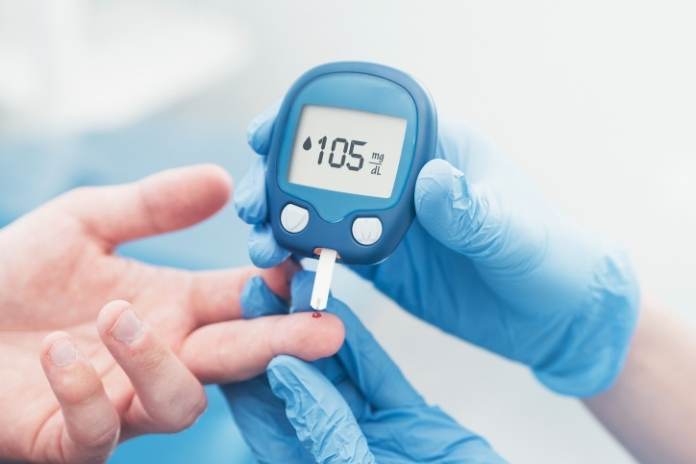
Prediabetes is more than just driving blood sugar higher; it sneakily increases stiffness in arteries, promotes inflammation, and contributes to cardiovascular disease years before diabetes appears on the lab result. The glimmer of hope that making lifestyle changes can turn around prediabetes can help lower blood pressure, cholesterol, inflammation, and insulin resistance, thereby reducing cardiovascular risk.
Prediabetes is an extremely common condition that affects hundreds of millions of adults around the world. Prediabetes usually passes unnoticed until another condition, such as high blood pressure or high cholesterol, is identified.
Before type 2 diabetes appears, elevated blood sugar levels and insulin resistance can already damage blood vessels and the heart. During this “silent” period, it is an opportune time to make changes to blood sugar to either halt or delay the onset of major cardiovascular disease.
What Is Prediabetes? (Quick Medical Overview)
Prediabetes can only be diagnosed by using typical glucose levels that are sandwiched between normal and diabetic thresholds.
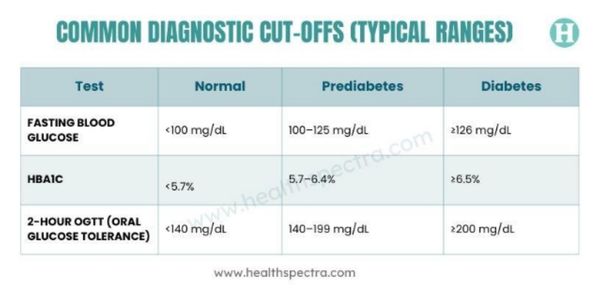 A difference exists between prediabetes and type 2 diabetes in that, while blood sugar levels are increased, they have not yet reached the levels considered diagnostic for diabetes, and it may be possible to prevent late complications.
A difference exists between prediabetes and type 2 diabetes in that, while blood sugar levels are increased, they have not yet reached the levels considered diagnostic for diabetes, and it may be possible to prevent late complications.
In fact, a large number of individuals who experience prediabetes do not have any apparent symptoms, as fatigue, frequent urination, or thirst typically occur once the individual has developed diabetic conditions.
Read More: Heart Disease Causes And Effects Due To Common Habits
How Prediabetes Raises Heart Disease Risk
Prediabetes is at the focal point of what is called metabolic syndrome, in which there are patterns of insulin resistance, hypertension, dyslipidemia, and increased abdominal obesity that significantly increase the risk of heart problems.
Prediabetes and Cardiovascular Disease: Key Mechanisms
- Insulin Resistance and Atherosclerosis: In this condition, cells resist the effects of insulin. Consequently, the pancreas produces more insulin, leading to elevated blood glucose and lipids that stick to the arterial walls, accelerating atherosclerosis.
- Persistent Inflammation: Blood sugar and fat from visceral fat can trigger an inflammatory response that destabilizes atheromas and leads to thrombus formation.
Effects on major risk factors:
- Blood Pressure: Insulin resistance and sodium retention cause high blood pressure because of additional work by the heart.
- Cholesterol Levels: Patients with prediabetes tend to have low HDL (“good” cholesterol) and high triglycerides, which is a potent predictor for coronary artery disease.
- Endothelial Dysfunction: There is less production of nitric oxide in the inner lining of the blood vessels, called the endothelium. This results in less flexible arteries.
Large cohort studies have shown that those with prediabetes are at a significantly increased risk for CVD, stroke, and death, after adjusting for other risk factors, when compared to those with normal glucose levels.
What “Reversing Prediabetes” Actually Means
Reversal is not a magic cure; it is a Risk Reduction Strategy.
In fact, turning around prediabetes typically involves:
- Normalization of blood sugar levels(fasting glucose, HbA1c, or OGTT).
- These progressions are being sustained over time, preferably with fewer or without other drugs.
Important Clarifications:
- Reversal does notconfer lifelong protection, so if lifestyle veers off track, or overweight, inactivity, or poor eating habits re-emerge, prediabetes and heart disease risk may redevelop.
- The primary objective is to reduce the risk of progression to type 2 diabetes, thereby reducing damage to the heart and blood vessels.
Evidence: How Reversing Prediabetes Affects Heart Health
Large lifestyle intervention studies provide solid support for early interventions in people with prediabetes.
The Diabetes Prevention Program demonstrated that an intensive lifestyle intervention (healthy diet, 150 minutes per week of physical activity, and 7% weight loss) reduced the risk of developing type 2 diabetes from prediabetes by 58% over 3 years.
Follow-up trials revealed that subjects in the lifestyle intervention had favorable blood pressure, triglyceride, and cholesterol values, often requiring fewer medications than those in the control groups.
Approximately two decades of follow-up, in which postponing or preventing diabetes resulted in a decreased prevalence of microvascular events (involving the eyes, kidneys, and nerves) among those who did not develop diabetes.
Although the primary outcomes did not demonstrate a substantial reduction in major cardiovascular events, individuals who did not develop diabetes had significantly lower rates of vascular events than those who did.
In short, the reversal of prediabetes and the prevention of developing diabetes can enhance a number of cardiovascular risk factors and minimize the vascular injury that precedes heart disease.
Lifestyle Changes That Improve Blood Sugar and Heart Health
Nutrition Patterns
A healthy diet is an important part of the strategy. Patterns of eating are far more valuable than perfection. To focus, therefore, consider:
- High-fiber diets: Vegetables, fruits, beans, nuts, and seeds help to slow the absorption of glucose, increase the body’s sensitivity to insulin, and optimize blood cholesterol levels.
- Whole grains over refined grains: For example, replacing white rice, maida, and sweetened cereals with oats, brown rice, millets, and whole wheat can work wonders in lowering both HbA1c and fasting glucose.
- Lean protein, such as lentils, beans, fish, eggs, and lean poultry, will help keep you full, maintain weight, and prevent a rise in blood sugar levels.
- Healthy fats: Replacing saturated and trans fats with avocados or avocado oil, and eliminating or reducing intake of saturated and trans fats, are beneficial for lowering cardiovascular disease risk by reducing C-reactive protein levels and improving lipid profiles.
A normal blood sugar level prevents recurrent endothelial injury and consequently limits the process of developing an atherosclerotic state.
Physical Activity
One of the best ways to overcome insulin resistance symptoms is by exercising on a regular basis.
- Physical activities, such as cycling, brisk walking, and swimming, for 150-300 minutes per week, can increase fasting glucose, blood pressure, and triglycerides.
- Resistance exercise (2 to 3 times a week) increases muscle mass, and muscle, which is a substantial sink for glucose, increasing insulin sensitivity and reducing HbA1c.
A priority in this regard would be consistency, not intensity, such that even taking occasional walks can greatly improve metabolic health.
Weight Loss (If Needed)
For individuals who are obese or overweight, some pounds can be incredibly beneficial. A loss of 5-7% of body weight can help in improving insulin resistance and normalizing diabetes. Visceral or central obesity is more harmful, and slimming down the waistline helps more for inflammation, blood pressure, and cholesterol levels than overall weight loss.
Crash diets, or very quick weight loss, are not encouraged. Rather, incremental changes will help sustain muscles and boost metabolism.
Read More: How Many Carbs Should a Diabetic Have Per Day? What Experts Recommend
Other Key Risk Factors to Address
Prediabetes-related cardiovascular risk factors are complex, and just managing hyperglycemia is not sufficient.
Important areas for management:
- Blood pressure: Maintaining it around or below 120/80 mmHg will not stress already Insulin Resistance-stressed arteries.
- Cholesterol: Reducing LDL and increasing HDL through lifestyle modification and, when necessary, medications helps to stabilize or halt the progression of the atherosclerotic plaques.
- Smoking cessation: Smoking further accelerates endothelial dysfunction and inflammation, thereby substantially increasing the risk of heart disease in individuals with glucose metabolism dysfunction.
- Sleeping, stress:Lack of sleep and stress can increase cortisol levels in the body, leading to problems with insulin, blood pressure, and appetite.
Can Medication Play a Role?
The primary approach would still be lifestyle modification; however, pharmacotherapy becomes an alternative if glycemic or cardiovascular risk factors persist. In the DPP, metformin significantly prevented the progression to diabetes by 31% in the intention-to-treat population, especially among the young, obese population, but this was less effective than lifestyle interventions.
Certain glucose-lowering and anti-weight medications (such as some GLP-1 receptor agonist medications) are currently investigated regarding their effectiveness in diabetes prevention and secondary prevention of CVD. Their use in primary prediabetes remains in development.
More accurately, it is useful to consider pharmacotherapy as complementary rather than a substitute for nutrition, exercise, and weight management programs.
Who Benefits Most From Early Prediabetes Reversal
People with prediabetes can all improve their conditions through lifestyle interventions. There are, however, groups of people with higher levels of cardiovascular benefits.
This applies to individuals with:
- Strong family history of heart disease, early heart attacks.
- High blood pressure or already elevated LDL and Triglycerides.
- Increased abdominal obesity or signs of metabolic syndrome, including elevated waist measurement and low HDL cholesterol.
Owing to their greater baseline risk, for every one-point improvement in blood sugar, blood pressure, or cholesterol, there is more absolute protection from the heart.
Read More: Effective Sleeping Patterns Mitigate Risks Of Heart Disease
When Prediabetes Needs Closer Medical Follow-Up

Monitoring aids in identifying any issues early enough to customize treatment. If any of the following situations occur, more intense follow-up:
- HbA1c or fasting blood glucose levels remain high despite strong lifestyle modifications.
- You begin manifesting symptoms that may include shortness of breath when exercising, chest pain, palpitations, or pain in the legs when walking.
- Associated risk factors (smoking, hypertension, high levels of LDL, strong family history) require personalized risk evaluation and possibly evaluation by cardiologists.
Common Myths About Prediabetes and Heart Disease
- “Heart disease only occurs after diabetes.” Well, cardiovascular disease begins in the prediabetic stage because the risk for cardiovascular disease is already increased compared to those with normal glucose levels.
- “A normal blood sugar level is now defined as having ‘zero risk.’” However, once a person has had prediabetes, their risk is never quite ‘zero,’ since long-term ‘behavioral patterns’ and other risks remain significant.
- “Thin people don’t get prediabetes.” Normal-weight persons may also experience insulin resistance and prediabetes if they possess a high genetic propensity or visceral fat.
Read More: How Quality Sleep Supports Diabetes Management: Tips for a Healthier Life
Final Takeaway
Prediabetes is not a benign phase but rather an early alert suggesting that IR, inflammation, and E-D dysfunction are already happening in your arteries. The reversal of prediabetes through lifestyle measures and, if needed, medications can reduce glycemia, major CV risk factors, and substantially decrease risks of type 2 DM and CVD.
Viewing prediabetes as a transition rather than a label will give you the best chance at taking care of your heart in the long run.
References
- Arreola, E. V., et al. (2025). Post-hoc analyses from the Diabetes Prevention Program Outcomes Study (DPPOS): Prediabetes remission and cardiovascular outcomes.
- Perreault, L., et al. (2014). Regression from prediabetes to normal glucose regulation is associated with reduction in cardiovascular risk: Results from the Diabetes Prevention Program Outcomes Study.
- Vistisen, D., et al. (2019). Reversion from prediabetes to normoglycaemia and risk of cardiovascular disease and mortality.
- Liu, X., et al. (2021). Pre-diabetes reversion to normoglycemia and risk of cardiovascular disease.
- Davoodian, N., et al. (2025). Regression from prediabetes to normoglycaemia and the risk of cardiovascular disease.
- Vistisen, D., et al. (2019). Reversion from prediabetes to normoglycaemia and risk of cardiovascular disease and mortality.
- Shimayama, C., et al. (2025). Impact of diabetes remission or progression on the incidence of cardiovascular disease.
- Cao, Z., et al. (2023). Risk of death associated with reversion from prediabetes.
- Gregg, E. W., et al. (2024). Impact of remission from type 2 diabetes on long-term cardiovascular risk.
- An, X., et al. (2024). Early effective intervention can significantly reduce all-cause mortality in prediabetic patients.
- Davoodian, N., et al. (2025). Prediabetes transitions to normoglycaemia or type 2 diabetes.
- Rubio-Almanza, M., et al. (2018). Cardiovascular risk reduction over time in patients with end-stage renal disease.
- Stentz, F. B., et al. (2021). High protein diet leads to prediabetes remission and positive changes in incretins and cardiovascular risk factors.
- Kowall, B., et al. (2021). Reversion from prediabetes to normoglycaemia after weight change.
- Rivera-Martínez, W. A., et al. (2025). Prediabetes reversal factors in CV risk program (2019-2023).
In this Article