ll cover:
- What is an epidural, and how does it work?
- When do most experts recommend getting it?
- How early is too early, and how late is too late?
- What factors should be considered based on labor progression?
- Tips for communicating clearly with your provider.
Whether you’re leaning toward an unmedicated birth or planning to request an epidural as soon as contractions begin, this article will give you the clarity and confidence to make an informed, empowered choice.
Because in the end, it’s not just about managing pain, it’s about feeling supported and respected throughout your labor, on your terms.
What is an Epidural and How Does It Work?

An epidural is one of the most widely used and effective forms of regional anesthesia during labor. It works by numbing the lower half of your body, significantly reducing or eliminating pain from contractions and the birthing process, without putting you to sleep or affecting your awareness.
Unlike general anesthesia, which affects your entire body, an epidural targets the nerve pathways in the lower spine, blocking pain signals from traveling to your brain. This allows you to stay awake, alert, and engaged in your labor experience while managing discomfort in a controlled way.
Step-by-Step: What to Expect During the Procedure
- Positioning for Placement: You’ll either sit up and lean forward or lie on your side in a curled position. This helps widen the space between the bones in your lower back, making it easier for the anesthesiologist to access the right spot.
- Cleaning and Numbing: The skin on your lower back will be thoroughly cleaned with an antiseptic solution to reduce the risk of infection. A small injection of local anesthetic is then given to numb the area; this may sting briefly, but it helps ensure you don’t feel pain when the larger needle is inserted.
- Accessing the Epidural Space: A hollow needle is carefully inserted into the epidural space, the area surrounding the dura mater, which is the protective covering of the spinal cord. You may feel pressure, but not sharp pain.
- Threading the Catheter: Once the needle is in the correct position, a thin, flexible catheter (like a tiny straw) is threaded through it. The needle is then removed, leaving just the catheter in place. This catheter allows for continuous or intermittent delivery of pain medication throughout labor.
- Administering Medication: The medication typically includes a combination of a local anesthetic (such as bupivacaine, lidocaine, or ropivacaine) to numb the nerves and a small dose of an opioid (like fentanyl or sufentanil) to enhance the pain relief. These medications don’t take away all sensation; you’ll likely still feel pressure or movement, but they significantly dull or eliminate pain.
- Onset of Relief: Pain relief usually begins within 10 to 20 minutes after the initial dose. Your care team will monitor you and your baby closely to ensure both safety and effectiveness. Additional doses, or “top-ups,” can be given through the catheter to maintain comfort as labor progresses.
What You’ll Feel After the Epidural
- A warming or tingling sensation in your lower body.
- Gradual numbness from the waist down (though you may still feel pressure).
- A possible loss of full mobility, especially in your legs, though modern low-dose or “walking” epidurals preserve some movement.
- Noticeable relief from contraction pain, allowing you to rest, regain energy, or focus on other parts of your labor experience.
Epidurals do not affect your mental alertness or your ability to bond with your baby after birth. Most people describe the transition as a wave of relief, especially after hours of intense contractions.
Typical Stages of Labor: When Is an Epidural Commonly Given?
To understand the best time for an epidural, you need to know the three main stages of labor:
1. Latent Phase (0–3 cm dilation)
- Early labor is characterized by irregular, mild contractions.
- You may still feel comfortable enough to move around, rest, or even sleep between contractions.
- Experts usually discourage epidurals at this stage because:
- Labor may not yet be firmly established.
- Early epidurals can increase the risk of labor stalling or needing further interventions.
2. Active Phase (4–7 cm dilation)
- Contractions become longer, stronger, and closer together.
- You’re entering the part of labor where discomfort intensifies.
- This is the most common window for epidural placement, as labor is well underway, and pain relief can help you conserve energy for pushing.
3. Transition Phase (8–10 cm dilation)
- The most intense part of labor, with strong, frequent contractions.
- Some women reach this phase quickly, while others labor longer.
- By this point, it can be too late for an epidural, depending on hospital policy and how close you are to delivery.
Even if an epidural is technically possible, the time it takes to administer and take effect might mean you deliver before it starts working.
Bottom line: The active phase is generally considered the ideal time to get an epidural.
How Dilated Should You Be Before Getting an Epidural?
Most experts recommend waiting until you’re around 4–5 cm dilated, early active labor, before requesting an epidural. This timing strikes a balance between:
- Providing effective pain relief.
- Allowing labor to progress naturally before introducing anesthesia.
Why cervical dilation matters:
- If the epidural is given too early (before labor is active), it can slow cervical dilation and lead to a longer labor.
- If given at or after 4 cm, research shows it does not significantly increase the risk of cesarean delivery or prolonged labor compared to avoiding pain relief altogether.
This is why many hospitals follow protocols encouraging women to wait until labor has established a regular contraction pattern and the cervix has dilated to 4–5 cm.
Early vs. Late Epidural: Pros and Cons
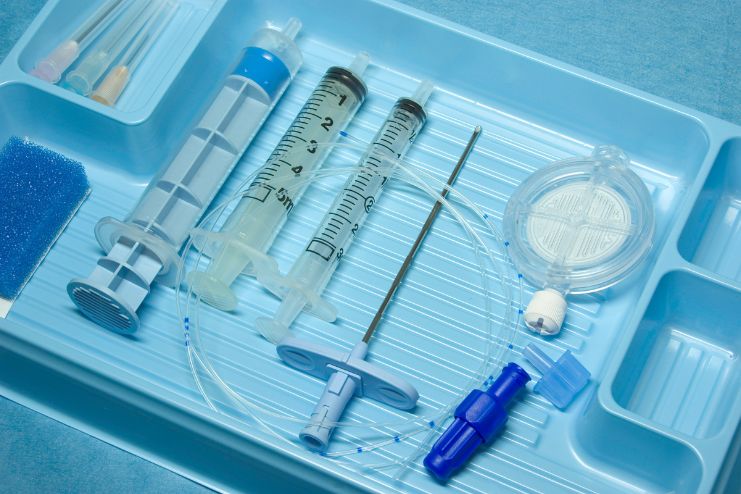
When it comes to epidural timing, it differs from person to person. Both early and late epidurals have their advantages and drawbacks.
Early Epidural (before 4 cm dilation)
Pros:
- Early pain relief can help you rest, reduce stress hormones, and relax your pelvic floor.
- Particularly beneficial if you have a long latent phase or strong early contractions.
Cons:
- Early epidurals can slow down labor by reducing contractions’ strength or frequency.
- Increased need for labor augmentation with medications like Pitocin.
- Possible higher risk of assisted delivery (forceps or vacuum) if labor stalls.
Late Epidural (after 7 cm dilation)
Pros:
- Labor often progresses faster because your body has had time to establish strong contractions before anesthesia.
- You may retain more mobility earlier in labor, which can help position the baby.
Cons:
- Contractions are more painful in late active labor and transition, so you may experience significant discomfort before relief starts.
- There’s a smaller window to place the epidural safely; if you progress quickly, it could be too late.
When Is It Too Late to Get an Epidural?
Hospitals typically consider an epidural too late when you’re in advanced transition, often beyond 8–9 cm dilation, or if the baby’s head is already descending rapidly.
Here’s why:
- It takes 10–20 minutes for an epidural to begin working after placement.
- If delivery seems imminent, there’s a chance you could give birth before the epidural provides relief.
- Administering an epidural very late can also cause low blood pressure, which may affect the baby’s heart rate.
Ultimately, the decision depends on your labor’s speed and your care team’s discretion. Some anesthesiologists are willing to attempt placement even in late labor if there’s enough time, but others may advise focusing on other pain relief methods, like IV pain medications or nitrous oxide, if an epidural is no longer practical.
How Long Does It Take for an Epidural to Start Working?
The typical onset time for an epidural is 10–20 minutes after the medication is administered. However, several factors can affect how quickly you feel relief:
- Placement Precision: If the catheter is well-positioned, pain relief starts faster.
- Dosage: Different concentrations or volumes of medication can change the onset time.
- Individual Response: Some people metabolize anesthesia faster or slower, affecting its effectiveness.
Top-ups during labor: Your anesthesiologist or nurse anesthetist can give additional doses through the catheter to maintain or deepen pain relief as needed. This means your epidural can provide continuous comfort throughout labor and pushing.
What Do Experts and Doctors Recommend?
Professional guidelines and experienced OBs, midwives, and anesthesiologists emphasize personalized decision-making when it comes to epidural timing.
The American College of Obstetricians and Gynecologists (ACOG) states there is no strict cervical dilation requirement before placing an epidural. The key is ensuring labor is established and progressing.
However, many hospitals still follow the 4–5 cm guideline to balance effective pain relief with minimizing labor interventions.
Here’s what experts recommend:
- Talk to your care team early: Let your OB or midwife know your preferences for pain relief when you arrive at the hospital.
- Stay flexible: Labor can be unpredictable. You might plan for a later epidural but find yourself wanting it sooner, or vice versa.
- Listen to your body: Your comfort matters. If pain becomes overwhelming and labor is active, it’s reasonable to ask for an epidural even if you initially planned a medication-free birth.
- Consider your medical history: Some health conditions or pregnancy complications may influence when or whether an epidural is recommended.
Ultimately, the best time to get an epidural is when your pain reaches a point that you feel you can’t manage comfortably, and when it’s still medically appropriate for placement.
Conclusion
Most women receive an epidural during active labor, typically between 4–6 cm dilation, when contractions are strong but labor is still progressing at a manageable pace. Getting it too early can slow labor, while waiting too long might mean missing the window for effective relief.
The most important takeaway? There’s no perfect timing for everyone. Trust your instincts, communicate openly with your OB or midwife, and remember that your comfort and well-being are essential parts of your birth experience.
Final reassurance: The best time for an epidural is when you feel you need it, and when your care team confirms it’s still safe and effective.
References
- https://americanpregnancy.org/healthy-pregnancy/labor-and-birth/what-is-an-epidural/
- https://madeforthismoment.asahq.org/pain-management/epidural/
- https://www.mayoclinic.org/healthy-lifestyle/labor-and-delivery/in-depth/stages-of-labor/art-20046545
- https://www.pregnancybirthbaby.org.au/epidural
- https://www.ncbi.nlm.nih.gov/books/NBK544290/
- https://www.webmd.com/baby/what-to-know-best-time-to-get-epidural
- https://www.newcastle-hospitals.nhs.uk/services/maternity/labour-and-birth/pain-relief/epidural/
- https://obgyn.onlinelibrary.wiley.com/doi/full/10.1002/ijgo.14175
- https://www.mayoclinic.org/healthy-lifestyle/labor-and-delivery/in-depth/stages-of-labor/art-20046545
- https://www.healthline.com/health/pregnancy/cervix-dilation-chart
- https://utswmed.org/medblog/epidurals-myths/
- https://www.fvhospital.com/learn-more/epidural-analgesia-in-labour-2/
- https://www.thebump.com/a/epidural
- https://pubmed.ncbi.nlm.nih.gov/7926239/
- https://www.nhs.uk/tests-and-treatments/epidural/
- https://www.birthinjuryhelpcenter.org/birth-injuries/help-center/epidural/
- https://www.npr.org/sections/health-shots/2018/10/09/655817377/when-giving-birth-for-the-first-time-push-away
- https://www.quora.com/How-many-centimeters-are-too-late-for-an-epidural
In this Article