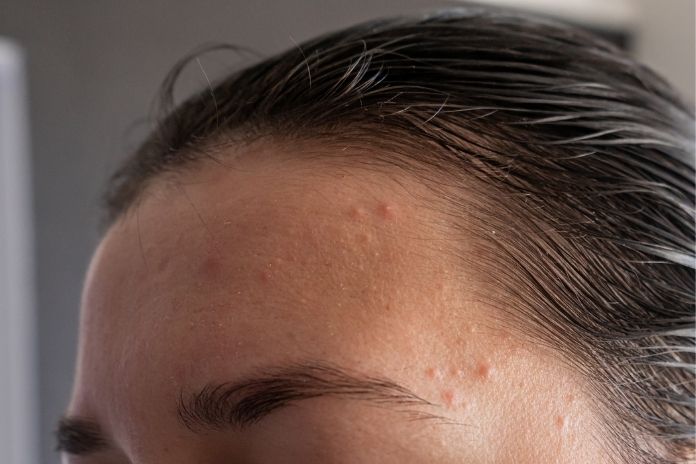
Have you ever run your fingers over your forehead, cheeks, or chin and felt tiny, stubborn bumps under the skin? They’re not red, swollen, or painful like regular pimples, but they don’t seem to budge either.
These small, skin-colored bumps are called closed comedones, and they’re one of the most common forms of acne that people struggle with, often without even realizing what they are.
The tricky part is that closed comedones don’t scream “breakout.” Instead, they quietly sit under the surface, creating rough, uneven skin texture and making your complexion look less clear. And because they’re not inflamed, they often get mistaken for dry skin, allergic reactions, or even ignored completely until they start clustering.
Here’s the frustrating part: closed comedones rarely go away on their own. They can linger for weeks, months, or longer if not addressed properly. But the good news is that with the right knowledge and routine, they’re absolutely manageable, and you can smooth them out without damaging your skin.
In this guide, we’ll break it all down: what closed comedones actually are, why they form in the first place, the most effective dermatologist-approved treatments, simple at-home care tips, and the common mistakes that make them worse. By the end, you’ll know exactly how to deal with them and how to keep them from coming back.
What Are Closed Comedones?
Closed comedones are a form of non-inflammatory acne, meaning they’re not red, swollen, or painful, but they can still be frustrating. They form when a pore (also known as a hair follicle) gets clogged with a mix of oil (sebum), dead skin cells, and debris.
The key difference lies in how the pore is blocked:
- Closed comedones: The pore’s opening is sealed at the surface, trapping the material inside. On the skin, they show up as tiny, firm, skin-colored or slightly white bumps. They often feel rough to the touch and can cluster together, creating uneven texture.
- Open comedones (blackheads): Here, the pore stays open. The trapped material inside oxidizes when it hits air, which turns it dark; that’s why blackheads look black.
- Whiteheads vs. closed comedones: The terms often get mixed up. Technically, a “whitehead” is a type of closed comedone that looks raised with a visible white tip caused by the keratin plug beneath the surface. Not all closed comedones look white; many just blend in with your skin tone.
Where they usually appear:
- Forehead, especially near the hairline.
- Cheeks
- Chin and jawline.
- Occasionally, on the chest, shoulders, or back.
Like most types of acne, closed comedones form when excess oil and dead skin cells plug one of your hair follicles (a.k.a. pores). This clog causes a raised bump that can be white (hence the name whitehead) or flesh-colored but isn’t yet inflamed or painful, Clarissa Yang, MD, chief of dermatology at Tufts Medical Center in Boston, tells.
What this really means is that closed comedones sit in a sort of middle ground; they’re not obvious breakouts yet, but they’re not “harmless” either. Left alone, some can turn into red pimples or cysts, which makes early care important.
What Causes Closed Comedones?

Closed comedones don’t appear overnight. They’re usually the result of several factors working together, from what’s happening inside your body to the products you put on your skin.
1. Excess Sebum (Oil) Production
Your sebaceous glands naturally produce oil to keep skin soft and protected. But when they go into overdrive, the excess sebum mixes with dead skin cells and forms a plug inside pores. Hormonal changes, like those during puberty, menstrual cycles, pregnancy, or conditions such as PCOS, often drive this overproduction.
2. Dead Skin Buildup
Normally, the skin sheds old cells through a natural process called desquamation. If that cycle slows down, dead cells pile up instead of falling away, which traps oil and debris inside the pore. Think of it like leaves clogging a gutter: nothing drains properly, so buildup collects beneath the surface.
3. Comedogenic Skincare or Makeup
Not all products are skin-friendly. Heavy oils, certain silicones, thick creams, or makeup that isn’t labeled non-comedogenic can block pores and worsen closed comedones. Even “clean” or “natural” products can cause problems if the ingredients are too rich for acne-prone skin.
4. Hormonal Fluctuations
Androgens, the hormones that ramp up oil gland activity, play a major role in comedonal acne. This is why teens often get breakouts, women may notice flare-ups around their cycle, and people with hormonal imbalances are more prone to stubborn bumps.
5. Lifestyle Factors
Daily habits matter more than most people think:
- Diet: Some studies link high-glycemic foods (like white bread, soda, and sweets) and dairy with increased acne risk. While the evidence isn’t definitive, many people report improvements after reducing them.
- Stress: Elevated cortisol can kick oil production into high gear, setting the stage for clogged pores.
- Improper Cleansing: Skipping face washing, leaving makeup on overnight, or using harsh cleansers that strip the skin barrier can all backfire, leading to more closed comedones.
Evidence shows microcomedones are the first step in acne (often appearing in adolescence), can progress into visible comedones and pimples, and acne frequently persists into adulthood, where lifestyle and skincare factors play a role.
Read More: Can Too Many Skincare Actives Damage Your Skin Barrier?
How Dermatologists Treat Closed Comedones

When closed comedones refuse to clear with basic skincare, dermatologists step in with targeted treatments. Their approach usually combines therapies that unclog pores, regulate oil, and speed up skin renewal. The goal is not just to treat existing bumps but also to prevent new ones from forming.
- Topical Retinoids
- Examples: Adapalene (Differin), Tretinoin, Tazarotene
- How they work: Retinoids are vitamin A derivatives that normalize cell turnover. By keeping dead skin cells from sticking together, they stop pores from getting clogged in the first place. Over time, they also help fade bumps that are already there.
- Evidence: A 2017 review in Dermatology and Therapy identified retinoids as the gold standard for comedonal acne, thanks to their proven long-term effectiveness.
- What to expect: Mild dryness or peeling at first, which usually improves with regular use and moisturizing.
- Chemical Exfoliants
- Alpha-hydroxy acids (AHAs): Glycolic acid and lactic acid work at the surface, dissolving dead skin buildup that roughens texture.
- Beta-hydroxy acids (BHAs): Salicylic acid penetrates deeper, breaking down sebum plugs inside the pore.
- Best for: Mild to moderate closed comedones, especially when cleansing alone isn’t enough. These acids are often prescribed as a complement to retinoids or as maintenance in between stronger treatments.
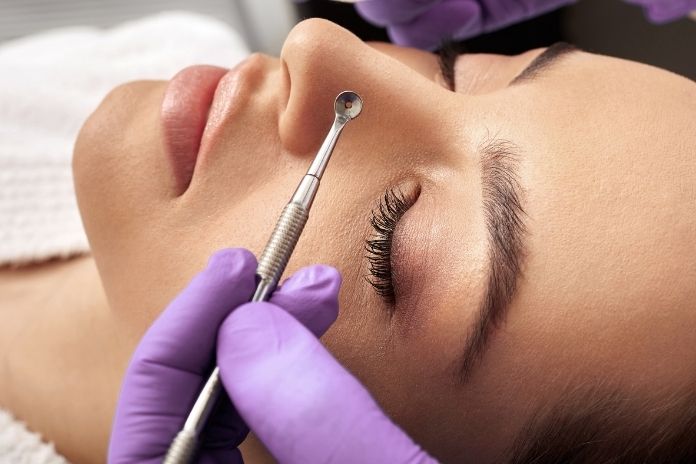
- Professional Treatments: Sometimes, hands-on procedures make the biggest difference:
- Facials with extractions: When performed hygienically by dermatologists or trained estheticians, these can safely remove clogged material.
- Chemical peels: Superficial peels with salicylic or glycolic acid exfoliate more intensively than at-home products, helping clear clusters of comedones.
- Microdermabrasion: A gentle mechanical exfoliation that smooths rough texture and improves product penetration.
- Prescription Options: For stubborn or widespread closed comedones, dermatologists may escalate care:
- Topical combinations: Retinoids paired with topical antibiotics or benzoyl peroxide if inflammatory acne is also present.
- Oral medications: In severe or resistant cases, oral isotretinoin (commonly known as Accutane) may be considered. This works by shrinking sebaceous glands and dramatically reducing oil production.
A classic review shows tretinoin reduces microcomedones (the earliest acne lesion) after 12 weeks of therapy, i.e., retinoids work on the plugs that become closed comedones, but they need time.
Bottom line: Dermatologist treatments are rarely one-size-fits-all. They often involve layering therapies, like a retinoid at night, salicylic acid in the morning, and the occasional peel, while adjusting strength and frequency to minimize irritation.
At-Home Skincare Tips for Closed Comedones

If your closed comedones are mild, you don’t always need prescription-strength treatments right away. Often, a consistent and gentle skincare routine makes a big difference. The key is to support skin turnover, keep pores clear, and avoid ingredients that make the problem worse.
1. Choose Non-Comedogenic Products
Look for labels that say “non-comedogenic,” “oil-free,” or “won’t clog pores.” Lightweight moisturizers, gel-based sunscreens, and breathable makeup formulas are less likely to trap oil and dead skin cells. Even if your skin feels oily, skipping moisturizer is a mistake; it can lead to rebound oiliness.
2. Gentle Cleansing (Twice Daily)
Wash your face morning and night with a mild, sulfate-free cleanser. Over-cleansing or using harsh foaming washes strips the skin barrier, which often leads to more oil production and irritation. Think balance, not squeaky-clean.
3. Exfoliate 2–3 Times Per Week
Chemical exfoliants (preferred): Salicylic acid (BHA) penetrates pores to dissolve oil and debris, while glycolic or lactic acid (AHAs) smooth surface buildup.
Avoid harsh scrubs: Physical exfoliants with rough beads or shells can cause micro-tears and worsen inflammation.
4. Targeted Spot Treatments
Niacinamide: Helps regulate oil production and calm irritation.
Benzoyl peroxide: Useful if you have a mix of closed comedones and inflamed pimples, but less effective on comedones alone. Apply spot treatments sparingly; more product doesn’t mean faster results.
5. Consistency Is Key
Closed comedones take time to form, and they take time to clear. Stick with a simple routine for at least 6–8 weeks before judging results. Jumping from product to product usually delays improvement.
Pro Tip: Introduce one active ingredient at a time. For example, start with salicylic acid a few nights a week, then add a retinoid later. Using AHAs, BHAs, and retinoids all at once often causes irritation, which can actually make comedones worse.
What NOT to Do
When it comes to closed comedones, the wrong approach can easily make things worse. These are the most common pitfalls dermatologists warn against:
1. Picking or Squeezing
Unlike blackheads, closed comedones are sealed under the skin. Trying to pop them doesn’t clear the pore; it just forces debris deeper or tears the surrounding skin. The result? Redness, scarring, dark spots, or even infection. If you’re tempted to “dig them out,” resist. Extraction should only be done hygienically by a professional.
2. Over-Washing or Harsh Scrubbing
Many people think scrubbing harder will clear bumps faster. In reality, aggressive cleansing damages the skin barrier and strips natural oils. Your skin compensates by producing even more sebum, setting up a vicious cycle of clogged pores. Stick to gentle cleansing twice daily, no more, no less.
3. Product Overload
It’s easy to assume that piling on multiple acids, masks, and serums will speed results. In truth, combining too many exfoliants often backfires, leading to raw, irritated skin that’s more prone to breakouts. Skincare works best when it’s consistent and minimal, one or two active ingredients at a time, not five.
4. Skipping Sunscreen
Many people skip SPF because they’re worried about breakouts. But sun damage not only worsens acne scarring, it also thickens the outer layer of skin, which can trap more oil and cells inside pores. The fix? Choose a lightweight, non-comedogenic sunscreen daily.
5. Expecting Overnight Results
Closed comedones clear slowly because they sit deeper under the skin’s surface. Switching products every week out of frustration prevents progress. Patience, 6 to 12 weeks of consistent care, is part of the treatment.
According to dermatologists, over-exfoliation is very common. “For some reason, people think exfoliating means ‘torture my skin like it has secret government information,'” Boston board-certified dermatologist Ranella Hirsch previously joked to Allure. “Over-exfoliating is probably the single most significant cause of breakouts.”
Bottom line: Gentle, steady care works better than aggressive fixes. If bumps persist despite a solid routine, that’s when it’s time to see a dermatologist.
Read More: Skincare Mistakes That Make Acne Worse (And How to Avoid Them)
When to See a Dermatologist
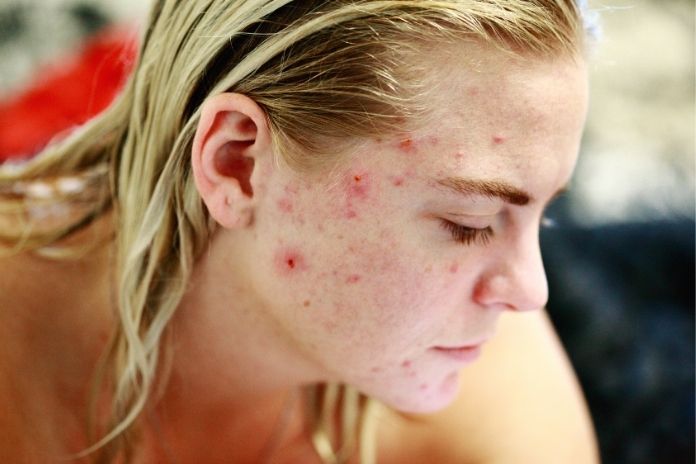
Self-care works for many people, but medical attention is needed if:
- Closed comedones persist despite 2–3 months of consistent skincare.
- Bumps spread or become inflamed.
- Texture worsens, affecting self-confidence.
- You have both comedones and cystic/inflammatory acne.
A dermatologist can tailor treatment, sometimes combining topical and oral options. They also ensure safe extractions when necessary.
Prevention Tips
Treating closed comedones is one thing, but keeping them from coming back is another challenge. Because they often recur, prevention is just as important as treatment. Here’s what dermatologists recommend for long-term skin health:
- Build a Consistent Skincare Routine. A solid daily routine should include four basics:
- Cleanse: Use a gentle, non-stripping cleanser morning and night.
- Treat: Apply a targeted active (like salicylic acid, glycolic acid, or a retinoid if tolerated).
- Moisturize: Even oily skin needs hydration; choose a lightweight, non-comedogenic formula.
- Protect: Finish with sunscreen every morning.
Consistency matters more than chasing the newest products.
- Use Oil-Free, Non-Comedogenic Sunscreen
SPF is non-negotiable, especially if you’re using retinoids or chemical exfoliants, which make skin more sun-sensitive. The right sunscreen prevents UV damage, reduces the risk of post-acne marks, and avoids pore clogging. Look for gel or fluid textures labeled oil-free or non-comedogenic.
- Always Remove Makeup Before Bed
Sleeping with makeup is one of the fastest ways to clog pores. Even “non-comedogenic” makeup can cause buildup if left on overnight. Use a gentle makeup remover or cleansing balm, followed by your regular face wash, to ensure skin is truly clean.
- Balance Diet and Hydration
While food isn’t the root cause of comedones, certain choices can make breakouts worse. Diets high in refined sugars, dairy, and processed carbs have been linked in some studies to acne flare-ups. Prioritize whole foods, fruits, vegetables, lean proteins, and drink enough water to support overall skin function.
- Manage Stress Levels
Chronic stress raises cortisol, a hormone that stimulates oil glands. The result? Extra sebum and a higher chance of clogged pores. Incorporating relaxation practices, like yoga, breathing exercises, journaling, or even short walks, can help keep stress (and skin) in check.
Pro Tip: Prevention doesn’t mean perfection. Occasional bumps happen, but with a consistent and gentle approach, they’ll be less frequent, less stubborn, and easier to treat when they do appear.
Conclusion
Closed comedones can be frustrating because they linger quietly under the skin, refusing to vanish no matter how much you scrub or spot-treat. But here’s the thing: they’re not permanent. They’re simply clogged pores stuck beneath the surface, and that means they respond best to time, consistency, and the right treatments, not quick fixes.
Topical retinoids help regulate skin cell turnover. Gentle chemical exfoliants like salicylic or glycolic acid slowly clear out what’s trapped. Sunscreen and proper moisturization protect your skin barrier so it can actually heal. And while progress may feel slow, each step in a steady routine is pushing you closer to smoother, clearer skin.
The most important takeaway is this: patience is your strongest weapon. Closed comedones rarely clear up overnight, but with persistence, they will improve. Think of skincare less like a sprint and more like a marathon; you may not notice every small change day by day, but over time, the difference becomes undeniable.
And remember, you’re not in this alone. If at-home care doesn’t seem to move the needle, dermatologists have powerful, safe tools that can help, from professional extractions to prescription treatments that target stubborn congestion directly.
Bottom line: closed comedones are not the end of your clear-skin journey. With science-backed care, consistency, and a little patience, they can be treated, prevented, and kept under control. Every bump is temporary; your commitment to your skin is what makes the difference.
References
- https://www.medicalnewstoday.com/articles/comedonal-acne
- https://dermnetnz.org/topics/comedonal-acne
- https://ijdvl.com/comedones-in-dermatology/
- https://evenlyclinic.com/blog/acne/what-are-comedones-how-to-treat-them
- https://www.laroche-posay.co.uk/en_GB/closed-comodones-causes-and-treatments.html
- https://medlineplus.gov/ency/article/003236.htm
- https://onlinedoctor.superdrug.com/comedonal-acne.html
- https://www.meetaugust.ai/en/library/blog/view/what-is-closed-comedones-vs-fungal-acne
- https://m.youtube.com/watch?v=_PKWdRO0DBE
In this Article