This question comes up in real life more than people admit. Not in dramatic situations. Just normal ones: “It’s just one beer.” “I feel fine already.” “The antibiotic is mild.” “My friend drank on it, and nothing happened.”
The truth is, alcohol with antibiotics is never always a strict “NO,” but it is also not harmless either. The problem here is that many online answers are too simple: either they just scare you too much, or they dismiss it too casually.
A more honest way to look at it is this: Alcohol does not always create a dangerous chemical reaction. But it often creates a recovery failure.
So the real question becomes: Do you want your infection gone fast, or do you want a drink in the middle of treatment?
Let’s break this down properly, without generic advice.
The “Danger Zone”: Antibiotics You Must Never Mix with Alcohol
Some antibiotics are not just “mildly affected” by alcohol. They can cause serious reactions even with small amounts. These are the ones where alcohol is a hard NO.
1. Metronidazole (Flagyl)
Used for dental infections, gut infections, bacterial vaginosis, and parasites. Mixing alcohol can trigger a reaction called a “disulfiram-like reaction,” which may cause the following:
- Severe vomiting
- Flushing
- Pounding headache
- Fast heartbeat
- Breathlessness
Even mouthwash containing alcohol can sometimes worsen symptoms. Wait at least 48–72 hours after finishing.
As family physician Dr. Jasmine Vayalil points out, “Certain medications like cough syrups, laxatives, and mouthwashes can contain a notable amount of alcohol – not just alcoholic beverages. If experiencing any adverse side effects while on antibiotics, check to make sure one of those is not the culprit.”
2. Tinidazole
Similar to metronidazole, which is often given for amoebiasis and giardiasis. Same alcohol reaction risk. Avoid alcohol during treatment and for 3 days after.
3. Linezolid
This one is less talked about.
Linezolid can interact with alcohol indirectly because it affects certain brain chemicals. Some alcoholic drinks (especially tap beer and wine) contain tyramine (a food chemical), which can raise blood pressure dangerously.
Not common, but definitely risky enough to avoid.
4. Certain Cephalosporins (like Cefotetan)
Not every cephalosporin, but some specific ones, can cause the following:
- Nausea
- Flushing
- Low blood pressure
- Rapid heartbeat
Doctors usually warn clearly if you are on one of these.
5. Isoniazid and Griseofulvin: Liver Toxicity Risk
Some antibiotics already carry a risk of drug-induced liver injury (DILI). Alcohol adds an extra load.
Isoniazid (used for TB) is especially known for hepatic stress. Mixing ethanol here is not about nausea; it’s about liver inflammation.
Your liver is doing all the metabolism work. Combining both is like running two heavy machines on one small generator.
As family physician Dr. Jasmine Vayalil explains, “In general, alcohol can cause liver damage when there is too much for the liver to break down and toxins build up. This is exacerbated when the liver doesn’t work as well (i.e., in people with liver disease) or when the liver is trying to process other medications/toxins simultaneously (i.e., in the case of older people who often require multiple medications).”
Therefore alcohol becomes riskier with antibiotics that already stress the liver.
Common Antibiotics and Alcohol (The “Caution” Tier)
Now comes the confusing part. Many antibiotics do not have a direct toxic interaction with alcohol. But that doesn’t mean it is “safe.”
As consultant clinical pharmacist Dr. Geraldine Moses explains, “Certainly, there are many medications that do have alcohol warnings. But with most antibiotics, frankly, it’s not a big deal.”
The key phrase there is most. The issue is rarely a dramatic chemical reaction. The issue is recovery efficiency.
It means the risk is indirect: recovery slows, side effects intensify, and your body struggles.
1. Amoxicillin
Alcohol does not cancel it. But alcohol increases stomach upset, dizziness, and dehydration.
If infection is mild, one drink may not cause disaster, but it is still an unnecessary strain.
2. Azithromycin
No major chemical reaction, but alcohol can worsen nausea, fatigue, and liver load (liver strain).
Azithromycin already stays long in the body, so mixing is not smart.
3. Doxycycline
Alcohol can reduce effectiveness if drinking is heavy or frequent. Also increases the risk of acid reflux, stomach irritation, and even sunburn.
4. Ciprofloxacin/Levofloxacin
Alcohol increases dizziness and confusion. Also, both can affect tendons and nerves in rare cases, and alcohol adds more stress to the nervous system.
5. Nitrofurantoin (Antibiotic for Urinary Tract Infection – UTI)
Alcohol may worsen nausea, headache, and liver irritation. UTIs already need hydration; alcohol does the opposite.
3 Ways Alcohol Sabotages Your Recovery

First, what do antibiotics do? Public health pharmacist Dr. Megan Freeland explains, “Antibiotics work in two ways. They either kill bacteria or they stop bacteria from growing…”
Now, this is the part most blogs miss. The issue is not always “interaction.” The issue is interference.
1. Alcohol Confuses Your Body’s Priorities
When you drink, the liver focuses on clearing alcohol first. So your body is basically doing the following:
- Detox work
- Immune work
- Antibiotic metabolism (drug processing)
altogether. That slows recovery. Not dangerous always, but inefficient.
2. Alcohol Makes Side Effects Feel Worse
Many antibiotics already cause nausea, loose stools, fatigue, and headache. Alcohol adds the same symptoms.
So patients often think, “This antibiotic is too strong.” But actually, it is the combination.
3. Alcohol Weakens Immune Response Quietly
Alcohol reduces certain immune cell activity for hours. So even if an antibiotic is killing bacteria, your immune system support becomes weaker.
That means infection lingers, relapse chances increase, and recovery feels slower. This is why doctors say, “Don’t drink during illness, not just during antibiotics.”
Read More: Top 8 Antibiotic Creams for Hidradenitis Suppurativa (Dermatologist-Approved)
The “Wait Time” Cheat Sheet (Resumption Timeline)
People always ask: “How long after antibiotics can I drink?” Here is the practical answer.
1. High-risk antibiotics
- Metronidazole: wait for 3 days after last dose
- Tinidazole: wait for 3 days
- Cefotetan: wait for 3 days
- Linezolid: avoid unless doctor approves
2. Common antibiotics
- Amoxicillin: wait for 24 hours after last dose
- Azithromycin: wait for 48 hours (stays longer in body)
- Doxycycline: wait for 24–48 hours
- Ciprofloxacin: wait for 48 hours
3. Simple rule
If infection symptoms are still present, don’t drink even if the course is finished. Alcohol after antibiotics is less about the medicine and more about your recovery stage.
In most cases, delaying antibiotics just to drink is never recommended. As family medicine physician Dr. Colleen Clayton explains, patients should usually choose nonalcoholic options instead of postponing treatment.
However, not every infection carries the same urgency. “Something like bacterial vaginosis, which I commonly treat with metronidazole, is never urgent,” she notes. “If symptoms aren’t too bothersome, then I may tell patients they can start their antibiotic after the weekend.”
Read More: The Hidden Dangers of Overusing Antibiotics: What You Need to Know
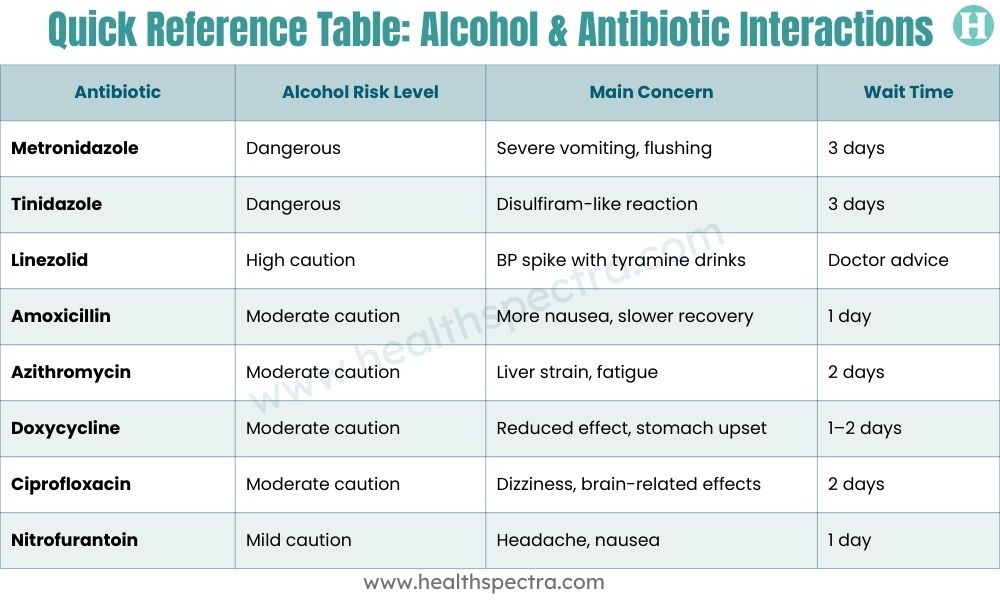
Quick Reference Table: Alcohol and Antibiotic Interactions
Final Thoughts
The internet treats this topic too dramatically or too casually. Reality is simple: Some antibiotics with alcohol mean real danger. Most antibiotics with alcohol mean unnecessary recovery delays.
Your body heals better without alcohol during an infection
So the smarter question is not: “Will I die if I drink?” It is, “Why make your treatment slower for one drink?”
Antibiotics are already a short-term medicine. Alcohol can wait.
Read More: Why You Shouldn’t Use Leftover Antibiotics — Even If You Feel Sick Again
- The biggest risk is not always interaction between alcohol and antibiotics, but recovery slowing down quietly.
- Metronidazole and tinidazole are true “never mix” antibiotics.
- Alcohol can reduce antibiotic success indirectly by weakening the immune response and sleep repair.
- Even common antibiotics become less effective when the body is dehydrated or immune-suppressed.
- Most studies focus on chemical reactions, but less research exists on how small alcohol amounts affect immune recovery speed during antibiotic therapy.
FAQs
1. Can I drink one beer while on antibiotics?
Depends on the antibiotic. With metronidazole, absolutely no. With amoxicillin, it may not be dangerous, but it still delays recovery.
2. Does alcohol cancel antibiotics?
Not directly, but it can reduce effectiveness indirectly by weakening immunity and worsening side effects.
3. How long after finishing antibiotics can I drink?
Usually 24–48 hours, but for metronidazole/tinidazole, wait 3 days.
4. What happens if I accidentally drink alcohol?
Most likely experience nausea or dizziness. If on metronidazole and symptoms are severe, seek medical help.
5. Is wine safer than hard liquor with antibiotics?
No. The problem is alcohol itself, not the type. Some wines also contain tyramine, which is risky with linezolid.
In this Article