Memory, thinking, conduct, and the capacity to carry out daily tasks are all impacted by dementia, a degenerative illness. It is a group of symptoms brought on by brain illnesses like Alzheimer’s disease rather than a single infection.
Dementia is not a normal aspect of growing older. It refers to a collection of symptoms that emerge when a disease affects the brain. The term “risk factors” refers to the wide range of variables that can raise an individual’s likelihood of getting dementia.
Medical, behavioral, and environmental variables are among the various categories of risk factors for dementia. While you cannot control some risk factors, you can avoid others.
The likelihood that someone may have dementia at some point in their life is their “risk” of developing it. While dementia is a possibility for everyone, some people are more susceptible than others. These individuals are “at higher risk.”
Your brain health may be affected for a long time if you develop it in your 40s, 50s, or 60s. The age of onset is essential, according to the study, and earlier diagnoses are associated with a higher risk. Taking proactive measures during these years can help maintain mental acuity and memory long into old age.
Read More: 9 Essential Tips for a Dementia-Friendly Environment
How Midlife Health Affects Brain Function
Subtle changes in the brain start long before overt symptoms show up, making midlife a critical time. At this point, the brain’s volume may begin to decrease gradually, especially in the regions in charge of memory and judgment.
Researchers examined the timing and the combination of around 46 chronic illnesses by analyzing data from more than 280,000 participants in the UK Biobank. They discovered that before receiving a dementia diagnosis, up to 80% of patients had two or more medical disorders.
One crucial factor was the age at which these disorders appeared:
Before the age of 55, researchers found the strongest correlations with eventual dementia in heart disease, atrial fibrillation, and diabetes.
Stroke, anxiety, and depression were most strongly associated with increased risk between the ages of 55 and 70.
These findings suggest that certain diseases may have the most significant impact on brain health during “critical time windows.”
There were some alarming findings from a recent study on the lifetime risk of dementia in the United States: Between the ages of 55 and 95, people face a 42% lifetime risk of dementia. By 2060, experts project 1 million yearly cases of dementia—about twice the 514,000 cases reported in 2020. Currently, around 6 million Americans have dementia.
“Something that our society really wrestles with is how to deal with people who need intensive, long-term care in older age,” says Elizabeth Selvin, PhD ’04, MPH, a study co-author, professor in Epidemiology, and director of the Welch Center for Epidemiology and Clinical Research.
However, researchers say the message of the study is not one of “doom and gloom.” Rather, the findings present an opportunity to address dementia risk factors and take steps in middle age to prevent or slow the onset of dementia later in life.
Condition #1: High Blood Pressure
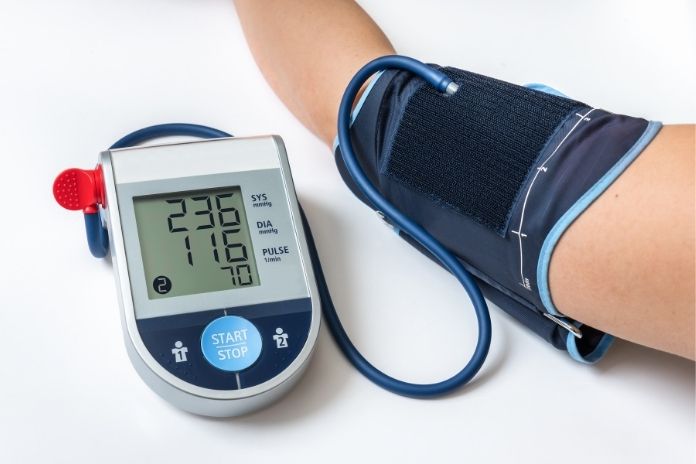
Maintaining blood pressure within a reasonable range has long been known to help prevent heart attacks and strokes. Now, a new risk that is worth avoiding has been discovered by a recent Johns Hopkins University study: Compared to people with regular blood pressure readings, those with high blood pressure in their midlife experienced a higher loss in critical thinking abilities later in life.
The findings are noteworthy despite the slight difference, which is comparable to an additional 2.7 years of brain aging on average when research participants were in their 70s, 80s, and 90s. This cognitive decline might not be sufficient for most people to perceive the difference, but it might be enough for someone to be diagnosed with dementia or mild cognitive impairment.
Read More: Illiterate people are at higher risk of developing dementia, new study reveals
Condition #2: Type 2 Diabetes

Individuals with diabetes are 100% more likely to acquire vascular dementia and have a 73% greater risk of dementia overall. Some traits of Alzheimer’s disease and type 2 diabetes are similar, including oxidative damage and compromised insulin signaling.
Type 2 diabetes harms blood vessels and causes inflammation in the brain and other parts of the body. Persistently elevated blood sugar levels have hampered memory, learning, and decision-making for many years.
According to a study, diabetes identified before midlife has been particularly detrimental to long-term brain function, highlighting the importance of early blood sugar control as a preventative measure.
Effective diabetes management is essential for long-term brain health, and the first stages in controlling diabetes are a nutritious diet, regular exercise, and weight control.
Condition #3: Obesity

According to epidemiological research, those who are obese in their middle years are more likely to develop dementia than those who maintain a good, healthy weight. Obesity raises the risk of diabetes and hypertension, two conditions linked to a higher risk of dementia.
According to a study on individuals with mild cognitive impairment, researchers linked a normal body mass index (BMI under 25), increased physical activity, and a healthy diet to decreased levels of plaques and tangles, which indicate Alzheimer’s disease.
Condition #4: High Cholesterol

Our livers produce the majority of the cholesterol in our blood. It is necessary for several bodily functions, including the synthesis of vitamin D and hormones. Cholesterol comes in various forms, some of which are harmful and others of which are beneficial.
In our 40s, 50s, and 60s, having elevated LDL cholesterol (bad cholesterol) is linked to a higher risk of dementia. In our 30s to 60s, having low levels of HDL cholesterol (good cholesterol) can also raise our risk of dementia.
Amyloid and tau are two proteins that can accumulate in the brain as a result of high cholesterol levels. Alzheimer’s disease is closely associated with these proteins. According to research, lowering cholesterol levels may lessen the quantity of amyloid that accumulates in our brains.
High blood levels of LDL cholesterol can also raise our risk of stroke. Blockages or ruptures in the blood vessels supplying the brain damage brain cells and cause strokes. Vascular dementia develops in nearly one out of every three stroke survivors.
Condition #5: Depression

Depressive episodes are associated with an increased risk of dementia, and this association seems to be strongest in later life.
Measurable alterations in the brain, like decreased volume in the hippocampus and prefrontal cortex, can result from depression. Additionally, it interferes with sleep, food, and motivation in daily life—all of which, if compromised for an extended length of time, can lead to cognitive deterioration.
Crucially, the results imply that depression might not only be an early sign of dementia but also contribute to an increased risk, particularly if it appears in midlife. Some antidepressants may reduce Alzheimer’s disease indicators, according to preliminary research.
Read More: Connected Brain Networks Can Spread Dementia, New Study Suggests
Condition #6: Sleep Apnea

According to a Michigan Medicine study, dementia in people, especially women, is exacerbated by a prevalent but underdiagnosed sleep condition.
To ascertain the possible impact of known or suspected obstructive sleep apnea on the risk of dementia, researchers looked at survey and cognitive screening data from approximately 18,500 persons.
Bouts of limited or disturbed breathing typify the persistent sleep disease known as obstructive sleep apnea while you sleep. Having known as obstructive sleep apnea or its symptoms, which many individuals are unaware they have, was linked to an increased risk of dementia symptoms or a diagnosis in the years to come for all adults 50 and older.
“Our findings offer new insight into the role of a treatable sleep disorder on long-term cognitive health at the population level for both women and men,” said first author Tiffany J. Braley, M.D., M.S., neurologist, director of the Multiple Sclerosis/Neuroimmunology Division and co-founder of the Multidisciplinary MS Fatigue and Sleep Clinic at University of Michigan Health.
Condition #7: Chronic Stress

Researchers examined the connection between performance on a range of brain function tests and cortisol levels. The findings showed that those with the highest cortisol levels did worse on measures of attention, memory, organization, and visual perception.
Researchers also observed that brain alterations, recognized as predisposing factors for Alzheimer’s disease and other forms of dementia, strongly correlated with high cortisol levels. In those with the highest cortisol levels, these changes appeared so clearly that a brain MRI scan could detect them.
Condition #8: Smoking

Smoking is widely recognized as damaging to both lungs and the heart. However, smokers and medical professionals alike frequently pay less attention to the harm tobacco causes to the brain than is necessary.
The risk of dementia is increased by smoking, according to compelling data. This takes into account whether an individual smokes during middle age or later in life.
Vascular disorders, or issues with the heart and blood vessels, are more likely to occur among smokers. These vascular problems are also linked to Alzheimer’s disease and vascular dementia, the two most common forms of dementia.
Additionally, toxins in cigarette smoke cause cell stress and inflammation, both of which researchers have linked to Alzheimer’s disease.
Read More: New Study shows that both abstinence and excess consumption of alcohol increase risk of Dementia
Condition #9: Heart Stroke

According to the Oxford study, stroke was one of the best indicators of dementia. Strokes, no matter how big or small, harm brain tissue and break connections between different parts of the brain.
Researchers have shown that strokes between the ages of 55 and 70 double the risk of dementia. Prevention by lowering blood pressure, controlling cholesterol, and engaging in regular exercise could thereby significantly lower the number of dementia cases worldwide.
Prevention & Lifestyle Tips
In general, maintaining a healthy lifestyle may help address risk factors linked to Alzheimer’s and related dementias, even if there is no proven prevention or effective treatment for these conditions.
Determine and Manage High Blood Pressure: High blood pressure (hypertension) affects more than just the heart, blood vessels, and brain, and is an additional risk factor for stroke and vascular dementia. Knowledge exists that we may decrease the risk of dementia when we can treat hypertension with medication and practice lifestyle changes, including physical activity and cessation of smoking when possible.
Promote Reduction in Air Pollution: Evidence has been accumulating that air pollution, including chemicals as well as tiny particles/particulates produced by companies and vehicles, is associated with dementia, cognitive decline, and early mortality. Positively, there appears to be a decreased risk of dementia over time when air quality improves.
Manage and Control High Blood Sugar: High blood sugar or glucose generates an increased risk for heart disease, stroke, dementia, and cognitive deficit. Specifically, people with diabetes have an increased brain disease directly to high blood glucose. A positive note is the control of blood sugar by good food choices that promote good health, regular physical activity, smoking cessation, and monitoring blood sugar levels.
Eat a balanced diet: A balanced diet which includes moderating other fats and carbohydrates regularly with intake of fruit, vegetables, whole grains, lean meats/seafood, low-fat/nonfat dairy products, and unsaturated fats (olive oil in moderation).
Reduce the chance of Head Injury: Physical assault to the brain by way of traumatic brain injury (TBI) may impair the normal function of the brain. Wear seat belts in cars, wear the appropriate gear when playing contact sports or riding a bike, and consult a doctor as soon as you suspect a concussion or traumatic brain injury.
Continue to be Mentally Engaged: Engaging your mind can be achieved through various activities, such as reading, playing board games, taking up a new hobby, learning a new skill, working or volunteering, and interacting with others.
Read More: How Chronic Stress Shrinks Your Brain (and What to Do About It)
Conclusion
Midlife is a critical period for determining your brain’s long-term health. Your decisions between the ages of 40 and 60 can either prevent cognitive decline later in life or save your memory and thinking abilities. For years before symptoms show up, conditions including depression, high blood pressure, diabetes, obesity, and high cholesterol can cause quite harm to blood vessels and brain cells.
The good news is that you can always take action at any time. Make routine health examinations a priority, treat chronic conditions promptly, and adopt a healthy lifestyle that incorporates stress reduction, regular exercise, a balanced diet, and mental stimulation. Midlife offers a key chance to safeguard your brain, one of your most valuable assets.
References
- https://timesofindia.indiatimes.com/life-style/health-fitness/health-news/6-midlife-health-conditions-that-can-raise-dementia-risk-oxford-study-reveals/articleshow/123272540.cms
- https://www.msn.com/en-in/health/other/6-midlife-health-conditions-that-can-raise-dementia-risk-oxford-study-reveals/ar-AA1KqL5t
- https://uk.news.yahoo.com/health-conditions-may-increase-risk-233000952.html
- https://www.alzheimers.org.uk/sites/default/files/pdf/factsheet_risk_factors_for_dementia.pdf
- https://www1.racgp.org.au/newsgp/clinical/list-of-dementia-risk-factors-grows
- https://www.mayoclinic.org/diseases-conditions/dementia/symptoms-causes
- https://publichealth.jhu.edu/2025/preventive-steps-in-midlife-can-help-to-lower-dementia-risk
- https://www.hopkinsmedicine.org/health/wellness-and-prevention/hidden-brain-risk-midlife-high-blood-pressure
- https://publichealth.jhu.edu/faculty/1882/elizabeth-selvin
- https://publichealth.jhu.edu/welch-center-for-prevention-epidemiology-and-clinical-research
- https://www.comfortinghome.com/posts/15-dementia-risk-factors
- https://www.hopkinsmedicine.org/health/conditions-and-diseases/high-blood-pressure-hypertension
- https://www.alzdiscovery.org/cognitive-vitality/blog/nine-lifestyle-factors-may-lower-your-alzheimers-risk
- https://pubmed.ncbi.nlm.nih.gov/28761927/
- https://www.alzheimersresearchuk.org/dementia-information/dementia-risk/cholesterol-and-dementia-risk/
- https://www.alzheimers.org.uk/about-dementia/managing-the-risk-of-dementia/possible-risks-of-dementia/cholesterol
- https://www.uofmhealth.org/profile/1343/tiffany-joy-braley-md
- https://www.michiganmedicine.org/health-lab/sleep-apnea-contributes-dementia-older-adults-especially-women
- https://pubmed.ncbi.nlm.nih.gov/24828079/
- https://www.ganeshdiagnostic.com/news.php
- https://www.orlandohealth.com/content-hub/how-stress-increases-dementia-risk
- https://www.alzheimers.org.uk/about-dementia/managing-the-risk-of-dementia/reduce-your-risk-of-dementia/smoking
- https://www.heart.org/en/news/2021/07/06/smoking-harms-the-brain-raises-dementia-risk-but-not-if-you-quit
- https://www.michiganmedicine.org/health-lab/11-ways-reduce-your-risk-dementia
- https://www.alzheimers.gov/life-with-dementia/can-i-prevent-dementia
In this Article


















