A diagnosis of C3 glomerulopathy often raises one important question: Does this mean kidney failure is inevitable? It’s an understandable fear. The disease is rare, poorly explained outside specialist settings, and closely tied to kidney function, which makes the stakes feel immediate and high.
Search online, and the anxiety usually gets worse. Many sources focus on advanced cases or quote statistics without context. That can make it seem like the outcome is already decided. In reality, long-term research and clinical follow-up tell a more nuanced story.
C3 glomerulopathy can lead to kidney failure, but it does not do so in everyone. Progression is highly variable. Some people experience a slow decline over decades. Others remain stable for long periods with relatively preserved kidney function. Some patients move between phases of activity and stability rather than following a straight downward path.
What this really means is that the diagnosis itself is not a prediction. Risk depends on patterns: how active the disease is, how early it’s detected, how the complement system is behaving, and how closely the condition is monitored and managed over time.
This article focuses on what long-term data actually shows, not fear-driven assumptions. Understanding risk in C3 glomerulopathy starts with understanding variability, not assuming the worst.
What Kidney Failure Means in C3 Glomerulopathy
When people hear the term kidney failure in relation to C3 glomerulopathy, it often sounds abrupt and final. In reality, kidney failure is the endpoint of a long process, not a sudden switch that flips overnight. Understanding how chronic kidney disease fits into that process helps separate what is possible from what is inevitable.
C3 glomerulopathy causes ongoing injury to the glomeruli, the microscopic filters that clean the blood. That injury unfolds over time. The key point is this: kidney failure represents one possible outcome of long-term damage, not the default course for every patient.
Chronic Kidney Disease vs. Kidney Failure
C3 glomerulopathy is classified as a complement-mediated kidney disease because abnormal activation of the complement system damages the glomeruli. When this damage persists, it leads to Chronic Kidney Disease, or CKD.
CKD describes a gradual decline in kidney function measured over months or years. It ranges from mild impairment to severe loss of filtration capacity. Importantly, CKD is a broad category. Many people live for years, even decades, with stable CKD and never reach kidney failure.
Kidney failure, also called end-stage kidney disease, is the final stage of CKD. It occurs when the kidneys can no longer regulate fluid balance, electrolytes, acid-base status, and waste removal without medical support. At that point, dialysis or kidney transplantation becomes necessary to sustain life.
Not all CKD progresses to kidney failure. In C3 glomerulopathy, progression depends on disease activity, response to treatment, and how much irreversible damage has already occurred.
Read More: Polycystic Kidney Disease: Early Signs and Treatment Options
What “End-Stage Kidney Disease” Means Clinically
From a clinical standpoint, end-stage kidney disease is usually defined by an estimated glomerular filtration rate below 15 mL/min/1.73 m². Numbers alone, however, are not the full picture.
Symptoms matter. Some people develop fluid overload, persistent nausea, fatigue, shortness of breath, or dangerous electrolyte imbalances before reaching that numerical threshold. Others may tolerate lower eGFR levels for longer, with fewer symptoms. The decision to start dialysis is based on overall clinical status, not just a lab value.
In C3 glomerulopathy, kidney failure is rarely a sudden event. Most patients who progress show a clear pattern over time: rising creatinine, falling eGFR, increased proteinuria, and signs of chronic scarring on biopsy. These changes typically unfold over years, not weeks.
Why Progression Is Often Gradual, Not Sudden
The kidneys have a significant functional reserve. Even as some glomeruli are damaged, others continue to compensate. In C3 glomerulopathy, complement-mediated injury slowly leads to inflammation and scarring. As healthy tissue is replaced with scar tissue, filtration capacity declines.
This process is cumulative and usually incremental. That’s why trends matter more than isolated lab results. A single abnormal test does not define kidney failure. Consistent patterns over time do.
Regular monitoring allows clinicians to distinguish between temporary fluctuations and true progression. It also creates opportunities to slow further damage through blood pressure control, proteinuria reduction, and targeted therapies when appropriate.
Understanding kidney failure in the context of C3 glomerulopathy means recognizing it as a long-term risk and not an immediate outcome. The disease moves on a timeline measured in years, and for many patients, careful management significantly alters that timeline.
How C3 Glomerulopathy Affects the Kidneys Over Time
C3 glomerulopathy is caused by dysregulation of the alternative complement pathway, a part of the immune system that helps fight infections. In this condition, the system stays active when it shouldn’t. The result is persistent deposition of complement component C3 within the glomeruli, the kidney’s filtering units.
Research supported by the National Institutes of Health shows that this ongoing complement activation drives chronic inflammation, even during periods when symptoms appear mild or stable. The disease does not need to feel active to cause microscopic injury. That’s one reason C3 glomerulopathy can progress quietly.
Each inflammatory episode damages the glomerular basement membrane, a critical structure responsible for filtration. Unlike skin or liver tissue, glomeruli have very limited regenerative capacity. When injury occurs repeatedly, healing happens through fibrosis rather than repair. Functional tissue is gradually replaced with scar tissue.
As scarring accumulates, filtration efficiency declines. Protein begins to leak into the urine, blood pressure becomes harder to control, and waste products are cleared less effectively. This process unfolds over time, often in fits and starts rather than in a straight line.
Importantly, two patients with the same diagnosis can have very different symptoms.
What predicts outcome is not the disease label, but the level of ongoing activity. Persistent proteinuria, repeated inflammatory flares, progressive scarring on biopsy, and poor response to treatment signal a higher risk. Stable labs, controlled protein loss, and quiet disease signal a slower course.
What the Data Shows About Kidney Failure Risk
Because C3 glomerulopathy is rare, most outcome data come from observational cohorts followed over long periods rather than large randomized trials. These studies track patients in real-world clinical settings, which provides a useful perspective but also introduces variability.
Across multiple cohorts published in nephrology journals, the pattern is consistent: a substantial minority of patients progress to kidney failure over time, while others maintain usable kidney function for many years or even decades.
Most long-term studies suggest that approximately one-third to one-half of patients may reach end-stage kidney disease within 10 to 15 years. The exact percentage depends heavily on who was studied, when they were treated, and how advanced the disease was at diagnosis.
These numbers describe population-level risk, not individual destiny. They reflect averages across diverse patients with very different starting points and disease behavior.
Why Reported Rates Vary So Widely
Progression rates differ significantly across studies because C3 glomerulopathy is not a single, uniform condition. Research cohorts often include:
- Different disease subtypes, such as dense deposit disease and C3 glomerulonephritis
- Wide variation in baseline kidney function at diagnosis
- Differences in access to specialized care and complementary therapies
- Patients diagnosed in different treatment eras, before and after modern management strategies
- Uneven follow-up durations and outcome definitions
All of this affects reported outcomes.
This is why individualized prognosis matters far more than headline statistics. Population averages are useful for understanding risk, but they cannot tell you how a specific person’s disease will behave. What matters most is how active the disease is now, how it responds to treatment, and how trends evolve over time.
In C3 glomerulopathy, the future is shaped by patterns, not percentages.
Factors That Increase the Risk of Progression to Kidney Failure in C3 Glomerulopathy
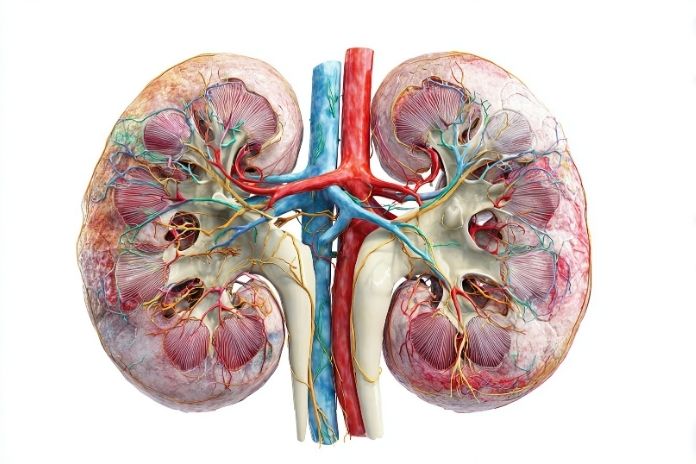
Not all patients with C3 glomerulopathy follow the same path. Some maintain stable kidney function for years, while others experience a gradual decline toward end-stage kidney disease (ESKD). Understanding what drives progression can help patients and clinicians focus on modifiable risk factors and closely monitor high-risk features.
Persistent Proteinuria
Persistent protein in the urine is one of the strongest predictors of kidney disease progression in C3 glomerulopathy. It is more than just a marker of damage, protein itself actively injures kidney tissue. Ongoing proteinuria promotes inflammation in the tubules and interstitium, which accelerates scarring. Patients with higher levels of proteinuria generally experience a faster decline in kidney function.
Excess protein triggers inflammatory signaling pathways within kidney tubules, leading to fibrosis and further reduction in filtration capacity. This relationship is observed across nearly all forms of glomerular disease, making proteinuria both a warning sign and a target for treatment. Controlling protein loss is therefore a central goal of therapy.
Read More: How to Reduce Proteinuria in IgA Nephropathy Naturally and Medically
Reduced Kidney Function at Diagnosis
Patients with reduced kidney function at the time of diagnosis have less functional reserve. Even modest disease progression can accelerate their progression toward ESKD. Baseline estimated glomerular filtration rate (eGFR) is one of the most reliable long-term prognostic indicators in C3 glomerulopathy.
Earlier diagnosis provides an opportunity to slow disease progression through interventions such as blood pressure control, proteinuria reduction, and targeted therapies. Catching the disease before significant loss of kidney function occurs improves the chances of long-term stability.
Poor Disease Control or Frequent Relapses
C3 glomerulopathy is driven by complement-mediated inflammation. Periods of active disease accelerate damage, while patients with stable, well-controlled disease progress more slowly. Frequent relapses or ongoing inflammatory activity increase the risk of cumulative injury and scarring.
According to nephrologists, patients who achieve sustained reductions in proteinuria and inflammatory markers generally have better long-term kidney survival, even if initial disease severity was high. This underscores the importance of consistent monitoring and aggressive management of active disease.
Specific Disease Subtypes and Pathologic Features
Certain subtypes of C3 glomerulopathy, such as dense deposit disease, and specific biopsy features, like extensive crescents or interstitial fibrosis, are associated with a higher risk of progression. These features indicate more aggressive disease or existing damage at the time of evaluation.
A kidney biopsy provides a detailed snapshot of disease activity and scarring at a single point in time, but it cannot predict the future with certainty. Pathology informs risk assessment, guides treatment decisions, and helps stratify patients, but it must be interpreted alongside clinical course and laboratory trends.
Can C3 Glomerulopathy Stay Stable Without Kidney Failure?
Yes. Long-term follow-up studies document patients who maintain stable kidney function for many years, especially with early diagnosis and consistent management.
Some individuals experience slow progression measured over decades rather than years.
Regular lab surveillance allows early detection of worsening proteinuria or declining eGFR, enabling timely adjustments in care.
C3 glomerulopathy behaves more like a spectrum than a single disease trajectory.
How Treatment Influences Kidney Failure Risk
Treatment aims to:
- Reduce proteinuria
- Control blood pressure
- Suppress active inflammation
- Slow CKD progression
There is currently no cure, but disease modification is possible.
Renin-angiotensin-aldosterone system (RAAS) blockade remains foundational. Lower proteinuria consistently predicts better outcomes.
Immunosuppressive therapies and emerging complement inhibitors are used selectively. According to experts at the Cleveland Clinic, responses vary, and treatment decisions are individualized, balancing benefits and risks.
How Fast Does Progression Typically Happen?
Progression in C3 glomerulopathy is usually gradual. Sudden kidney failure is uncommon unless triggered by severe acute injury.
Some patients show minimal change over long periods. Others progress steadily despite therapy. This variability underscores the need for personalized monitoring.
Disease activity often fluctuates. Remission phases can last years, especially with good blood pressure and protein control.
What Happens If Kidney Failure Does Occur?
Facing the possibility of kidney failure can be overwhelming, but understanding what it means and what options exist can make it more manageable. Kidney failure, or end-stage kidney disease (ESKD), occurs when the kidneys can no longer perform essential functions like filtering waste, balancing electrolytes, and regulating fluid levels.
While this represents a serious stage of C3 glomerulopathy, it does not mean the end of quality of life. Modern medicine offers effective ways to support kidney function and sustain daily living.
Kidney Replacement Options
If ESKD develops, patients typically have two main treatment options: dialysis and kidney transplantation.
- Dialysis temporarily replaces kidney function by filtering the blood through a machine (hemodialysis) or using the lining of the abdomen (peritoneal dialysis). It allows patients to maintain essential bodily functions, though it requires regular sessions and monitoring.
- Kidney transplantation offers a long-term solution. Many patients achieve an excellent quality of life after transplant. However, C3 glomerulopathy can recur in the transplanted kidney in some cases, making ongoing monitoring essential.
Early education and planning around these options improve outcomes, reduce stress, and allow patients to make informed choices rather than reacting in crisis. Even with kidney failure, care remains individualized, focusing on preserving health and maintaining lifestyle as much as possible.
Read More: Life After a Kidney Transplant: What to Expect in the First Year and Beyond
Can Kidney Failure Be Prevented in C3 Glomerulopathy?
While there is no guaranteed way to prevent kidney failure, research and clinical experience show that the risk can often be significantly reduced with careful management. Prevention in this context means slowing disease progression, protecting remaining kidney function, and addressing modifiable risk factors.
Frequent laboratory testing, tracking eGFR, creatinine, and urine protein, combined with routine blood pressure checks, allows clinicians to detect changes early. Early intervention can prevent small problems from becoming irreversible damage. Consistent monitoring provides the information needed to adjust medications, optimize treatment, and maintain kidney health for as long as possible.
Lifestyle measures do not correct the underlying complement disorder, but they are powerful tools for protecting kidney function.
Key strategies include:
- Maintaining healthy blood pressure through diet, exercise, and medications as prescribed.
- Avoiding medications that can harm the kidneys (nephrotoxins), such as certain pain relievers.
- Supporting overall health through balanced nutrition, regular physical activity, and adequate sleep.
These steps complement medical therapy and can meaningfully slow the trajectory toward kidney failure.
Warning Signs That Kidney Function May Be Worsening
Monitoring for early warning signs allows patients and clinicians to act before irreversible damage occurs. Key indicators include:
- Rising proteinuria: An increase in urine protein often precedes measurable declines in kidney function.
- Declining lab markers: Serial measurements showing falling eGFR or rising creatinine indicate that kidney filtration is decreasing.
- Worsening swelling or high blood pressure: Edema, puffiness, or uncontrolled hypertension can signal declining kidney function or active disease.
Persistent or increasing proteinuria and a downward trend in eGFR are among the most important clinical signals that chronic kidney disease may be progressing. These markers help guide nephrologists in deciding when to adjust treatment or intensify monitoring to slow further loss of kidney function. – Dr. Waqar Kashif.
Any sustained change in these markers should prompt a consultation with a nephrologist. The goal is timely evaluation and adjustment, not panic.
When to Talk to a Nephrologist About Long-Term Risk
Patients with C3 glomerulopathy should maintain an ongoing dialogue with their nephrologist, especially when:
- Symptoms or labs change:New swelling, fatigue, or shifts in lab results are reasons to schedule a discussion.
- Questions about prognosis or planning arise:Conversations about the future, including potential kidney replacement therapies, help patients prepare and make informed decisions.
- Shared decision-making is essential: Management works best when patients understand their condition, treatment options, and associated risks, enabling them to participate actively in care planning.
Proactive communication empowers patients to stay ahead of disease progression, ensuring that decisions are guided by knowledge rather than fear.
Final Takeaway
Does C3 glomerulopathy lead to kidney failure? For some patients, yes, but for many, progression is slow, and kidney function can remain stable for years. The course is highly variable.
What matters most are early detection, effective control of disease activity, and regular follow-up with a nephrologist. Monitoring proteinuria, lab markers, and kidney function over time allows timely intervention before irreversible damage occurs.
Individual risk factors, such as baseline kidney function, subtype, and treatment response, shape outcomes more than the diagnosis alone. In short, C3 glomerulopathy sets the context, but proactive management and monitoring determine the future.
References
- Biorasi. (n.d.). Rare disease spotlight: C3 glomerulopathy.
- Cleveland Clinic. (n.d.). C3 glomerulopathy (C3G).
- ERKNet. (n.d.). C3 glomerulopathy / IC-MPGN: Disease information.
- Frontiers in Nephrology. (2024). Advances in the understanding and management of C3 glomerulopathy.
- Indian Journal of Nephrology. (n.d.). Incidence and profile of C3 glomerulopathy: A single-center study.
- Kidney Disease: Improving Global Outcomes. (n.d.). Estimated glomerular filtration rate (eGFR). National Kidney Foundation
- Malacards. (n.d.). C3 glomerulopathy.
- MedlinePlus Genetics. (n.d.). C3 glomerulopathy. U.S. National Library of Medicine.
- MyKidneyDiseaseTeam. (n.d.). Treatments for C3 glomerulopathy.
- National Center for Biotechnology Information. (n.d.). C3 glomerulopathy. In StatPearls.
- National Center for Biotechnology Information. (n.d.). C3 glomerulopathy. In GeneReviews.
- National Institutes of Health. (2019). C3 glomerulopathy: Pathogenesis and treatment.
- Netherlands Journal of Medicine. (n.d.). C3 glomerulopathy: Clinical features and outcomes.
- PubMed. (2023). Clinical profiles and patterns of kidney disease progression in C3 glomerulopathy.
- ScienceDirect. (2026). C3 glomerulopathy: Emerging therapeutic approaches.
- Silence Therapeutics. (n.d.). Making sense of C3 glomerulopathy.
- WebMD. (n.d.). C3 glomerulopathy: Causes, symptoms, and treatment.
In this Article