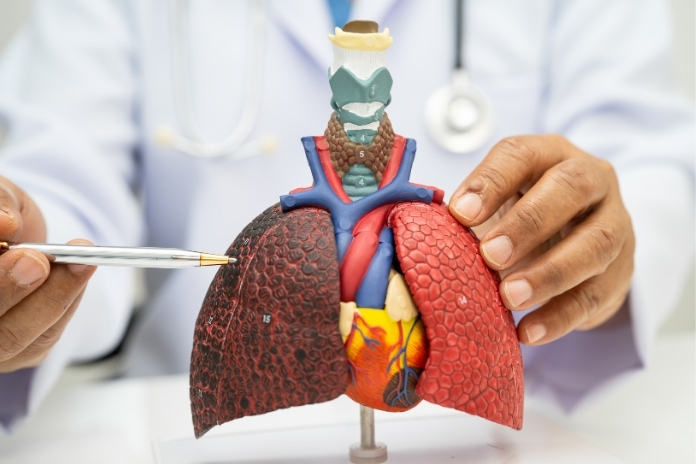
Lung cancer can be silent early because the lungs have few pain nerves, and tumors, especially peripheral ones, often don’t affect breathing until they’re bigger. Eligible people should discuss low-dose CT screening with their clinician to catch cancers before symptoms appear.
Many lung cancers start quietly, with no coughing, no chest pain, no dramatic warning. That silence is dangerous: cancers found because they caused symptoms are more likely to be advanced and harder to cure. But “silent” doesn’t mean harmless.
Early detection changes outcomes: randomized trials and large screening programs have shown that low-dose CT (LDCT) screening of high-risk, asymptomatic people finds cancers at an earlier, more curable stage and reduces lung-cancer deaths.
This article explains why lung cancer can be symptom-free at first, the subtle clues people commonly miss, who remain at risk even without symptoms, how LDCT screening works and who should consider it, and the steps to take if something is found. This is educational, screening decisions are individualized and best made with your clinician.
Why Lung Cancer Can Be “Silent”
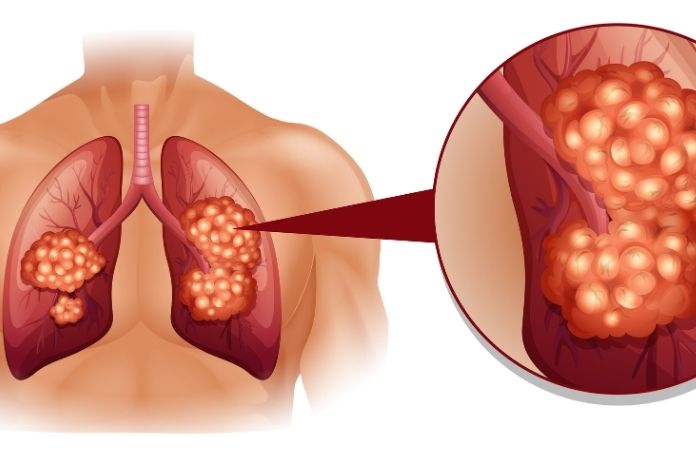
A simple anatomic fact helps explain the silence: large parts of the lung have very few pain receptors. Tumors growing inside lung tissue itself often don’t trigger pain signals until they expand to press on the chest wall, pleura, or nerves. That’s why a small peripheral tumor can quietly enlarge for months.
Central tumors (near main bronchi) are more likely to cause cough, bleeding, or airway obstruction and therefore may be noticed earlier, but many lung cancers begin at the lung periphery, especially adenocarcinomas, and produce no obvious symptoms.
Tumor size and location matter: a nodule that’s a centimetre or two in the outer lung won’t necessarily interfere with breathing, and the lungs can compensate for a gradual loss of function, masking early decline.
Finally, many people at risk already have chronic cough or breathlessness from smoking, COPD, or other lung disease, so a new cancer-related change can be mistaken for “normal” baseline symptoms. That combination, few pain fibers, peripheral growth, small size, and symptom overlap with common lung problems, is why lung cancer can be clinically silent until it’s advanced.
Subtle Early Clues People Often Miss

Not everyone with early lung cancer is symptom-free, but when symptoms occur, they’re often mild and slow to change. Watch for trends rather than one-off events.
Respiratory changes to notice: a new cough or one that changes or worsens, especially if it lasts >3 weeks; subtle shortness of breath during activities you used to handle easily; or repeated pneumonia or chest infections that recur in the same area of the lung. Cough accompanied by blood, even small streaks, is a red flag.
Voice and chest sensations: unexplained hoarseness (if a tumor affects the nerve to the vocal cord) or a persistent, mild chest ache or pressure that doesn’t feel like a typical muscle strain may be early signals.
Systemic hints: unintended weight loss, persistent fatigue, or reduced appetite over a few weeks can precede overt respiratory symptoms. Less common early pointers include shoulder or scapular pain (Pancoast-type tumors), new wheeze, or localized bone pain if spread has already occurred. Remember: change from your baseline matters, get persistent, unexplained shifts evaluated rather than waiting for dramatic symptoms.
“Some lung cancer symptoms warrant immediate attention. Others just need to be looked at within two or three weeks. A constant symptom is more of a problem than one that happens only for a short time and then resolves on its own. And combinations of symptoms are more concerning than one is by itself.” – Dr. Ara Vaporciyan, MD Anderson Cancer Center
Who’s At Risk Even with “No Symptoms”?
Risk isn’t defined by symptoms. People who should pay attention even when they “feel fine” include:
Tobacco exposure. Current and former smokers carry the highest risk, and cumulative pack-years matter (how many packs per day × years). Secondhand smoke also raises risk.
Environmental and occupational exposures. Lifetime radon exposure, asbestos, diesel exhaust, silica, and certain metals increase lung cancer risk. Radon exposure, for example, is a leading cause in never-smokers and is often undetected without home testing.
Personal and family factors. Prior chest radiation, chronic lung disease (COPD, pulmonary fibrosis), older age, and a family history of lung cancer all raise baseline risk. Air pollution and cumulative lifetime exposure further increase risk.
Even individuals who have never smoked can develop lung cancer if they have a combination of risk factors. If you have any of these risk factors, it’s worth discussing screening and vigilance with your clinician.
Read More: How to Check Your Lung Health at Home: Simple Tests and Warning Signs to Watch
Screening is the Safety Net, Low-Dose CT (LDCT)

Because early on lung cancers are often silent, LDCT screening is the only routinely recommended test proven to reduce lung-cancer deaths in high-risk, asymptomatic people. The landmark National Lung Screening Trial (NLST) and subsequent trials showed that annual low-dose CT scans reduce lung-cancer mortality by about 20% or more compared with chest X-ray in eligible populations. That benefit underpins current screening programs.
Who typically qualifies?
Guidelines vary slightly: the U.S. Preventive Services Task Force (USPSTF) recommends annual LDCT for adults 50–80 years with a ≥20 pack-year smoking history who currently smoke or quit within the past 15 years.
The American Cancer Society’s updated guidance also recommends annual LDCT for people 50–80 with a ≥20 pack-year history (details and individual criteria differ by organization). Eligibility should be assessed with your clinician.
Benefits vs risks
Benefits: Early detection, a high chance of curative treatment, and lower mortality in screened populations.
Risks: False positives (benign nodules that prompt follow-up scans or invasive tests), incidental findings, anxiety, and a small radiation exposure. Clinicians balance these when recommending screening.
What to expect?
LDCT is quick (usually minutes), noninvasive, and interpreted by radiologists trained to follow nodule management protocols. Results may lead to interval scans, PET-CT, or biopsy when indicated.
As UCLA’s Dr. Denise Aberle, a leader in lung-screening research, summarizes: “CT was shown to be the first and most effective way of reducing lung-cancer mortality.” Discuss eligibility, benefits, and possible follow-up before scheduling.
Simple decision flow:
Eligible? Discuss LDCT with your clinician – Schedule annual LDCT. Results: normal – continue annual screening; nodule detected – radiologist risk assessment – short-interval imaging, PET, or biopsy as indicated.
When to See a Doctor: Now, Red Flags
Some symptoms need prompt evaluation. See a clinician if you have: a cough lasting more than 3 weeks, coughing up blood (even small amounts), unexplained weight loss or persistent fatigue, persistent hoarseness, new or worsening shortness of breath, chest pain, recurrent pneumonia in the same area, or a new-onset wheeze. These signs don’t mean you have cancer, but they require assessment, imaging, and basic tests, which are the next step.
Urgent red flags that warrant immediate care include sudden neurologic symptoms (severe headache, weakness), new bone pain, or face/neck swelling and distended neck veins (possible superior vena cava syndrome), which may indicate advanced or obstructive disease and need rapid evaluation. Don’t wait; early assessment shortens the time to diagnosis and treatment when needed.
If Something is Found: The Diagnostic Pathway
Stepwise work-up
A suspicious nodule on LDCT usually prompts a diagnostic CT to better characterize size and location, and sometimes a PET-CT to assess metabolic activity and search for spread. Imaging guides whether a biopsy is needed.
Tissue diagnosis, the gold standard, is obtained by bronchoscopy for central lesions, CT-guided transthoracic needle biopsy for peripheral nodules, or surgical biopsy when required. Chest X-rays alone are not definitive.
Staging and molecular testing
Once pathology confirms cancer, staging (I–IV) uses imaging to map spread; early stages (I–II) may be treated surgically with curative intent, while advanced stages require systemic therapy and/or radiation.
Modern management increasingly depends on molecular and biomarker testing (EGFR, ALK, ROS1, KRAS, PD-L1, and others), which guides targeted and immunotherapy choices. Testing is standard for non-small cell lung cancer because it changes treatment and outcomes.
Multidisciplinary care
Thoracic surgeons, medical and radiation oncologists, pulmonologists, radiologists, and pathologists collaborate to build a personalized plan. Timelines vary, but teams typically move quickly from suspicious scan to tissue diagnosis and staging, so that definitive therapy can start without undue delay.
Read More: Top 10 Breathing Support Products to Enhance Lung Health Naturally
FAQs
Can lung cancer have zero symptoms until late?
Yes, many early lung cancers are asymptomatic because small or peripheral tumors don’t cause pain or airflow problems. Screening is how these are found before symptoms appear.
If I’m a non-smoker, should I worry?
Most lung cancers occur in smokers, but non-smokers can develop lung cancer from radon, occupational exposures, air pollution, prior radiation, or genetic factors. Screening is currently targeted to high-risk smokers; discuss individual risk with your doctor.
Is a chest X-ray enough?
No. Chest X-rays miss small nodules that LDCT can detect; LDCT is the proven screening tool for eligible people.
How often is screening done?
Typically, annually for eligible people; follow-up intervals after a suspicious finding depend on nodule size, appearance, and risk assessment.
Conclusion
Early-stage lung cancer rarely makes its presence obvious. Tumors often grow silently in the outer regions of the lungs, away from major airways and pain-sensitive areas, which means you might feel completely fine even as changes develop.
That’s why absence of symptoms shouldn’t be mistaken for good health, especially if you smoke, live with someone who smokes, or have long-term exposure to radon, air pollution, or workplace carcinogens like asbestos or diesel exhaust.
For people at higher risk, annual low-dose CT scans can make all the difference. Large clinical trials, including those published in the New England Journal of Medicine, show that regular screening detects lung cancers at earlier, more treatable stages and can lower mortality rates by 20–24%.
Early detection doesn’t just save lives, it allows for less aggressive treatment and a better quality of life after recovery.
If you notice subtle but persistent changes, like a chronic cough, unexplained fatigue, hoarseness, shortness of breath, or gradual weight loss, take them seriously. Talk to your clinician about your risk level and screening options.
Lung cancer caught early is often curable; lung cancer caught late rarely is. Awareness, prevention, and timely screening are your strongest defenses.
References
- https://pmc.ncbi.nlm.nih.gov/articles/PMC11814423/
- https://pubs.acs.org/doi/10.1021/acsomega.7b02035
- https://pubs.acs.org/doi/10.1021/acsami.4c16840
- https://www.nature.com/articles/s41392-023-01722-y
- https://www.researchgate.net/publication/388914285_Exploring_lung_cancer_microenvironment_pathways_and_nanoparticle-based_therapies
- https://www.sciencedirect.com/science/article/pii/S221287781930403X
- https://www.mdpi.com/2072-6694/13/14/3421
- https://www.oecd.org/content/dam/oecd/en/publications/reports/2023/10/adverse-outcome-pathway-on-deposition-of-energy-leading-to-lung-cancer_bdc46c0d/a8f262c2-en.pdf
- https://www.sciencedirect.com/science/article/pii/S1044579X22000499
- https://patents.google.com/patent/CA2444691A1/en
- https://onlinelibrary.wiley.com/doi/pdfdirect/10.1111/resp.12183_30
- https://link.springer.com/content/pdf/10.1007/978-3-031-84297-9.pdf
- https://iopscience.iop.org/article/10.1088/1742-6596/1294/6/062112/pdf
- https://escholarship.org/content/qt6972h04z/qt6972h04z.pdf
- https://europepmc.org/article/pmc/9841368
- https://www.researchgate.net/publication/393405339_Conquering_Cancer_from_Within_A_Relativistic_and_Transdisciplinary_Framework_Toward_Cellular_Recovery_and_Death_Transformation
- https://www.nature.com/articles/s41392-024-01979-x
- https://molecular-cancer.biomedcentral.com/articles/10.1186/s12943-025-02344-4
- https://core.ac.uk/download/287735478.pdf
- https://openarchive.ki.se/ndownloader/files/48935464
In this Article