Endometriosis affects approximately 1 in 10 women, but many spend years silently suffering before they are diagnosed. They’re frequently reassured that their pain is “just part of being a woman” or, worse, told it’s “all in their head.” This health neglect waits out treatment, harms quality of life, and perpetuates a pattern of perpetual pain in women being ignored and not understood.
So, what is endometriosis like? And why is it so very commonly misdiagnosed?
Let’s debunk the experience of endometriosis pain, why it’s so commonly confused with something else, and how you can push for answers.
Read More: Holistic Menstrual Health: Comprehensive Strategies for Easing Menstrual Discomfort
What Is Endometriosis?

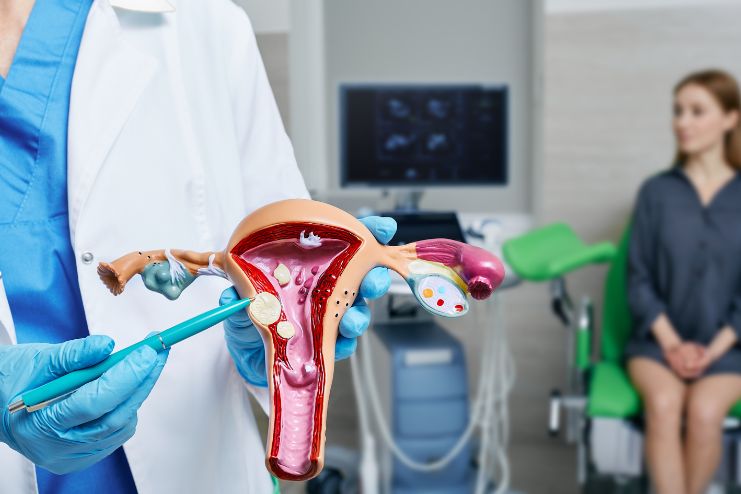
Endometriosis occurs when tissue that is identical to the lining of the uterus (endometrium) develops outside the uterus—on the ovaries, fallopian tubes, bladder, bowels, and even the diaphragm or lungs in very rare situations. This out-of-place tissue acts just like regular endometrial tissue: it thickens, breaks down, and bleeds with every menstrual cycle.
But unlike the uterine lining, this tissue has nowhere to go. It causes inflammation, scarring, pelvic pain, and adhesions that cause organs to stick together.
Why is diagnosis even more difficult? This tissue isn’t always detectable on ultrasounds or imaging. Many don’t get a diagnosis until they have a laparoscopy—a minimally invasive surgery that allows doctors to directly see and biopsy the lesions.
What Endometriosis Pain Feels Like
Endometrosis pain can be terrible. Here’s how it actually feels:
1. Pelvic Pain That’s More Than “Just Cramps”
This is not your typical period pain. Pelvic pain and endometriosis tend to feel like:
- Stabbing, searing, or burning pain that persists or gets worse over time
- Deep, nagging sensations in the lower abdomen or pelvic area
- Pain that radiates to the lower back, hips, or legs
This pain may not follow a predictable cycle and can hit you even when you aren’t menstruating.
“It was like a knife turning inside of me,” one woman reported in Fertifa’s patient histories.
2. Severe Menstrual Cramps That Disrupt Daily Life
Endometriosis pain vs. period pain is like a paper cut compared to an open wound.
Endo women tend to:
- Have cramps beginning days before periods
- Take time off from school or work each month
- Still hurt after the bleeding stops
This is not “bad periods”—this is chronic pain that disrupts life.
3. Pain During or After Sex (Dyspareunia)
Pain during sex is a sign of endometriosis, especially with deep penetration. Pain can feel:
- Sharp or throbbing that is deep
- Lasting for hours or even extending to the next day
Unfortunately, this painful symptom is usually shrugged off as psychological or attributed to anxiety, particularly in younger women.
4. Pain With Bowel Movements or Urination
Endometriosis can impact the bowel and bladder. Symptoms may include:
- Irritable bowel syndrome (IBS)
- Urinary tract infections (UTIs)
- Rectal cramping or painful bowel movements
- Urinary burning or urgency, particularly during menstruation
These GI symptoms and endo signs are quite commonly misdiagnosed as gut or bladder problems, causing additional delays in diagnosis.
5. Chronic Fatigue and “Endo Belly”
Ever heard of endo belly? It’s what women call the painful bloating, pressure, and distension they experience in their belly, often on a cyclical basis.
- Bloating that resembles a food intolerance
- A belly that visibly puffs up during flare-ups
- Fatigue that’s like getting hit by a truck, and usually unrelated to sleep
According to Dr. Boz, MD, these symptoms are often misattributed to gluten sensitivity, food intolerances, or stress.
Read More: Understanding Pelvic Health: Common Issues and Maintenance Tips
Why Endometriosis Is So Often Misdiagnosed

Endometriosis can often be misdiagnosed. Here are a few reasons:
- Symptoms Overlap With Other Conditions:
Endometriosis may present itself like:
- IBS
- Pelvic inflammatory disease
- Ovarian cysts
- Interstitial cystitis
- Fibroids
- UTIs
Which is why it’s frequently misdiagnosed—or simply overlooked.
Endometriosis misdiagnosis is so common that one FCI article reports it as being mistaken for between one and eight other conditions.
- Medical Gaslighting and Bias:
Too frequently, women, particularly young, Black, or Brown women, are dismissed, having their symptoms labeled as “normal” or “psychosomatic.” As Yale Medicine states, this dismissal represents a significant obstacle to diagnosis.
This process, referred to as medical gaslighting, postpones treatment and has many doubting themselves about their pain.
- No Non-Invasive Diagnostic Test:
Imaging and blood tests typically don’t detect endometriosis unless there are visible endometriomas (ovarian cysts). The only right diagnosis is through laparoscopy, which many physicians are reluctant to prescribe early.
That’s why the endometriosis diagnosis can get delayed up to even 7 years.
- Hormonal Birth Control May Mask Symptoms Temporarily:
Hormonal medications can quiet symptoms, but they don’t treat the underlying cause. So, individuals often think they’re “okay” for years, until symptoms increase.
Read More: Fibroids vs. Ovarian Cysts: Know the Difference
Other Clues That It Could Be Endometriosis
Curious if your pain might be more than awful periods? Here are a couple of red flags:
- Difficulty getting pregnant
- History of endo, fibroids, or autoimmune diseases in the family
- Ache that worsens with ovulation
- Cyclical bladder, bowel, or nerve symptoms
- Chronic pain after typical imaging or lab work
Some individuals have silent endometriosis, which results in infertility or nonspecific symptoms with minimal or no pain during periods. And, as highlighted in this Fertifa article, tracking these patterns can offer critical clues for diagnosis.
How to Advocate for a Diagnosis
Obtaining answers begins with self-advocacy. Here’s how:
- Monitor your symptoms. Maintain a comprehensive pain and symptom calendar.
- Request a referral to a gynecologist with expertise in endometriosis
- If symptoms do not improve with treatment, ask for a laparoscopy
- Push for second opinions even if your pain is reduced, and you still have doubts
- You know your body best. Don’t be afraid to say, “This isn’t normal.” This helps you get control and make the right decision.
Treatment Options Once Diagnosed
While there’s no permanent cure, many women find relief with the right combination of treatments:
- Hormonal therapies (e.g., birth control, GnRH agonists) to suppress lesion growth
- Laparoscopic excision surgery, the gold standard treatment, removes lesions without just burning them
- Pelvic floor physical therapy to relax muscle tension and enhance function
- Anti-inflammatory diets and lifestyle modifications to minimize flares
- Mental health counseling to deal with the stigma of chronic pain
- Treatment must be tailored, not universal
Read More: What Your Period Blood Color Says About Your Health
Final Thoughts

Endometriosis pain is real, but often misunderstood. It’s not “just cramps” or “bad periods.” It’s a chronic illness that needs early diagnosis, precise diagnosis, and compassionate, informed treatment.
If your pain is interfering with your life, trust yourself. You deserve answers. You deserve relief. The more we talk about endometriosis, the closer we get to better care for everyone affected.
References
- https://www.fertifa.com/post/endometriosis-pain
- https://pmc.ncbi.nlm.nih.gov/articles/PMC9175578/
- https://www.yalemedicine.org/news/endometriosis-is-more-than-painful-periods
- https://www.drbozmd.com/blog/6-endometriosis-imposters-that-could-delay-a-correct-diagnosis-and-wreck-your-future
- https://www.fertifa.com/post/endometriosis-pain
- https://www.fcionline.com/article/8-endometriosis-symptoms-misdiagnosed/
- https://www.yalemedicine.org/news/endometriosis-is-more-than-painful-periods
In this Article

















