Kidney stones are a painful and often serious condition, yet many women are initially misdiagnosed with a urinary tract infection (UTI) due to overlapping symptoms like pelvic pain, urinary urgency, and discomfort during urination. While both conditions affect the urinary tract, they are fundamentally different in origin and require completely different treatments.
Misinterpreting one for the other doesn’t just delay relief — it can lead to worsening complications, including infections, ureter blockages, and even kidney damage. For women, the risk of misdiagnosis is higher due to several factors. Female anatomy can make it harder to pinpoint the exact source of pain, and since UTIs are more common in women, there’s a tendency to assume that any urinary symptom must be an infection.
In this article, we’ll break down why this misdiagnosis happens so often, what key signs separate kidney stones from UTIs, and how women can advocate for better testing and faster, more accurate treatment. If you’ve ever been told it’s “just a UTI” but something felt off, this might be the clarity you’ve been looking for.
Why Women’s Kidney Stones are Often Missed
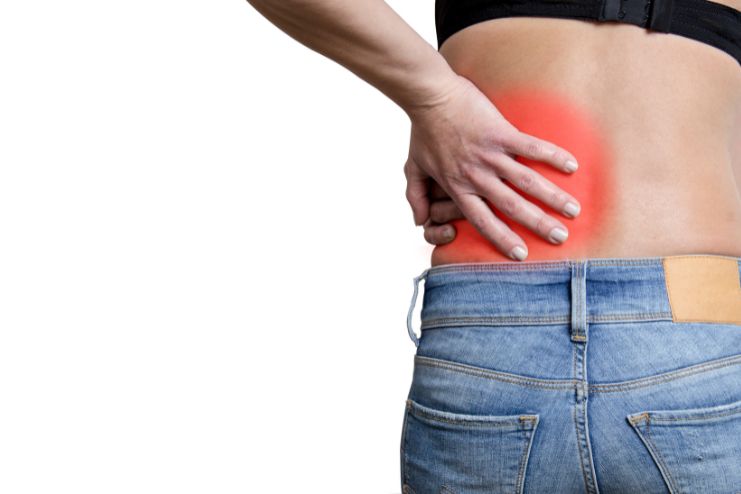
Kidney stones are often thought of as a male-dominated condition, but women experience them too, and often go undiagnosed. Despite presenting with intense symptoms, many women are misdiagnosed with UTIs because the signs overlap. Compounding the issue are diagnostic shortcuts, gender-based assumptions, and the complex nature of female anatomy.
These factors contribute to delayed treatment and unnecessary suffering. Understanding why this happens is the first step to preventing it.
Symptom Overlap
UTIs and kidney stones can feel similar at first, which is why doctors often default to diagnosing a UTI. But several key differences, especially the nature and location of the pain, are often missed during initial assessments. Recognizing these differences early can prevent misdiagnosis.
- Both conditions may involve urinary urgency, burning, and pelvic pain.
- Kidney stone pain tends to be sharp, severe, and radiates to the back or groin.
- Stones often cause flank pain and cramping that comes in waves.
- Blood in the urine without signs of infection suggests a stone, not a UTI.
- UTIs usually don’t involve nausea, vomiting, or severe one-sided pain.
Gender Bias in Pain Assessment
Women’s pain is often underestimated or misattributed — a problem well-documented in medical literature. This bias leads to under-treatment, especially in emergency rooms where quick assumptions are made. Women are more likely to be told their symptoms are “normal” or emotional.
- Studies show women receive less aggressive pain treatment than men.
- Women’s urinary symptoms may be dismissed or labeled as anxiety-related.
- Severe kidney stone pain may be written off as “just a bad UTI”.
- Pain complaints during menstruation or menopause are often overlooked.
- Quick prescriptions for antibiotics often replace proper diagnostic tests.
Anatomical Considerations
Female anatomy makes diagnosis more challenging, especially when pain radiates to the pelvis. Kidney pain may mimic gynecological issues like ovarian cysts or menstrual cramps, leading to delays. Without imaging, doctors may never suspect a kidney stone.
- Pain from the kidneys can feel like it’s coming from the uterus or bladder.
- Reproductive health conditions may mask or mimic stone symptoms.
- Patients are often referred to gynecologists instead of urologists.
- Pelvic pain is frequently generalized, missing kidney-specific evaluation.
- Symptoms may be dismissed as hormonal or cycle-related without proper testing.
UTI vs. Kidney Stone: Key Symptom Differences

Urinary tract infections and kidney stones can look similar on the surface, but they’re very different conditions with different treatments. Many women are given antibiotics for what seems like a UTI, only to find out later that a kidney stone was the actual cause.
That’s why it’s essential to understand how the symptoms differ. Even a small change in how the pain feels or where it shows up can be a major clue. Paying attention to these differences helps ensure faster, more accurate care.
UTIs
UTIs are infections in the bladder or urethra, and they tend to cause irritation rather than sharp pain. Most symptoms stay focused in the lower abdomen or pelvic region. They usually improve with antibiotics and hydration.
- Burning sensation during urination.
- Frequent urge to urinate, even after emptying the bladder.
- Cloudy or foul-smelling urine.
- Lower abdominal or pelvic discomfort.
- Mild pressure around the bladder area.
Kidney Stones
Kidney stones cause pain that is much more intense and often shifts from the back to the groin. Unlike UTIs, the pain can be sharp, stabbing, and unpredictable. Stones may also trigger nausea and visible blood in the urine without any infection.
- Severe pain in the lower back or side (flank pain).
- Pain that radiates to the lower abdomen or groin.
- Blood in urine without signs of infection.
- Nausea and vomiting, especially during pain episodes.
- Pain that comes in waves and doesn’t stay in one place.
The UC Davis Health Department of Urologic Surgery notes that kidney stones can cause “dull lower back pain that comes and goes, or sharp pain that moves to your abdomen or groin,” whereas UTIs often result in discomfort in the lower abdomen.
Signs Your “UTI” Might Be a Kidney Stone
Sometimes what feels like a stubborn UTI may actually be a kidney stone causing the trouble. If your symptoms don’t improve with antibiotics or if certain warning signs appear, it’s important to consider a different diagnosis. Recognizing these signs early can help you get the right treatment without unnecessary delays.
- Symptoms persist even after completing a full course of antibiotics.
- Urine cultures come back negative, showing no bacterial infection.
- Pain is severe, located on one side, and comes in waves rather than constant burning.
- Blood appears in urine without the usual infection signs, like fever or cloudy urine.
- You experience repeated episodes of urinary discomfort and pain that keep returning.
A matched-cohort study over a 19-year period indicated that individuals with kidney stones had a significantly higher risk of developing UTIs compared to those without stones. The hazard ratio was 5.67, emphasizing a strong association between kidney stones and subsequent UTIs.
How Kidney Stones Form and Who’s at Risk

Kidney stones develop when certain substances in the urine become highly concentrated and crystallize, forming solid masses inside the kidneys or urinary tract. Various factors increase the likelihood of stone formation, including lifestyle habits, diet, genetics, and specific health conditions.
While kidney stones can affect anyone, women have some unique risk factors that contribute to their chances of developing stones. Understanding these causes and risks can help in prevention and early detection.
Causes
Several common factors can trigger kidney stone formation by increasing the concentration of stone-forming substances in the urine or reducing fluid levels:
- Dehydration: Not drinking enough water leads to concentrated urine, which increases the chance of crystals forming.
- High intake of oxalate-rich foods: Foods like spinach, nuts, and chocolate contain oxalates that can combine with calcium to form stones.
- Family history of kidney stones: Genetics plays a strong role; if close relatives have stones, your risk is higher.
- Chronic urinary tract infections: Persistent infections can change urine composition and promote stone formation, especially struvite stones.
Women-Specific Risks
Women face some additional risks related to their biology and life stages that can contribute to kidney stone development:
- Postmenopausal hormonal changes: Decreased estrogen levels can affect calcium metabolism, increasing stone risk.
- Pregnancy-related urinary stasis: During pregnancy, slowed urine flow can allow crystals to form more easily.
- Recurrent UTIs: Repeated infections can damage the urinary tract and create an environment where stones are more likely to form.
Types of Stones
Kidney stones vary by composition, and each type may require different treatment and prevention strategies:
- Calcium oxalate stones: The most common type, formed when calcium binds with oxalate in urine.
- Uric acid stones: Occur when urine is too acidic, often related to diet or metabolic conditions.
- Struvite stones: Typically linked to infections, these stones can grow quickly and become large if untreated.
Read More: Kidney Stones: Types, Causes, Symptoms, and Diet
Diagnostic Tools That Help Distinguish Stones from UTIs
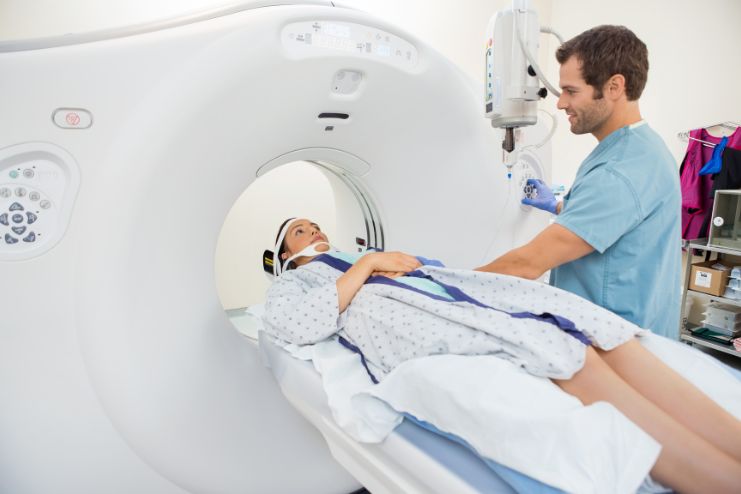
Accurate diagnosis is essential for effective treatment, especially since kidney stones and UTIs share many symptoms. Healthcare providers rely on several diagnostic tools to tell these conditions apart and determine the best course of action. Understanding these tests can empower patients to advocate for the right evaluations when symptoms persist or don’t respond to initial treatments.
Urinalysis
- A simple, non-invasive urine test that checks for the presence of blood, crystals, and bacteria.
- Detecting blood (hematuria) without bacteria can indicate kidney stones rather than infection.
- Identifies signs of infection, such as white blood cells and bacteria, which point toward a UTI.
Non-contrast CT Scan
- This is considered the gold standard imaging test for kidney stones due to its high accuracy (over 95%).
- Provides detailed images of the urinary tract, helping to locate the size, number, and position of stones.
- Quick and widely available, making it the preferred choice in emergency settings.
- Does not require contrast dye, reducing the risk of allergic reactions or kidney strain.
Ultrasound
- A radiation-free imaging option is often used for pregnant women or patients who need to avoid CT scans.
- It can detect larger stones and signs of urinary tract obstruction, but is less sensitive for small stones.
- Useful for monitoring stone movement or assessing complications without exposing patients to radiation.
Blood Tests
- Assess kidney function by measuring markers such as creatinine and blood urea nitrogen (BUN).
- Help detect systemic infection or inflammation that could indicate a complicated UTI or kidney involvement.
- Can identify electrolyte imbalances caused by kidney stones or dehydration.
Why Timely Diagnosis Matters
Prompt and accurate diagnosis of kidney stones is crucial to prevent serious health complications and reduce patient suffering. When kidney stones are mistaken for UTIs or other conditions, delays in proper treatment can allow the problem to worsen. Early intervention not only improves outcomes but also helps avoid unnecessary costs and emotional stress.
- Urinary obstruction: Untreated stones can block urine flow, causing intense pain and potentially damaging the kidneys.
- Kidney infections (pyelonephritis): Blockages increase the risk of infections that can spread to the kidney, requiring urgent medical care.
- Chronic kidney disease: Repeated or prolonged obstruction and infections can impair kidney function over time.
- Increased healthcare costs and patient distress: Misdiagnosis often leads to multiple doctor visits, unnecessary treatments, and emotional strain from ongoing symptoms.
Treatment Options: Stones vs. UTIs
Treating kidney stones and urinary tract infections requires very different approaches, even though their symptoms can overlap. While UTIs typically respond well to antibiotics and hydration, kidney stones often need more targeted pain management and sometimes surgical intervention. Understanding these differences can help patients seek the right care and avoid complications.
UTIs
- Antibiotic therapy: The primary treatment to eliminate the bacterial infection causing the UTI. The specific antibiotic depends on the bacteria identified and resistance patterns.
- Increased fluid intake: Drinking plenty of water helps flush bacteria from the urinary tract and supports healing.
- Pain management: Over-the-counter pain relievers such as acetaminophen or ibuprofen can ease discomfort during infection.
Kidney Stones
- Pain management and hydration for small stones: Many small stones pass naturally with adequate pain control and increased fluids to promote stone passage.
- Extracorporeal shock wave lithotripsy (ESWL): A non-invasive procedure that uses sound waves to break larger stones into smaller pieces that can be passed more easily.
- Ureteroscopy or surgical removal: For large or obstructive stones, a ureteroscope can be used to remove or break stones; surgery may be required in complex cases.
- Preventive measures: Includes dietary changes like reducing oxalate-rich foods, maintaining hydration, and sometimes medications to prevent new stone formation.
When to Advocate for Further Testing
If symptoms don’t improve or worsen despite treatment, it’s important to speak up and ask your healthcare provider about further diagnostic options.
- Persistent symptoms despite treatment: If your urinary symptoms don’t get better after a full course of antibiotics or other therapies, further testing is needed.
- Severe or radiating back pain: Intense pain that spreads from the back to the groin or abdomen may indicate kidney stones or other serious conditions.
- Visible blood in urine: Blood that you can see clearly in your urine, especially without other infection signs, warrants additional investigation.
- Nausea, vomiting, or fever with urinary symptoms: These signs may signal infection or complications related to kidney stones and require urgent evaluation.
Patients should feel empowered to discuss imaging options, such as ultrasound or CT scans, with their doctors to ensure an accurate diagnosis and appropriate treatment plan.
Conclusion
Kidney stones in women are frequently misdiagnosed as urinary tract infections due to the similarity in symptoms and the complexities of female anatomy. Understanding the key differences between kidney stones and UTIs is essential for both patients and healthcare providers to ensure timely and accurate diagnosis.
Diagnostic tools such as urinalysis, ultrasound, and CT scans play a vital role in distinguishing kidney stones from infections, guiding the appropriate course of action. Early detection and intervention can prevent serious consequences such as urinary obstruction, kidney infections, or long-term kidney damage.
With greater awareness and timely care, kidney stones in women can be identified quickly, treated successfully, and prevented in the future, leading to better health outcomes and peace of mind.
References
- https://melbourneurologycentre.com.au/kidney-stone-symptoms-female-patients/
- https://www.urologyhealth.org/urology-a-z/k/kidney-stones
- https://timesofindia.indiatimes.com/life-style/health-fitness/health-news/reasons-why-more-women-are-falling-prey-to-kidney-problems-post-30s/photostory/100571876.cms
- https://dcurology.net/2021/06/15/differentiating-kidney-stones-from-a-urinary-tract-infection/
- https://www.advancedurology.net/blog/do-i-have-kidney-stones-or-a-uti-how-to-tell-the-difference
- https://nortonhealthcare.com/news/uti-or-kidney-stone/
- https://www.mayoclinic.org/diseases-conditions/kidney-stones/symptoms-causes/syc-20355755
- https://my.clevelandclinic.org/health/diseases/15604-kidney-stones
- https://www.mykidneystone.com/en-US/basics/causes-risk-factors.html
- https://www.urologyhealth.org/urology-a-z/k/kidney-stones
- https://panoramichealth.com/blog/the-link-between-urinary-tract-infection-and-kidney-stones/
In this Article















