Many people mistakenly believe that arthritis only affects older adults. While joint discomfort is indeed common in seniors, it can also impact younger people, sometimes manifesting as early as their twenties and thirties.
Early-onset arthritis often causes pain in the sacroiliac joints, a condition known as sacroiliitis. Regardless of your age, don’t overlook persistent joint pain. It’s time to break the age barrier on joint health because osteoarthritis (OA) isn’t exclusively a senior’s condition.
According to the CDC, young adults can develop OA, the most common form of arthritis. Often referred to as “wear and tear” arthritis or “degenerative joint disease,” OA is caused by the breakdown of joint cartilage, which ultimately affects the underlying bone.
Early arthritis diagnosis can make a significant difference in your quality of life. With proper medical care and lifestyle adjustments, you can slow disease progression, reduce pain, and maintain joint mobility. This article will explain the subtle indicators of early-onset arthritis, why it can start at a younger age, and what steps to take if you’re experiencing joint problems.
Read More: The Ultimate Arthritis Toolkit: 12 Products That Provide Comfort
Understanding Early-Onset Arthritis in Your 30s
Approximately 15% of people over 30 have osteoarthritis, making it the most prevalent type of arthritis and a degenerative disease that affects millions globally.
Arthritis can strike people as young as their twenties and thirties, though there are usually specific causes, such as repetitive joint stress or previous injuries. Dr. Steven DeFroda, an orthopedic surgeon and sports medicine specialist at MU Health Care, explains that by the time you reach your thirties and forties, “there’s often enough cumulative wear and tear on joints that you might start feeling aches and pains.”
While OA is the most common form, several other types can affect young adults:
Rheumatoid Arthritis (RA): This autoimmune and inflammatory condition can strike at any age, though doctors typically diagnose it in people between 30 and 50. When diagnosed before age 30, it’s considered early onset. RA is a chronic autoimmune disease that causes inflammation and joint damage. If left untreated, it can affect multiple joints and lead to deformities.
Osteoarthritis (OA): While typically beginning in the 50s, OA can occur at any age. When it develops earlier, doctors consider it an early onset. Symptoms often appear gradually and may worsen over time. Common early signs include achy joints, weakened muscles around joints, joint instability, and swelling.
Psoriatic Arthritis: This condition typically develops 10 to 20 years after the onset of psoriasis, a skin condition characterized by red, scaly patches. Most commonly affecting people in their 30s and 40s, psoriatic arthritis can occasionally begin earlier. Only a small percentage of people with psoriatic arthritis experience joint pain before developing skin lesions.
Lupus-Related Arthritis: Systemic lupus erythematosus (SLE) is an autoimmune disease that can impact every body system. Arthritis is among the most common symptoms associated with lupus, and its early stages can present similarly to rheumatoid arthritis.
Read More: Stay Active with Arthritis: 6 Low-Impact Exercise Equipment for Joint Health
Key Early Signs of Arthritis to Watch Out For
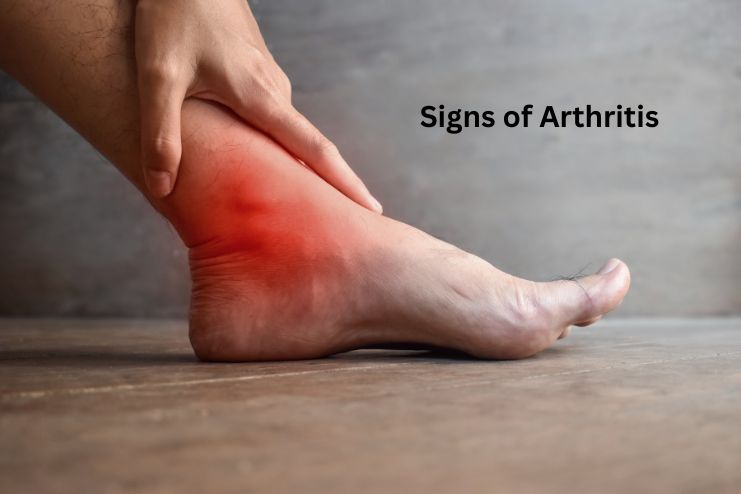
1. Persistent Joint Pain
Persistent joint pain is often one of the earliest and most noticeable indicators of arthritis. Unlike injury-related pain, which tends to be short-term, arthritis-related discomfort is usually long-lasting and can be ongoing or intermittent.
This pain typically worsens over time and occurs more frequently. It can develop even without noticeable swelling and usually affects the same joints repeatedly. If you’re experiencing persistent joint pain, particularly in your hands, knees, or wrists, consult your doctor.
2. Morning Stiffness Lasting More Than 30 Minutes
Extended morning stiffness that lasts more than 30 minutes could be an early sign of arthritis. This stiffness generally occurs after periods of inactivity and can develop gradually over time, typically indicating underlying inflammation in the joint lining.
While stiffness can occur with various types of arthritis, it’s a defining symptom of rheumatoid arthritis. If you experience daily morning stiffness that significantly impacts your routine, it’s worth discussing with a healthcare professional.
3. Swollen or Tender Joints
Joint tenderness or swelling is another early warning sign. Arthritis-related inflammation can cause noticeable swelling in the joint and surrounding area, often accompanied by tenderness to touch. Any swelling that persists for days or recurs frequently over a short period requires medical evaluation.
These symptoms may initially appear mild but can intensify as the condition progresses. Early identification of this pattern is crucial since prompt inflammatory treatment can prevent joint damage and improve long-term mobility.
4. Decreased Range of Motion
A reduced range of motion indicates that arthritis may be affecting joint function. Simple activities involving joint movement, such as tying shoes or reaching for objects, may become challenging. Without prompt intervention through physical therapy and other management techniques, this limitation can worsen and significantly impact daily activities.
5. Fatigue and General Malaise
Fatigue is an important but often overlooked early indicator of several forms of arthritis. This systemic symptom results from the immune system’s response to inflammation. If you experience ongoing fatigue alongside other joint complaints, an arthritis evaluation may be necessary.
People often experience fatigue, difficulty concentrating, or lack of motivation even before joint problems become apparent. A general feeling of being unwell (malaise) may also accompany this systemic tiredness. If you have unexplained exhaustion combined with joint discomfort, stress may not be the only culprit.
6. Clicking or Grinding Sounds (Crepitus)
Crepitus—the sensation of cracking, popping, or grinding in joints during movement—is a common early indicator of arthritis. This symptom suggests that the joint’s lubricating synovial fluid may be decreasing or that cartilage within the joint is deteriorating.
Crepitus is more likely to occur with osteoarthritis. You may hear or feel these sounds when walking, kneeling, or bending, often accompanied by stiffness or discomfort. While occasional joint noise is normal, frequent or painful crepitus can signal underlying joint degeneration.
7. Family History or Other Autoimmune Conditions
Your family history may influence your arthritis risk. If a parent or sibling has arthritis, you could be genetically predisposed to developing the condition, especially autoimmune types like lupus or RA.
Additionally, having other autoimmune conditions—such as thyroid disease, psoriasis, or celiac disease—increases your arthritis risk. These conditions often share similar immune system defects that can trigger joint inflammation.
Read More: 7 Practical Home Modifications for Arthritis-Friendly Living
Diagnosis and Testing Options

During your physical examination, physicians will assess your joints for warmth, redness, and swelling. They’ll also evaluate joint mobility to help determine your condition.
The type of arthritis you may have is determined by analyzing various bodily fluids. Medical professionals often examine samples of blood, urine, and joint fluid. To obtain joint fluid, doctors clean and numb the area before inserting a needle into the joint cavity to extract a sample.
These tests help identify the joint problems that could be causing your symptoms:
X-rays: Using low radiation levels, X-rays can reveal bone spurs, cartilage loss, and damage. While they might not detect early arthritic changes, doctors frequently use X-rays to monitor disease progression.
Computerized Tomography (CT): CT scanners combine X-rays from multiple angles to create cross-sectional images of internal structures. CT scans can visualize both bone and surrounding soft tissues.
Magnetic Resonance Imaging (MRI): MRIs combine radio waves with powerful magnetic fields to create detailed cross-sectional images of soft tissues, including cartilage, tendons, and ligaments.
Ultrasound: This technology uses high-frequency sound waves to image soft tissues, cartilage, and fluid-containing structures (bursae) near joints. Doctors also use ultrasound to guide needle placement when injecting medications into joints or extracting joint fluid.
Read More: 9 Essential Supplements for Joint Health and Arthritis Relief
How Early Treatment Can Help
Starting treatment as soon as arthritic symptoms appear can significantly impact long-term outcomes. Treatment requires a multifaceted approach that may include:
Patient Education: Understanding your condition immediately following diagnosis helps you prepare for its symptoms, effects, treatments, and potential outcomes.
Nonpharmacologic Therapy: Physical and occupational therapists play crucial roles in supporting recovery while pharmacologic treatments are administered. These therapies can be highly beneficial in disease management, focusing on exercises that strengthen muscles, improve flexibility, and alleviate pain and spasms.
Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen can help manage pain. For more severe cases, treatment may include Disease-Modifying Anti-Rheumatic Drugs (DMARDs), biologic medicines, anti-inflammatory steroids, or other specialized medications.
Additional Treatments: According to the Arthritis Foundation, options may include plasma injections, counterirritants, or other medications. Surgery may be necessary for some patients.
When to See a Doctor
Arthritis is not a specific diagnosis but rather a general term covering more than 100 diseases and related conditions. Determining the exact type of arthritis or related condition you have is the first step in receiving optimal care and developing an effective management plan.
Some forms of arthritis require immediate treatment. Early intervention can help maintain joint function and prevent other serious health issues, particularly with types of arthritis that can cause irreversible joint damage.
However, mild or infrequent joint problems might not require urgent medical attention. Still, it’s wise to discuss your joint health and any arthritis concerns with your doctor.
Watch for these potential arthritis symptoms:
- Pain, swelling, or stiffness in one or more joints
- Joints that feel warm to the touch or appear red
- Joint stiffness or soreness
- Difficulty performing daily tasks or moving a joint normally
- Any joint symptoms that concern you
If you’re experiencing worrisome joint problems, scheduling an appointment with your healthcare provider is a smart first step. However, diagnosing arthritis can be challenging, so you may need to consult a specialist. Rheumatologists are experts in diagnosing and treating disorders of the joints, muscles, and bones. They’re qualified to treat all forms of arthritis, particularly those requiring complex care and diagnoses. If you’re diagnosed with degenerative arthritis, your physician may recommend seeing an orthopedic specialist.
Read More: Expert Advice: 8 Ways to Support a Loved One with Arthritis
Final Thoughts
Most people in their thirties dismiss joint pain, stiffness, or swelling, assuming it results from temporary overuse or natural aging. Ignoring these early warning signs can lead to delayed diagnosis, disease progression, and irreversible joint damage with reduced mobility. Once symptoms worsen, treatment options become more limited.
The positive news is that early detection and intervention can significantly improve outcomes. With proper treatment—including medications, lifestyle changes, and supportive care—doctors can manage symptoms, slow disease progression, and help you maintain an active, pain-free life.
Your body typically provides subtle warning signs before more serious problems develop. Pay attention to these signals. While arthritis may begin quietly, there’s always a reason your joints are aching—and addressing it early can make all the difference in your long-term joint health and quality of life.
References
- https://www.proortho.com/osteoarthritis-in-your-20s-and-30s-is-a-real-thing/
- https://www.aarp.org/health/conditions-treatments/arthritis-symptoms/
- https://www.houstonphysicianshospital.com/10-early-signs-of-arthritis-you-should-not-overlook/
- https://fortune.com/well/2023/08/23/arthritis-affects-15-percent-adults-older-than-30-risk-factors/
- https://livehealthy.muhealth.org/stories/joint-pain-your-30s-and-40s-why-it-happens-and-how-handle-it
- https://www.verywellhealth.com/early-onset-arthritis-5113831
- https://www.mayoclinic.org/diseases-conditions/arthritis/diagnosis-treatment/drc-20350777
- https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/arthritis-diagnosis
- https://www.arthritis.org/health-wellness/about-arthritis/understanding-arthritis/diagnosing-arthritis
- https://www.arthritis.org/diseases/osteoarthritis
- https://my.clevelandclinic.org/health/diseases/12061-arthritis
- https://www.hss.edu/health-library/conditions-and-treatments/rheumatoid-arthritis-early-diagnosis-treatment
- https://www.arthritis.org/health-wellness/about-arthritis/understanding-arthritis/when-joint-pain-means-its-time
- https://www.mayoclinic.org/symptoms/joint-pain/basics/when-to-see-doctor/sym-20050668
In this Article
















