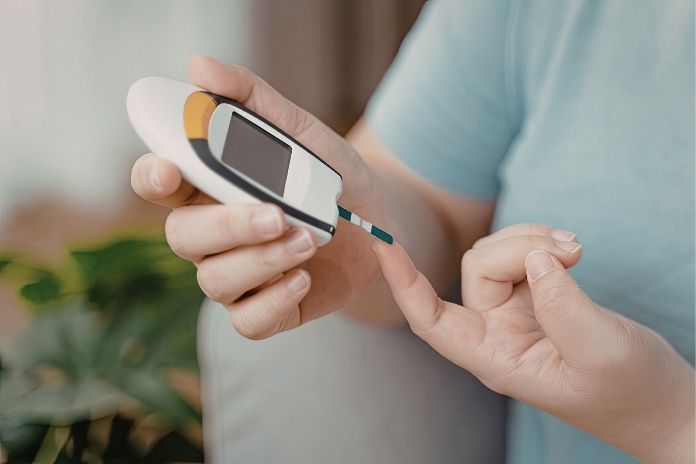
- Euglycemic DKA occurs without high blood sugar, making detection more difficult.
- SGLT2 inhibitors can raise ketone production, triggering ketoacidosis despite normal glucose.
- Nausea, fatigue, or rapid breathing may signal ketoacidosis and require urgent care.
The majority of people with diabetes associate significantly elevated glucose levels with diabetic ketoacidosis without high blood sugar. Diabetic ketoacidosis (DKA) is characterized by a sharp increase in blood glucose and the accumulation of hazardous acids known as ketones in the blood.
However, even when blood sugar levels seem normal, or only slightly raised, euglycemic diabetic ketoacidosis, a lesser-known but increasingly recognized condition, can develop. This article defines euglycemic diabetic ketoacidosis, explains how it differs from conventional diabetic ketoacidosis, and examines why SGLT2 inhibitors cause ketoacidosis in certain people.
Read More: Soups That Don’t Spike Blood Sugar: Smart Choices for Steady Glucose Levels
What Is Euglycemic Diabetic Ketoacidosis?
Both type 1 and type 2 diabetes can result in the dangerous medical condition known as euglycemic diabetic ketoacidosis (DKA, sometimes called EDKA).
To put it simply, it is a condition in which your body is still highly acidic (arterial pH less than 7.3 and serum bicarbonate less than 18 mEq/L) and has significant quantities of ketones, but your blood sugar levels aren’t excessively high (less than 250 mg/dL).
Your body produces ketones when it breaks down fat for energy, which occurs when there is insufficient insulin to use blood sugar. One of the most serious and potentially fatal consequences of diabetes is diabetic ketoacidosis (DKA), which can be brought on by a variety of circumstances.
Interestingly, the usage of sodium-glucose transporter 2 (SGLT2) inhibitors, a class of diabetes medication, has been linked to an increased incidence of EDKA. Since the causes of EDKA can vary and the blood sugar levels stay normal, it might be challenging to diagnose. It typically delays diagnosis of the illness.
How It Differs From Traditional Diabetic Ketoacidosis
Diabetes-related emergencies include diabetic ketoacidosis (DKA) and euglycemic DKA. People who have DKA may have hyperglycemia that is much higher than 250 mg/dL.
While people with type 1 diabetes (T1DM) are more likely to experience DKA, the use of SGLT-2 inhibitors, which are typically used for type 2 diabetes mellitus (T2DM), has recently been associated with euglycemic DKA, which is characterized by mildly elevated or nearly normal blood glucose at levels below 200 mg/dL.
In the absence of the significant hyperglycemia linked to DKA, euglycemic DKA might go unnoticed by clinicians.
Why Normal Glucose Levels Can Be Misleading
Delayed diagnosis is one of the main risks associated with diabetic ketoacidosis without high blood sugar. Healthcare providers teach many people with diabetes to watch for extremely high blood sugar levels, the main indicator of ketoacidosis. However, a person’s glucose levels may remain near normal in euglycemic diabetic ketoacidosis.
Consequently:
- Patients can believe that their symptoms have nothing to do with diabetes.
- Initially, medical professionals might consider other conditions.
- It’s possible to postpone diagnosis until symptoms worsen.
Read More: 5 Ways to Support Healthy Blood Sugar With Your Daily Drinks
How SGLT2 Inhibitors Can Trigger Euglycemic DKA
It is useful first to understand how SGLT2 inhibitors work in the body to understand why they can cause ketoacidosis. SGLT2 inhibitors are a class of medications that lower blood sugar by blocking the kidneys’ reabsorption of glucose. Rather, excess glucose is excreted in the urine.
How These Medications Lower Blood Sugar
Your kidneys’ SGLT2 protein is responsible for reabsorbing glucose. A portion of the glucose in your blood usually returns to your circulation after passing through your kidneys. These drugs prevent your kidneys from reabsorbing glucose by blocking the mechanism that reabsorbs it.
Rather, it ends up in your urine. It indicates that the glucose does not enter your bloodstream, so your blood sugar does not rise.
Why Lower Glucose Can Mask Rising Ketone Levels
SGLT2 inhibitors can conceal the early warning indicators of ketoacidosis because they suppress glucose levels. The body may begin using fat metabolism as a source of energy at the same time. The liver starts to break down fat and produce ketones when less glucose is available inside cells.
This change in metabolism may result in:
- Increased ketone buildup
- Increasing blood acid levels
- Metabolic acidosisdevelopment
The Role of Insulin, Glucagon, and Ketone Formation
The development of euglycemic diabetic ketoacidosis is also significantly influenced by hormones. Normally, glucagon stimulates ketone synthesis, while insulin inhibits it. The balance shifts toward ketone production when insulin levels decrease or become insufficient.
Numerous metabolic alterations may contribute to the condition:
- Decreased action of insulin
- Elevated release of glucagon
- Improved breakdown of fat
- Increased synthesis of ketones
Symptoms of Euglycemic DKA That Should Not Be Ignored

Euglycemic diabetic ketoacidosis (EDKA) looks a lot like regular hyperglycemic DKA, but the symptoms don’t always show up the same way for everyone. People usually feel sick to their stomach, throw up, have trouble breathing, run out of energy, lose their appetite, or feel stomach pain.
Unlike classic DKA, folks with EDKA often don’t get really thirsty or pee all the time, since their blood sugar isn’t sky-high. It usually takes longer for symptoms to show up, too, because the body needs more time without food to hit ketosis and get dehydrated.
Situations That Increase the Risk of Euglycemic DKA
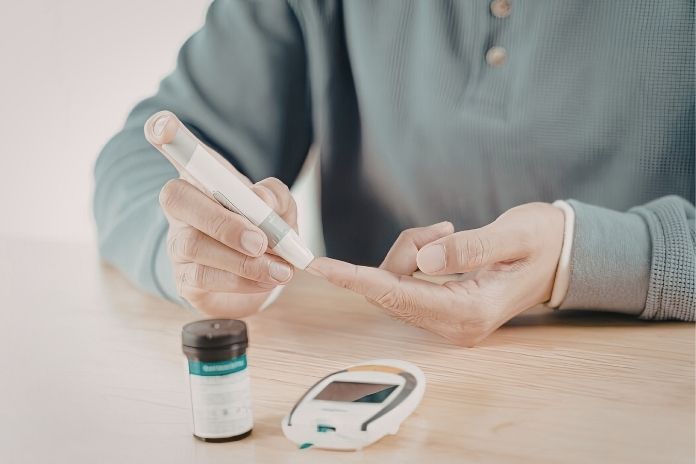
SGLT2 inhibitor DKA is more likely in several circumstances, especially when several factors occur simultaneously.
Prolonged Fasting or Very Low-Carbohydrate Diets
Because the body depends more on fat metabolism when following a very low-carb or ketogenic diet, ketone accumulation may increase. When combined with SGLT2 inhibitors, this metabolic shift may increase the risk of normal blood sugar ketoacidosis.
Acute Illness, Infection, or Surgery
When you’re sick, your body gets stressed and cranks up certain hormones. That pushes your system to make more ketones, which isn’t always a good thing. You get dehydration, and ketosis gets worse; you might not feel like eating, and suddenly, your insulin needs can change.
Reduced Insulin Use in People With Diabetes
People who reduce or stop insulin therapy while taking SGLT2 inhibitors may experience insulin deficiency, which significantly increases the risk of ketoacidosis.
Dehydration or Excess Alcohol Intake
Dehydration can raise ketone levels and exacerbate metabolic acidosis. Additionally, alcohol can disrupt insulin homeostasis and glucose metabolism.
Pregnancy or Increased Metabolic Stress
Pregnancy can change hormone levels and raise metabolic needs. These alterations may make SGLT2 inhibitor users more vulnerable to normal blood sugar ketoacidosis.
Read More: Why You Feel Weak or Dizzy After Meals, Even When Your Blood Sugar Is Normal
Who Should Be Especially Aware of This Risk?
Even though euglycemic diabetic ketoacidosis is rare, certain individuals should be especially mindful of the possibility. These populations include:
Type 1 Diabetes Using SGLT2 Inhibitors Off-Label
SGLT2 inhibitors are used off-label by certain individuals with type 1 diabetes to assist in controlling blood sugar levels. However, the risk of DKA with SGLT2 inhibitors is much higher in this group. Because of this, several recommendations for people with type 1 diabetes advise avoidance or caution.
Type 2 Diabetes Taking These Medications
People with type 2 diabetes receive the majority of SGLT2 inhibitor medications. Patients should be aware of potential SGLT2 inhibitor side effects, such as the uncommon risk of euglycemic diabetic ketoacidosis, even if the advantages of these drugs are well-established.
Recent Illness, Surgery, or Reduced Food Intake
Dehydration and ketosis are more likely during times of illness or fasting, especially if medication is taken as prescribed. For this reason, medical professionals frequently provide sick day rules for diabetes, which direct the administration of medications while ill.
How Euglycemic DKA Is Diagnosed
It takes more than just measuring blood sugar levels to diagnose euglycemic diabetic ketoacidosis. Acid-base balance, ketone levels, and symptoms are just a few of the variables that doctors must consider collectively. The first step is testing for ketones in blood or urine.
Further Laboratory Evaluation:
- Glucose
- Calcium
- Magnesium
- Creatinine
- BUN
- Ketones in urine and serum
- Beta-hydroxybutyric acid
- Arterial or venous blood gas analysis
- Lactic acid
- Chest X-ray
- ECG
- Osmolality of serum
- Alcohol
Treatment and Medical Management
Rehydrating a patient is the first step when they arrive severely dehydrated, which is frequently the case. This procedure involves administering fluids via an IV, such as lactated Ringer’s solution or isotonic saline.
These liquids help replenish your body’s electrolytes (minerals) and water, which are essential for vital processes. For the first one to two hours, the American Diabetes Association recommends starting with a high fluid intake.
Doctors will then begin an insulin infusion if the patient’s potassium level is above 3.3 mEq/L. Insulin helps control blood sugar levels. Since the patient’s blood sugar level is usually less than 250 mg/dL, sugar (5% dextrose) is added to the fluids to prevent hypoglycemia (low blood sugar) and to expedite the clearing of ketosis.
The body may lose total potassium, so doctors must monitor potassium levels carefully. Potassium is an important mineral that facilitates communication between muscles and neurons.
As a result, additional potassium and other electrolytes may need to be administered intravenously. The protocol for treating diabetic ketoacidosis (DKA), a serious consequence of diabetes, is to check blood sugar levels every hour and electrolytes approximately every four hours.
As soon as the diagnosis is made, it is critical to halt the patient’s use of SGLT2 inhibitors, a class of diabetes medications, and to suspend the prescription until the patient recovers from the acute illness. Doctors do not recommend sodium bicarbonate infusions to treat acidemia in this illness.
How People Taking SGLT2 Inhibitors Can Reduce Their Risk
While euglycemic diabetic ketoacidosis is uncommon, there are a few ways to lower the risk.
Following “Sick Day” Medication Guidance
Healthcare providers often give people with diabetes special “sick day” guidelines, explaining how to adjust their medication when they’re not feeling well.
Avoiding Extreme Carbohydrate Restriction Without Medical Advice
Very low-carb diets can make ketone buildup worse, especially if someone’s taking SGLT2 inhibitors. So, before making a big change to your diet, talk to your healthcare provider first.
Monitoring for Symptoms During Illness or Fasting
It’s crucial to identify symptoms of euglycemic DKA while unwell. Symptoms, including fatigue, nausea, or changes in breathing, should be carefully assessed.
Knowing When to Check Ketones
When unwell or experiencing symptoms, those using SGLT2 inhibitors may need to monitor their ketones; both blood and urine ketone testing can detect increased ketone levels before severe metabolic acidosis develops.
When to Seek Immediate Medical Care

Even when blood glucose levels appear normal, the following signs warrant immediate medical attention:
- When taking SGLT2 inhibitors, persistent nausea or vomiting may be a sign of SGLT2 inhibitor DKA.
- Extreme exhaustion, weakness, or rapid breathing could be signs of severe ketoacidosis emergency symptoms.
- Normal blood sugar ketoacidosis should be taken into consideration if a person with diabetes feels really sick while having normal glucose values.
Read More: Drinks That May Help Lower Blood Sugar Quickly (What Helps—and What Doesn’t)
Conclusion
Euglycemic diabetic ketoacidosis is a rare but serious condition that can happen even when blood sugar looks normal. The tricky part is that it often gets missed because people usually expect diabetic ketoacidosis to show up alongside really high glucose levels.
Medications like SGLT2 inhibitors have helped a lot of folks manage their diabetes better, but they do have a downside—they can mess with your metabolism and make SGLT2 inhibitor DKA more likely.
Early detection requires an understanding of warning signs, including chronic nausea, rapid breathing, exhaustion, or confusion.
References
- MD Searchlight. (January 29, 2023). Euglycemic diabetic ketoacidosis
- Barski, L., Eshkoli, T., Brandstaetter, E., & Jotkowitz, A. (2019). Euglycemic diabetic ketoacidosis
- StatPearls Publishing. (January 29, 2023). Overactive bladder.
- Ju, H.-H. (2025). Euglycemic diabetic ketoacidosis: How is it different from diabetic ketoacidosis
- Cleveland Clinic. (2025, July 31). SGLT2 inhibitors: What they are, uses & side effects
- Doral Health & Wellness. SGLT2 inhibitors: How do they work?
- Do Oracle. (February 20, 2025). What are the risk factors for euglycemic (normal blood glucose level) Diabetic Ketoacidosis (DKA)?
- NYSORA. Euglycemic diabetic ketoacidosis.
In this Article