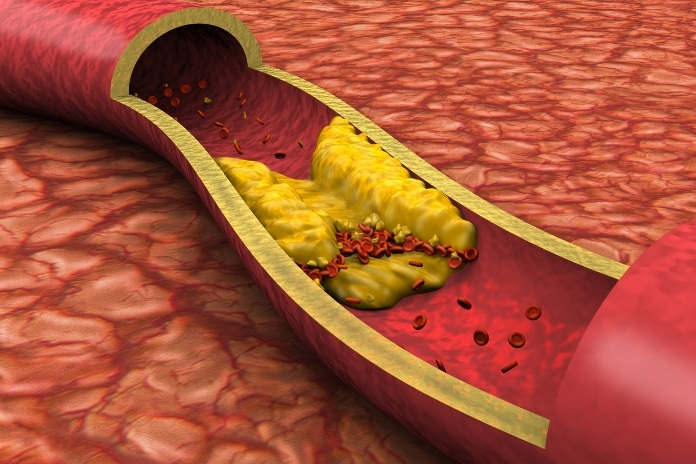
It may seem strange: you eat well, you exercise, you have a healthy weight. However, you have high cholesterol, as per your blood work reports. Many people believe that high cholesterol immediately means illness. The reality, however, is that cholesterol isn’t necessarily bad. Your body needs it to make hormones, vitamin D, and healthy cell membranes.
It’s not the total amount of cholesterol in your body that matters most, but the size of its particles, your level of inflammation, and how it interacts with your arteries. High cholesterol in healthy individuals is not rare, and it makes us think: when is a statin enough, and when might additional support be needed?
In this article, we’ll understand why cholesterol levels alone don’t always tell the full story, when statins may fall short, and how lifestyle changes and tests at the right time can reveal your actual heart-health.
Understanding Cholesterol: The Good, the Bad, and the Misunderstood

Before going deeper, we must understand the different types of cholesterol and why one number on a blood test can be misleading.
- LDL (Low-Density Lipoprotein): At times called “bad” cholesterol because excess LDL can build up in the walls of arteries and form plaque.
- HDL (High-Density Lipoprotein): “Good” cholesterol that removes LDL from the bloodstream and routes it to the liver.
- Triglycerides: Fat that adds to heart risk when raised, especially with insulin resistance.
- Total Cholesterol: Gives a general impression but does not tell the entire story. The amount of LDL and HDL, the size and density of LDL particles, and not just the ratio of LDL to HDL, are more significant.
Cholesterol, genetics, and lifestyle all contribute to how cholesterol affects heart health. Even with a higher LDL level, low inflammation, optimal HDL function, and healthy metabolism can change the game in your favor.
Read More: Cholesterol Myths vs. Facts: Debunking Common Misconceptions
When High Cholesterol Doesn’t Equal High Risk
You may be able to have elevated cholesterol and still be relatively low-risk if other protective forces are in your corner.
1. Low HDL Levels
An adequate level of HDL is what gets rid of LDL in your body and can prevent some of the risks from higher LDL. But very high levels of HDL aren’t always a good sign. The most important thing is that HDL is functioning well.
2. Low Inflammation and Stable Blood Sugar
Inflammation is among the largest factors that lead to bad cholesterol. If LDL particles get oxidized and cause inflammation, they tend to harm arteries. If your diet, exercise, and blood sugar management keep inflammation low, your overall heart risk decreases despite having relatively high cholesterol.
3. Good Arterial Health
The best thing to do to ascertain your actual risk is to get your arteries tested. Calcium scoring or carotid scanning will show whether plaque has formed. People with “high cholesterol” occasionally have arteries that are clean as a whistle, showing that numbers aren’t everything for your health.
When Statins Won’t Work
Statins are effective drugs for lowering LDL cholesterol, but they don’t address every cause of heart disease. Drug therapy might not be enough in some cases.
1. Statins Lower LDL but Can’t Reverse Lifestyle Risks
Statins reduce cholesterol production by the liver, but they can’t reverse inflammation, insulin resistance, or dietary defects. They do work, however, but best as part of sustained lifestyle modifications.
2. Elevated Lipoprotein(a) [Lp(a)]
Lp(a) is a genetic risk factor that raises heart-disease risk and isn’t lowered by statins. People with high Lp(a) may be healthy but at increased cardiovascular risk. New therapies are ongoing to examine this fact. Therefore this makes it one of the conditions where statins alone don’t work.
3. Continual Inflammation
Even if your cholesterol is normal, high C-reactive protein (CRP) is a sign that inflammation has not reduced. This type of chronic inflammation can damage blood vessels and increase heart disease. Careful attention to an anti-inflammatory diet, stress reduction, and better sleep can be helpful.
4. Statin Resistance or Side Effects
Others don’t respond to statins fully, or they develop side effects like muscle weakness or pain. In those cases, doctors can attempt other treatments like ezetimibe, PCSK9 inhibitors, or bempedoic acid to improve outcomes.
“We know that if you have heart disease, specifically atherosclerosis, statins, if tolerated, are an absolute must,” says Brian Cambi, MD, a Yale Medicine cardiologist. “As far as who should take statins for prevention, that continues to get refined.”
Read More: 10 Proven Ways to Boost Your HDL Cholesterol Without Medication
What Else Can You Do to Support Heart Health
Apart from medications, long-term protection of the heart occurs by improving how your body handles cholesterol and inflammation.
1. Eat an Anti-Inflammatory Diet

- Follow a Mediterranean-type diet with olive oil, nuts, fatty fish, whole grains, fruits, and vegetables.
- Avoid processed foods, sugar, and refined carbohydrates.
- Take fiber-containing foods and plant nutrients that help your body get rid of cholesterol naturally.
2. Exercise for Arterial Flexibility
Here are a few tips/exercise regimens you can follow to promote arterial flexibility:
- Do at least 150 minutes of moderate aerobic exercise each week.
- Include resistance training two to three times a week to maximize insulin sensitivity.
- Aim for daily physical activity, and not just exercise, which promotes circulation and decreases inflammation.
3. Regulate Stress and Sleep
Cortisol increases with chronic stress, leading to higher LDL and triglycerides. Relax with techniques of relaxation, mindfulness, and quality sleep to keep lipid metabolism in check and inflammation minimal.
4. Checkups and Blood Tests
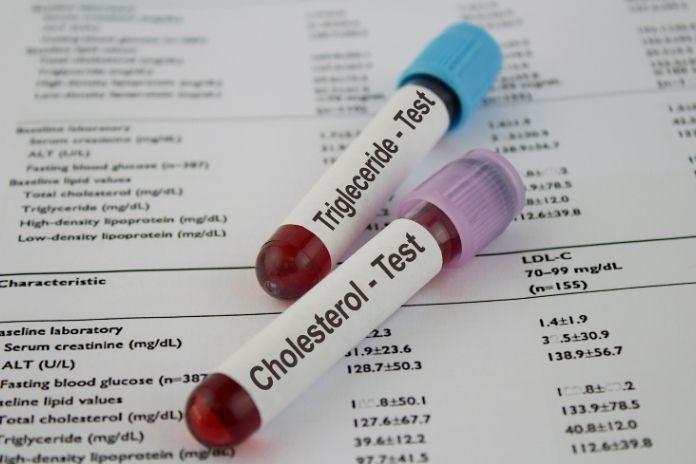
- You can ask your doctor for testing, like LDL particle size and hs-CRP, to measure real risk.
- If you have a history of heart disease in your family, request testing for Lp(a).
- If you are taking statins, monitor liver and muscle function periodically.
Read More: Food Swaps to Manage High Cholesterol Without Sacrificing Taste
When to Talk to Your Doctor

A few signs signal an immediate visit to a medical practitioner. Seek a doctor’s advice if:
- Your cholesterol stays high despite a healthy lifestyle.
- You have a family history of early heart disease.
- You experience statin side effects or reduced response.
- You’re unsure if medication is still necessary.
A healthcare provider can personalize your plan with deeper testing or adjusted treatment options.
Key Takeaway
High cholesterol does not automatically translate to bad health, but it is a sign that requires attention. Statins are helpful, but they work best as part of an overall healthy lifestyle, moderation of inflammation, and regular monitoring. The goal isn’t just to lower cholesterol numbers; it’s to maintain your arteries in good health and your overall cardiovascular function in top condition.
So, when you see high cholesterol in your reports the next time, do not panic immediately. Instead, sit back and assess all other factors. Book an appointment with your doctor to know if there is a need to worry. Most of the time, when other factors are normal, high cholesterol is not a problem!
FAQs About High Cholesterol and Statins
Q: Can you be healthy with high cholesterol?
Yes. Most individuals with higher cholesterol have low inflammation, high HDL, and good arteries. The secret is to understand why the cholesterol is elevated and know whether it’s bad.
Q: What lab tests identify real heart risk beyond cholesterol?
Advanced lipid testing, hs-CRP, and imaging such as coronary calcium scoring, will highlight silent risks not identified by routine panels.
Q: Do statins reduce heart attack risk for all?
They lower the risk significantly for most, but the response is individually dependent on things like genetics, inflammation, and atherosclerotic artery health.
Q: How do you decrease inflammation naturally?
A whole food diet, exercise, stress reduction, good sleep, and proper weight all play a part.
Q: Can you ever quit statins safely?
Under a doctor’s supervision only. Lifestyle and high-tech testing can allow for fine-tuning in a minority of low-risk individuals, but your doctor will have to decide on this.
References
- https://www.healthhub.sg/well-being-and-lifestyle/exercise-and-fitness/150minutes
- https://www.heart.org/en/health-topics/cholesterol/hdl-good-ldl-bad-cholesterol-and-triglycerides
- https://www.kauveryhospitalsbangalore.com/blog/c-reactive-protein-test
- https://www.ncbi.nlm.nih.gov/books/NBK395573/
- https://www.ucsfhealth.org/education/diagnosing-heart-disease
- https://www.keckmedicine.org/blog/what-is-the-difference-between-good-and-bad-cholesterol/
In this Article