Imagine dealing with urgent bathroom trips, abdominal pain, and rectal bleeding on a daily basis—this is the reality for over 900,000 Americans living with ulcerative colitis.
Ulcerative colitis is a chronic inflammatory condition affecting the large intestine (colon), where water is absorbed from waste material before it’s stored and eliminated. In ulcerative colitis, inflammation occurs in the inner lining of the colon, causing symptoms such as abdominal pain, rectal bleeding, and diarrhea.
This condition is often grouped with other inflammatory bowel diseases (IBD), including Crohn’s disease, though ulcerative colitis specifically affects only the colon’s inner lining. The disease can affect both men and women at any age, from childhood through adulthood.
This comprehensive guide covers everything you need to know about ulcerative colitis, including its symptoms, causes, treatment options, and prevention strategies.
Causes of Ulcerative Colitis
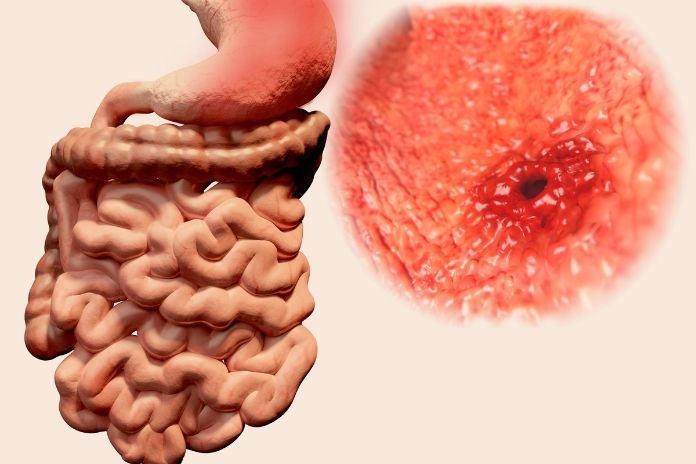
The primary cause of ulcerative colitis involves a malfunction in the immune system, which normally protects the body from infections caused by bacteria, viruses, and fungi. In ulcerative colitis, the immune system behaves abnormally and attacks the body’s own tissue, resulting in chronic inflammation of the large intestine.
“We think that the development of ulcerative colitis, which is a chronic inflammation of the colon, is multifactorial,” she said. “So it’s likely related to genetics, diet, and environment. And so what I mean by ‘environment’ is exposure to certain bacteria and certain infections that can sometimes trigger an autoimmune inflammatory condition in the colon.”
Genetic Factors: Ulcerative colitis can run in families, making it more common among people with a family history of inflammatory bowel disease. Researchers have identified more than 30 genes that may influence the development of ulcerative colitis. However, the exact genetic mechanisms and their relationship to treatment outcomes are still being studied.
Symptoms of Ulcerative Colitis
The most common symptoms of ulcerative colitis include rectal bleeding, abdominal pain, and diarrhea. The severity of symptoms depends on the extent and intensity of inflammation. Generally, inflammation limited to the rectum produces milder symptoms than more widespread disease.
Symptoms vary based on the type and location of ulcerative colitis:
Ulcerative Proctitis
In this form, inflammation is limited to the rectum. The primary symptom is rectal bleeding, often accompanied by tenesmus (feeling of incomplete bowel evacuation) and urgency.
Proctosigmoiditis
This type involves inflammation of both the rectum and sigmoid colon. Symptoms include rectal bleeding, tenesmus, urgency, cramping, and bloody diarrhea.
Left-sided Colitis
Inflammation begins at the rectum and extends to the left (sigmoid and descending) colon. Common symptoms include left-sided abdominal pain, bloody diarrhea, weight loss, and cramping.
Pancolitis
This severe form involves inflammation of the entire colon. Symptoms include rectal bleeding, fatigue, significant weight loss, fever, night sweats, abdominal pain, and cramping. This type is considered more serious and challenging to treat.
Fulminant Colitis
Although rare, this is the most severe form of ulcerative colitis. Patients experience severe dehydration, excessive bleeding, and persistent diarrhea. This life-threatening condition requires immediate hospitalization with intravenous medications and monitoring. In some cases, surgical removal of the colon may be necessary.
Complications of Ulcerative Colitis
Ulcerative colitis can lead to several serious complications, some of which can be life-threatening.
Cancer Risk The most significant long-term complication is an increased risk of colon cancer. Patients with ulcerative colitis have a two- to three-fold increased risk of developing colorectal cancer compared to the general population, with risk estimates of approximately 2% after 10 years, 8% after 20 years, and 18% after 30 years of disease. Regular screening is essential for early detection.
Other Complications Include:
- Arthritis and joint problems: Low back pain due to inflammation of the sacroiliac joints and other joint complications
- Eye and skin problems: Development of red, painful skin nodules and eye inflammation that can affect vision and require immediate medical attention
- Liver and bile duct diseases: Inflammation of bile ducts and other liver complications that may, in severe cases, require liver transplantation
- Blood clots:Increased risk of developing blood clots throughout the body
- Ankylosing spondylitis: A condition affecting the vertebral joints, more commonly seen in people with inflammatory bowel disease
Diagnosis of Ulcerative Colitis

Diagnosing ulcerative colitis typically begins with evaluating common symptoms such as diarrhea, rectal bleeding, and abdominal pain. Your healthcare provider may recommend several diagnostic tests:
- Endoscopy: To visually examine the colon lining and assess the extent of inflammation
- Tissue biopsy: Small tissue samples taken during endoscopy to confirm the diagnosis
- Stool tests: To check for infectious agents that might be causing inflammation
- Blood tests: To look for signs of inflammation and rule out other conditions
- Imaging studies: Such as CT scans or barium enemas to evaluate the extent of disease
Treatment of Ulcerative Colitis

Treatment for ulcerative colitis typically involves both medications and, in severe cases, surgery. Currently, there is no cure for ulcerative colitis, but various treatments can help manage symptoms and maintain remission.
Medication Options:
- Anti-inflammatory drugs to reduce inflammation
- Immune system suppressors to prevent the immune system from attacking the colon
- Biologics for moderate to severe cases
- Symptom-specific medications for diarrhea, pain, and other symptoms
Surgical Treatment: Surgery may be recommended for severe cases that don’t respond to medication. The most common procedure involves removing the entire colon and rectum. While this is a major decision, it can be curative and significantly improve the quality of life for patients with severe, treatment-resistant disease.
Managing Flare-ups and Remission: Ulcerative colitis follows a pattern of flare-ups (active symptoms) and remission (symptom-free periods). During flare-ups, patients may experience increased diarrhea, abdominal pain, and rectal bleeding. The goal of treatment is to achieve and maintain remission for as long as possible.
Living with Ulcerative Colitis

While ulcerative colitis is a chronic condition requiring ongoing medical care, many people with the disease lead full, active lives. Working closely with your healthcare team, following prescribed treatments, and making appropriate lifestyle modifications can help manage symptoms and prevent complications.
Regular monitoring and preventive care, including colon cancer screening, are essential components of long-term management for people with ulcerative colitis.
Ready to Take Control of Your Digestive Health?
If you’re experiencing symptoms of ulcerative colitis or have been recently diagnosed, don’t wait to seek proper medical care. Early diagnosis and treatment can significantly improve your quality of life and prevent serious complications. Schedule an appointment with a gastroenterologist today to discuss your symptoms and develop a personalized treatment plan.
Frequently Asked Questions (FAQ)
Q: Is ulcerative colitis the same as Crohn’s disease? A: No, while both are inflammatory bowel diseases, they differ significantly. Ulcerative colitis affects only the colon’s inner lining in a continuous pattern, while Crohn’s disease can affect any part of the digestive tract and involves all layers of the bowel wall.
Q: Can diet cure ulcerative colitis? A: No specific diet can cure ulcerative colitis, but certain dietary changes may help manage symptoms during flare-ups. It’s important to work with your healthcare provider and possibly a dietitian to identify trigger foods and maintain proper nutrition.
Q: Will I need surgery for ulcerative colitis? A: Surgery is typically reserved for severe cases that don’t respond to medication or when serious complications develop. About 25-30% of people with ulcerative colitis eventually require surgery, but many live well with medical management alone.
Q: Can I have children if I have ulcerative colitis? A: Yes, most people with ulcerative colitis can have children. However, it’s important to discuss family planning with your healthcare provider, as some medications may need adjustment during pregnancy, and timing conception during remission periods is generally recommended.
Q: How often should I have colonoscopies? A: Screening recommendations vary based on disease extent and duration. Generally, people with extensive colitis should begin surveillance colonoscopies 8-10 years after diagnosis, then every 1-2 years. Your gastroenterologist will determine the appropriate schedule for your specific situation.
Q: Is ulcerative colitis considered a disability? A: Ulcerative colitis can qualify as a disability under certain circumstances, particularly if symptoms significantly impact your ability to work or perform daily activities. The severity and frequency of symptoms, as well as response to treatment, are factors considered in disability evaluations.
Q: Can stress cause ulcerative colitis flare-ups? A: While stress doesn’t cause ulcerative colitis, it may trigger flare-ups in some people. Managing stress through relaxation techniques, regular exercise, and adequate sleep may help reduce the frequency and severity of symptoms.
References
- https://www.mayoclinic.org/diseases-conditions/ulcerative-colitis/symptoms-causes/syc-20353326
- https://www.ncbi.nlm.nih.gov/books/NBK459282/
- https://medlineplus.gov/genetics/condition/ulcerative-colitis/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC6554330/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC2725331/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC9498229/
In this Article






















