When it comes to women’s reproductive health, two of the most common yet widely misunderstood conditions are endometriosis and polycystic ovary syndrome (PCOS). Though both can disrupt menstrual cycles and contribute to infertility, they are fundamentally different in origin, progression, and management. Unfortunately, because they share overlapping symptoms, like pelvic pain, hormonal imbalances, and irregular periods, many women face delayed diagnoses, misdirected treatments, and years of unnecessary suffering.
The lack of awareness around endometriosis and PCOS can leave individuals feeling isolated, dismissed, or misunderstood by both their peers and healthcare providers. Understanding the distinctions between these two conditions is crucial not only for accurate diagnosis but also for effective care that supports both physical and emotional well-being.
In this article, we break down the science behind what causes each condition, how they manifest, how they’re diagnosed, and the range of treatment options available. We also explore the rare but real possibility of both conditions coexisting, and how that can complicate the clinical picture.
Endometriosis vs. PCOS: Understanding the Core Differences

Endometriosis and polycystic ovary syndrome (PCOS) affect millions of women worldwide, often during their most active and fertile years. Although both conditions can cause menstrual irregularities, pelvic discomfort, and fertility challenges, they are entirely distinct in their root causes, biological mechanisms, and treatment approaches. Misunderstanding these differences can lead to delayed care, misdiagnosis, or even worsening symptoms.
Endometriosis: An Inflammatory Disease Driven by Misplaced Tissue
Endometriosis is a chronic, estrogen-dependent inflammatory condition. It occurs when tissue similar, but not identical, to the uterine lining (endometrium) begins to grow outside the uterus, typically on pelvic organs like the ovaries, fallopian tubes, bladder, or bowel. Unlike normal endometrial tissue, these rogue implants do not shed during menstruation. Instead, they bleed internally, causing inflammation, scar tissue (adhesions), and often severe pain, especially around the menstrual cycle.
Key characteristics include:
- Severe menstrual cramps (dysmenorrhea).
- Chronic pelvic pain is often unrelated to the period.
- Painful intercourse (dyspareunia).
- Painful bowel movements or urination during menstruation.
- Infertility due to damage or distortion of pelvic anatomy.
Despite being common, endometriosis is underdiagnosed and misunderstood, often taking years from symptom onset to confirmation, typically through laparoscopy.
PCOS: A Hormonal and Metabolic Imbalance
PCOS, by contrast, is a hormonal and metabolic disorder characterized by excess androgens (male hormones like testosterone), irregular ovulation, and often insulin resistance. It’s not a disease of tissue misplacement, but rather a complex condition affecting hormone regulation, metabolism, and ovarian function. The name comes from the appearance of multiple small cysts on the ovaries, though not all people with PCOS have visible cysts on imaging.
Common symptoms include:
- Irregular or absent periods
- Ovarian cysts or enlarged ovaries
- Excess facial or body hair (hirsutism)
- Acne and oily skin
- Weight gain or difficulty losing weight
- Thinning hair or scalp hair loss
- Difficulty getting pregnant due to anovulation
Unlike endometriosis, PCOS is often diagnosed with the help of blood tests (to check hormone levels), a review of symptoms, and ultrasound imaging.
Read More: Endometriosis-Symptoms, Causes, Prevention and Treatment
Why It’s Important to Understand the Differences
While they may appear similar on the surface, especially when fertility struggles or menstrual disruptions are involved, endometriosis and PCOS have vastly different origins, implications, and treatments. One is rooted in inflammation and misplaced tissue, the other in hormone imbalance and insulin resistance. This distinction is not academic; it’s crucial for choosing the right tests, medications, lifestyle strategies, and even surgical interventions.
Getting a correct diagnosis early on empowers women to take control of their reproductive health, reduce pain or symptoms, and protect their future fertility. In some cases, both conditions may even coexist, adding further complexity to diagnosis and care, but also reinforcing the need for informed, individualized treatment.
- Endometriosis often manifests as a crippling cyclic pelvic pain and painful intercourse (dyspareunia) or bowel and bladder pain.
- PCOS typically presents with metabolic and hormonal symptoms – weight gain, acne, hair thinning, hirsutism, and irregular periods.
- Common ground: Both can cause heavy periods and fertility challenges.
Root Causes and Risk Factors

Understanding the underlying causes of female reproductive health issues is essential for timely diagnosis and effective treatment. Two of the most prevalent conditions, Endometriosis and PCOS, share overlapping symptoms but arise from different root mechanisms. A mix of genetic, hormonal, and environmental factors influences both disorders. Identifying these triggers helps clinicians personalize treatment plans. Below is a breakdown of the causes and risk factors for each condition.
1. Endometriosis
Endometriosis occurs when tissue similar to the uterine lining grows outside the uterus. It is driven by hormonal changes and may be influenced by genetics and immune dysfunction. This condition often leads to pain, inflammation, and fertility issues.
- Retrograde Menstruation: Menstrual blood flows backward into the pelvic cavity, allowing endometrial cells to implant outside the uterus.
- Immune/Lymphatic Spread: A weak immune system or lymphatic transport may allow endometrial-like cells to grow in abnormal locations.
- Genetic Predisposition: Endometriosis often runs in families, increasing the risk if close female relatives are affected.
- Coelomic Metaplasia: Peritoneal cells may transform into endometrial-like tissue due to inflammation or hormonal influence.
- Hormonal Influence: Estrogen fuels the growth of endometrial tissue, worsening inflammation and pain.
2. Polycystic Ovary Syndrome (PCOS)
PCOS is a hormonal disorder that affects ovulation and causes multiple cysts on the ovaries. It is influenced by genetic, metabolic, and lifestyle-related factors. Women with PCOS often face fertility issues, weight gain, and insulin resistance.
- Genetic: PCOS is more common among women with a family history, indicating a hereditary link.
- Hyperandrogenism: Excess testosterone disrupts ovulation and causes symptoms like acne and facial hair.
- Insulin Resistance: Cells resist insulin, leading to high insulin levels that increase androgen production and weight gain.
- Lifestyle Factors: Obesity and poor lifestyle choices worsen hormonal imbalances and PCOS symptoms.
According to Ob/Gyn Dr. Yolanda Thigpen, “a combination of genetic predisposition and environmental factors, including diet, exercise, and lifestyle, contribute to the symptoms of PCOS.”
Diagnosis: A Side-by-Side
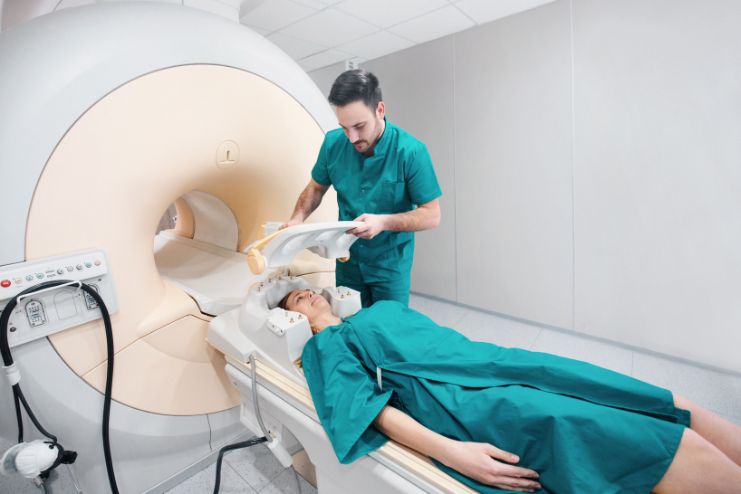
Accurate diagnosis is essential for effective treatment of Endometriosis and PCOS, both of which are often misdiagnosed or delayed. Despite overlapping symptoms like pelvic pain or irregular periods, the diagnostic process for each condition differs significantly. While Endometriosis requires surgical confirmation, PCOS is typically diagnosed through clinical signs and imaging. Knowing the gold standards and key tools helps both patients and healthcare providers act earlier.
Here’s a clear side-by-side breakdown of how each condition is identified.
1. Endometriosis
Endometriosis is notoriously difficult to diagnose due to its variable presentation and invisible lesions. Often, diagnosis is delayed for years due to symptom overlap with other conditions. A combination of surgical, imaging, and symptom-based assessments is used.
- Diagnostic Laparoscopy (Gold Standard): A minimally invasive surgery that allows visual confirmation of lesions; biopsy improves accuracy.
- Imaging (Ultrasound/MRI): Detects large cysts (endometriomas), but smaller lesions are often missed, limiting reliability.
- Symptom-Based Assessment: Chronic pelvic pain, painful periods, and painful sex are evaluated alongside physical examination findings.
2. Polycystic Ovary Syndrome (PCOS)
PCOS diagnosis is based on clinical criteria supported by imaging and hormone profiles. Unlike Endometriosis, surgery is not required for confirmation. The Rotterdam criteria are globally accepted for identifying PCOS.
- Rotterdam Criteria (Need 2 of 3): Irregular or absent ovulation, signs of hyperandrogenism, and polycystic ovaries on ultrasound.
- Ultrasound Imaging: “String of pearls” appearance from multiple small ovarian follicles is a classic finding.
- Blood Tests: Measures androgens, LH/FSH ratio, insulin, and glucose to assess hormonal and metabolic imbalances.
Impact on Fertility and Reproductive Health

Both Endometriosis and PCOS are leading contributors to female infertility worldwide. Below is a breakdown of how each condition impacts reproductive health, separately and when they co-occur.
Endometriosis
Endometriosis can significantly affect fertility, often before a woman even realizes she has the condition. Damage to reproductive organs and inflammatory changes are key culprits. Early treatment can improve the chances of conception.
- Major Cause of Infertility: Around 30–50% of women with endometriosis experience difficulty conceiving.
- Mechanisms of Impact: Inflammation disrupts egg quality, fallopian tube function, and can lead to pelvic adhesions or scarring.
Polycystic Ovary Syndrome (PCOS)
PCOS primarily affects fertility through irregular ovulation or complete lack of ovulation. Even when ovulation occurs, hormonal imbalance can interfere with implantation and early pregnancy. Management often includes lifestyle changes and medications like ovulation inducers.
- Ovulation-Related Infertility: Up to 70–80% of women with PCOS struggle with anovulation while trying to conceive.
- Other Reproductive Risks: Chronic unopposed estrogen raises the risks of miscarriage and endometrial cancer over time.
Co-occurrence: PCOS + Endometriosis
Though rare, some women have both PCOS and Endometriosis, making diagnosis and treatment more complex. This dual diagnosis often results in compounded fertility and pain-related issues. Medical management must be highly individualized in such cases.
- Prevalence: About 5% of women undergoing laparoscopy have both conditions; ~2% in the general population.
- Compounded Risks: Women with both have 10× higher odds of subfertility and 2.5× more chronic pelvic pain.
- Crossover Cases: Roughly 7% of endometriosis patients are also diagnosed with PCOS.
Treatment Options
Managing Endometriosis and PCOS requires a combination of medical, lifestyle, and sometimes surgical approaches. Because both conditions affect hormones and fertility, individualized treatment plans are essential. For Endometriosis, the focus is on pain relief and lesion removal. PCOS management targets hormone regulation, ovulation, and metabolic health. Here’s how both conditions are treated, along with expert insights on best practices.
1. Endometriosis
Treatment for Endometriosis is tailored to symptom severity and fertility goals. It ranges from medication to surgical excision, supported by lifestyle changes. Long-term management often combines multiple modalities.
- Pain Relief: NSAIDs like ibuprofen and naproxen help reduce menstrual cramps and pelvic pain.
- Hormonal Therapies: Includes birth control pills, progestins, GnRH agonists, and hormone-releasing IUDs.
- Surgical Intervention: Laparoscopic excision removes endometrial lesions and improves fertility outcomes.
- Supportive Care: Pelvic physiotherapy, anti-inflammatory diet, and mental health therapy ease chronic symptoms.
Dr. Luna, a reproductive medicine specialist at Cleveland Clinic, emphasizes: “Luckily, endometriosis treatment has come a long way in recent years, and is now tailored to individual needs and goals. We meet you where you are. Is it pain relief? Is it fertility? Is it having a baby in the next year?”
2. Polycystic Ovary Syndrome (PCOS)
PCOS treatment is multidimensional, balancing hormones, managing insulin levels, and supporting fertility. Lifestyle changes play a significant role in long-term symptom control. Management often evolves as patient needs change.
- Hormonal Regulation: Birth control pills manage irregular cycles; spironolactone reduces unwanted hair growth.
- Insulin Control: Metformin improves insulin sensitivity; diet and exercise reduce metabolic risk.
- Ovulation Induction: Letrozole or clomiphene are first-line therapies to help induce ovulation for pregnancy.
- Cosmetic and Metabolic Care: Acne medications, weight loss plans, and GLP‑1 agonists may be recommended based on symptoms.
Read More: 20 Natural Remedies For Endometriosis For Faster Relief
Can You Have Both Endometriosis AND PCOS?
Yes. While not common, a simultaneous diagnosis of Endometriosis and PCOS is possible and can present unique challenges.
A study reported approximately 7% overlap, highlighting that although both are distinct hormonal and reproductive disorders, they can co-occur in a small but significant group of patients.
What It Means Clinically
Having both conditions can complicate diagnosis, as some symptoms, like irregular periods, chronic pelvic pain, and infertility, overlap. This overlap may delay proper treatment or lead to underdiagnosis of one condition while focusing on the other.
For instance:
- Endometriosis causes tissue similar to the uterine lining to grow outside the uterus, leading to pain and inflammation.
- PCOS primarily involves hormonal imbalances and ovulatory dysfunction, often linked to insulin resistance and hyperandrogenism.
When both are present, the mechanisms behind pain and fertility disruption become more complex. A patient might have normal-appearing ovaries but still experience ovulatory issues, or severe pelvic pain without visible endometriotic lesions on ultrasound, making laparoscopy and hormonal panels crucial for accurate diagnosis.
Managing the Dual Diagnosis
Because of this complexity, treatment typically requires coordinated care involving:
- A gynecologist to manage structural and pain-related concerns, especially for Endometriosis.
- An endocrinologist or reproductive specialist to address ovulation, insulin resistance, and hormonal imbalances from PCOS.
- Fertility specialists for those planning conception, as both conditions independently impact fertility and may require assisted reproductive technologies (ART).
In cases where surgery is needed to remove endometriosis lesions, timing and hormonal preparation are especially important in patients who also have PCOS, as their ovulatory cycles are already irregular.
Studies and Research Highlights
A 2023 multi-site study (Salt Lake/SF) revealed:
- Operative cohort (473 women): 35% endometriosis only, 9% PCOS only, 5% both.
- Population cohort (127 women): 10% endometriosis only, 8% PCOS only, 2% both.
They also found that women with both had a 10‑fold increase in subfertility and 2.5‑fold more chronic pelvic pain.
Cellular-level insights
A 2025 Nature Med paper used single-cell transcriptomics to show that metformin plus lifestyle changes in PCOS patients improved endometrial health, identifying specific epithelial and stromal cell changes associated with insulin and androgen sensitivity.
Managing Life with Endometriosis vs. PCOS

Living with a chronic condition like Endometriosis or PCOS can feel overwhelming, but with the right strategies, both are manageable. While they differ in symptoms and treatment, both require a holistic approach to physical, emotional, and hormonal health.
Endometriosis
Endometriosis occurs when tissue similar to the uterine lining grows outside the uterus, causing pain, fatigue, and fertility challenges. Managing it requires a mix of symptom tracking, diet, therapies, and emotional support.
- Pain Log: Track symptoms daily to identify triggers and discuss with your doctor.
- Diet: Eat anti-inflammatory foods; limit red meat, dairy, and processed snacks.
- Therapies: Pelvic physio or TENS can ease chronic pelvic pain naturally.
- Support Groups: Connect with others to share experiences and reduce emotional stress.
PCOS (Polycystic Ovary Syndrome)
PCOS is a hormonal disorder affecting metabolism, skin, and fertility. Lifestyle adjustments, medical guidance, and emotional care play key roles in long-term management.
- Lifestyle: Follow a low-GI diet and stay active to manage weight and insulin.
- Medical Management: Treat with metformin, birth control, or anti-androgens as needed.
- Skin Care: See a dermatologist for acne, hair issues, and effective routines.
- Mental Health: Therapy helps with mood swings, anxiety, and body image concerns.
Final Thoughts
Living with Endometriosis or PCOS isn’t easy; it often means navigating a maze of pain, hormonal chaos, emotional strain, and invisible battles. These are not just medical conditions; they affect your identity, energy, appearance, and relationships. But here’s the truth: with awareness, support, and consistent self-care, they can be managed, and you can still live a vibrant, fulfilling life.
Build a routine that works for you: a nourishing diet, movement you enjoy, mental health check-ins, expert guidance, and a support system that gets it. Keep going, one day at a time, one choice at a time. Whether you’re in the middle of a flare-up or finding your rhythm, know that healing isn’t linear, but it is always possible.
You are more than your diagnosis. You are worthy of care, balance, and peace.
References
- https://www.healthline.com/health/womens-health/endometriosis-vs-pcos
- https://www.medicalnewstoday.com/articles/endometriosis-vs-pcos
- https://www.aucmed.edu/about/blog/endometriosis-vs-pcos-explained
- https://www.kofinasfertility.com/patient-info/pcos-and-endometriosis
- https://health.clevelandclinic.org/signs-symptoms
- https://www.medicalnewstoday.com/articles/161858
- https://www.goodrx.com/health-topic/diagnostics/signs-vs-symptoms
- https://firstaidtrainingcooperative.co.uk/difference-between-signs-symptoms/
- https://openworks.mdanderson.org/cgi/viewcontent.cgi?article=1005&context=word2023
- https://learning.eupati.eu/mod/book/view.php?id=215
- https://www.hopkinsmedicine.org/health/conditions-and-diseases/fertility-and-reproductive-health
- https://www.who.int/news-room/fact-sheets/detail/infertility
- https://www.cdc.gov/reproductive-health/infertility-faq/index.html
In this Article






















