If you’ve had a blocked nose that never really clears, even with nasal sprays or allergy medicines, you may be dealing with nasal polyps. Symptoms of nasal polyps include a blocked nose that is difficult to clear, even with the use of nasal sprays or allergy medications.
Nasal polyps are soft growths that occur in the lining of your nasal passages or sinuses. Due to chronic inflammation, these develop in the lining of your nasal pathways or sinuses. As time passes, they might enlarge and cause breathing difficulties. Also, polyps might reduce one’s sense of smell and taste, and increase the risk of frequent sinus infections.
While they are harmless, the effects of nasal polyps can be intense. They often appear in individuals with chronic sinus problems, asthma, or aspirin sensitivity. Understanding what they are, why they form, and when to seek medical help is key to preventing long-term nasal and respiratory problems.
In this article, we will look into the causes, symptoms, diagnosis, and treatment options for nasal polyps. Let’s also learn more about ways to deal with them and prevent them in the future.
Read More: 12 Effective Remedies to Stop Post Nasal Drip At Home
Quick Summary: What You’ll Learn
- What nasal polyps are and how they develop inside the nasal passages.
- Common causes and risk factors associated with chronic inflammation.
- Typical and red-flag symptoms that indicate when a referral to an ENT specialist is necessary.
- How doctors diagnose nasal polyps and what tests to expect.
- Treatment options, from sprays to surgery, plus lifestyle tips for prevention.
What Are Nasal Polyps? Anatomy and Pathophysiology

Nasal polyps are small, painless, tear-shaped growths that form on the lining of your nasal passages or sinuses. They most often occur in the ethmoid sinuses, which are situated between the eyes, but can develop anywhere in the nasal cavity.
As with any inflammation, the tissue inside the nose becomes swollen and waterlogged over time. This inflamed tissue eventually bulges outward, forming a soft, jelly-like mass called a polyp.
These growths can be small or large. Small polyps might not be noticeable, but larger ones, or clusters, can block airflow through the nose. The large polyps block sinus drainage and lead to chronic congestion. While these are not malignant tumors, nasal polyps are indeed benign; however, they might lead to serious conditions if they grow extensively.
Chronic inflammation is one of the primary reasons for developing nasal polyps. The release of various inflammatory mediators, including interleukins (IL-5, IL-13), and eosinophils maintains the swelling and tissue changes. Over time, this leads to what is called Type-2 or Th2 inflammation, which is common in people with CRSwNP.
Not all polyps are the same. Some are Th2-driven and highly inflammatory, while others are non-Th2 types dominated by neutrophilic inflammation. Understanding this difference is essential because Th2-driven polyps often respond to corticosteroid sprays or biologic therapies. While the non-Th2 types may be resistant to any or all of these.
Evidence Box A:
A 2016 Annual Reviews study found that epithelial barrier damage and Type 2 cytokines (IL-5, IL-13) drive chronic inflammation and tissue remodeling in the development of nasal polyps.
Read More: Can Holding in a Sneeze Damage Your Brain or Ears? What Doctors Say
Causes and Risk Factors
Nasal polyps form through chronic inflammation of the mucous membrane lining the nasal passages or sinuses. This can be caused by allergies, infections, immune disorders, or even structural issues that may obstruct normal drainage from the sinuses.
Main Causes Include:
- Chronic Inflammation: Prolonged sinus or nasal inflammation, also called chronic rhinosinusitis, is the most common underlying cause.
- Asthma and Allergic Rhinitis: Both conditions share common inflammatory pathways that make the nasal lining more reactive.
- Aspirin-Induced Respiratory Disease: This condition encompasses a combination of asthma, aspirin intolerance, and nasal polyps.
- Environmental Irritants: Factors such as pollution, dust, chemical fumes, and cigarette smoke can all irritate the nasal tissue.
- Bacterial or Fungal Colonization: The chronic presence of these microbes, particularly Staphylococcus aureus, exacerbates localized immune responses.
- Genetic and Systemic Conditions: Cystic fibrosis, primary ciliary dyskinesia, and immune deficiencies may predispose some patients to the development of polyps.
People with asthma, chronic sinusitis, allergic rhinitis, or a family history of nasal polyps are more at risk. The condition can be worsened by repeated infections of the respiratory pathways, a weakened immune system, and staying in areas with high pollution or humidity.
Evidence Box B:
A 2020 BioMed Central study linked higher IL-6 levels to airway epithelial dysfunction, worsening inflammation in chronic rhinosinusitis with nasal polyps.
Symptoms: What to Look For
The symptoms of nasal polyps can be quite broad and often resemble common sinus or allergy issues. The difference is that the symptoms persist, without any improvement, rather than appearing and disappearing in episodes.
Common Symptoms:
- Continuous nasal congestion or blockage
- Reduced or complete loss of smell (hyposmia or anosmia)
- Runny nose and postnasal drip
- Facial pressure or fullness, most commonly around the eyes and cheeks
- Sinus infections that are chronic and resistant to treatment with antibiotics
- Snoring or mouth breathing from obstructed airflow
Less Common Symptoms:
- Headaches or a heavy feeling in the face
- Reduced taste
- Sleep disturbances, or worsening of existing sleep apnea
When to be Concerned:
Alarming symptoms of nasal polyps include unilateral nasal obstruction, bleeding, or sudden loss of smell, which should be given immediate medical attention. Symptoms persisting beyond 12 weeks may indicate chronic rhinosinusitis with nasal polyps, requiring an evaluation by an ENT specialist.
Evidence Box C:
A PubMed Central review estimated that nasal polyps affect up to 4% of the general population, particularly adults with chronic sinus issues.
Diagnosis: How Doctors Confirm Nasal Polyps
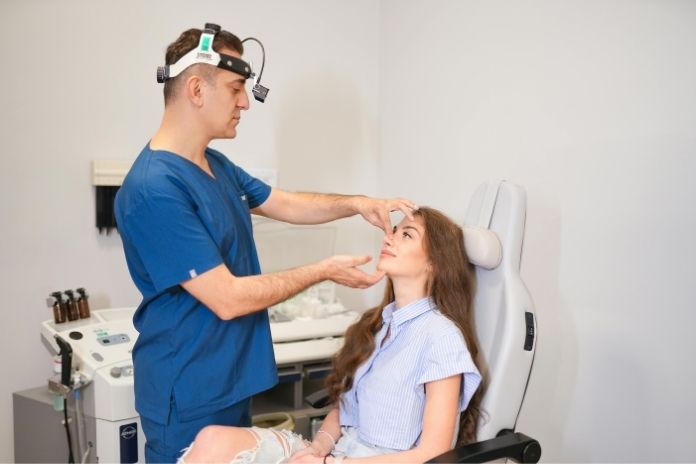
The diagnosis of nasal polyps is based on physical examination, imaging studies, and, in some cases, laboratory examinations. Your ENT specialist begins with a thorough history-taking to understand the chronicity of symptoms and possible causative factors.
Key diagnostic steps include:
- Nasal Endoscopy: A small, flexible camera is inserted into the nasal passages, allowing for direct visualization of polyps and inflammation.
- CT Scan of the Sinuses: This procedure provides a three-dimensional view of the sinus anatomy and assesses the extent of blockage. It is also important in the planning of surgery when required.
- Allergy Testing: Pinpoints allergic triggers that may be at the root of chronic inflammation.
- Blood Tests: These can be used to detect the level of eosinophils or IgE, which indicate allergic or inflammatory activity.
- Differential Diagnosis: The physician makes sure that symptoms are not caused by tumors, fungal infections, or structural deformities.
You can expect a nasal examination, sometimes followed by saline rinsing to clear the nasal passages of mucus. Also, the doctor might suggest imaging if he suspects a bigger blockage.
Read More: Can You Train Your Nose to Smell Again? The Science of Smell Therapy
Treatment Options and When to Get Checked
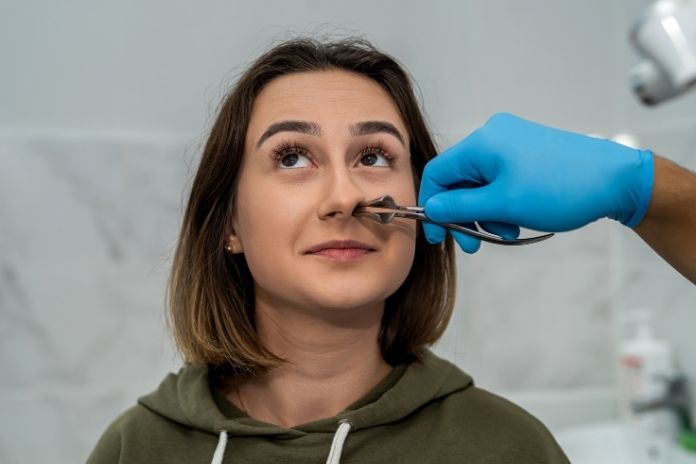
“Nasal polyps are usually treated with medications first, such as nasal steroid sprays, oral steroids, and nasal saline irrigations,” said Dr Kevin Hur, MD, a rhinology specialist with the USC Caruso Department of Otolaryngology – Head and Neck Surgery. Adding, “If left untreated, polyps can grow and obstruct the openings of the sinuses into the nasal cavity, causing difficulty sleeping, postnasal drip, fatigue, and facial pressure.”
Medical Management:
- For most people, treatment begins with medications aimed at shrinking polyps and reducing inflammation.
- Regular use of nasal corticosteroid sprays helps shrink polyps and alleviate congestion.
- Every day, rinsing with saline clears mucus, reduces irritation, and promotes the absorption of medication.
- Short-term oral steroids are used to control severe inflammation, but are not suitable for long-term use because of side effects.
- Antihistamines or leukotriene modifiers are an effective option for patients with allergic triggers.
- Biologic therapies include injectable drugs, such as dupilumab or omalizumab, that target specific inflammation pathways in CRSwNP and are effective for severe or recurrent forms of the disease.
Surgical Management:
If medical treatments are not effective, endoscopic sinus surgery can be suggested. During this less invasive procedure, surgeons remove polyps and clear blockages within the sinuses. The procedure is performed with the assistance of a small camera and specialized instruments, improving airflow and enabling medications to work more effectively.
Recovery generally takes a few weeks; however, maintenance therapy is important, as recurrence rates remain high if inflammation is not kept under control.
When to see a doctor:
Seek medical attention if nasal congestion, loss of smell, and recurrences of sinusitis continue and do not improve with conventional medication. If the symptoms persist even after treatment, it means you need more specialized care or advanced therapy.
Living with Nasal Polyps and Self-Care Tips

Long-term management of nasal polyps includes controlling inflammation and preventing its recurrence. Changing one’s lifestyle and continuing care even after surgery or successful medical treatment is essential.
Self-Care and Prevention Tips:
- Use regular saline rinses. They help keep nasal passages clean and reduce exposure to allergens.
- Maintain a clean and humid environment by using air purifiers and humidifiers to reduce irritants and dryness.
- Avoid irritants. Avoid exposure to cigarette smoke, air pollution, and strong chemical odors.
- Manage allergies and asthma by following treatment plans as prescribed to reduce inflammation.
- Stay hydrated and sleep well. Proper hydration keeps mucus thin; restful sleep helps regulate the immune system.
- Monitor your symptoms. Keep a symptom diary for nasal congestion, smell changes, and infections to identify early warning signs of recurrence.
The risk of nasal polyps recurring is as high as 80% if the underlying inflammation is not managed, hence the necessity for maintenance sprays and follow-up visits.
Quick Summary
Nasal polyps are benign yet troublesome growths resulting from chronic inflammation of the nasal passages. They may create constant congestion, a reduced sense of smell, and repeated sinus infections. These symptoms are often accompanied by other conditions such as asthma or allergic rhinitis.
Nasal polyps are typically diagnosed through nasal endoscopy and imaging to determine their extent. While most people will improve with corticosteroid sprays and saline rinses, stubborn cases may need therapies or surgery.
Long-term management requires proper and regular nasal care, avoiding triggers, and continued medical surveillance to suppress inflammation and prevent recurrence.
FAQs
Are nasal polyps cancerous?
No, all nasal polyps are malignant; however, every unilateral growth and bleeding should be subjected to medical scrutiny to rule out malignancy.
Can nasal polyps disappear on their own?
Small polyps may shrink with consistent use of nasal steroids, but most require ongoing treatment to prevent regrowth.
Why do nasal polyps affect smell?
Polyps obstruct airflow to the olfactory area and secrete inflammatory chemicals, which impede the normal functioning of smell receptors.
What’s the connection between asthma and nasal polyps?
Both conditions involve Type 2 inflammation, which causes swelling in the airways and sinuses. People with asthma are more likely to have polyps, especially when they are aspirin-sensitive.
Can nasal polyps occur in children?
Yes, but it’s not common. In cases when they do, doctors often check for cystic fibrosis or immune disorders.
How frequently do nasal polyps recur post-surgery?
Recurrence rates are high unless the inflammation is carefully looked after. Consistent use of sprays and saline rinses, along with follow-up visits, significantly reduces the risk.
Are there natural remedies that may help?
While natural methods can’t remove polyps, saline rinses, steam inhalation, and allergen control can ease symptoms.
When should I see an ENT?
Chronic nasal obstruction or diminished sense of smell lasting longer than 12 weeks, or symptoms that worsen despite medication, would require a visit to the ENT for evaluation.
References
- National Center for Biotechnology Information. (2024). Chronic Rhinosinusitis with Nasal Polyps (CRSwNP). In StatPearls.
- Carolina Asthma and Allergy Center. (n.d.). Nasal Polyps.
- Tender Palm Hospital. (n.d.). Nasal Polyps Treatment in Lucknow, India.
- Northwestern Medicine. (n.d.). Nasal & Sinus Polyps: Causes and Diagnoses.
- Hulse, K. E., Stevens, W. W., Tan, B. K., Schleimer, R. P. (2021). Pathogenesis of nasal polyposis. Annual Review of Pathology: Mechanisms of Disease, 16(1), 195–219.
- Li, X., Meng, J., Qiao, X., Liu, Y., Liu, F., Zhang, N., & Bachert, C. (2021). Immune mechanisms in chronic rhinosinusitis with nasal polyps: Development of animal models. Journal of Translational Medicine, 19(1), 1–13.
- Cao, P. P., Li, H. B., Wang, B. F., Wang, S. B., You, X. J., Cui, Y. H., & Liu, Z. (2021). Distinct immunopathologic characteristics of various types of chronic rhinosinusitis in adult Chinese. Frontiers in Immunology, 12, 841618.
- Kim, D. K., Jin, H. R., Eun, K. M., Kim, D. Y., Cho, S. H., & Kim, D. W. (2024). The IL-4/IL-13 signaling pathway in nasal polyp development and chronic rhinosinusitis. Frontiers in Immunology, 15, 11059040.
In this Article


















