When it comes to your heart, early detection and timely treatment are non-negotiable. Symptoms like chest pain, shortness of breath, dizziness, or extreme fatigue may point to restricted blood flow to the heart muscle, a warning sign you can’t afford to ignore. At this stage, doctors often recommend advanced tests and procedures to pinpoint the exact problem.
Two of the most important ones are angiogram and angioplasty. While the names sound similar, their roles in heart care are very different. Many people confuse the two because they’re often mentioned together during cardiac checkups. Here’s the thing: an angiogram is like a detective; it looks inside your arteries, identifies blockages, and maps the problem.
Angioplasty, on the other hand, is the fixer; it opens up those blockages and restores blood flow. One tells you what’s wrong, the other takes action to solve it. Understanding this difference could save not only confusion but also your life when facing a heart emergency.
This article breaks down both procedures in simple terms so you know exactly what to expect. You’ll learn how they work, when they’re needed, and what doctors look for at each step. We’ll also cover recovery, risks, and how these treatments fit into the bigger picture of heart health. By the end, you’ll be able to clearly distinguish between the two and feel more confident in making informed decisions. Because when it comes to your heart, clarity is power.
What Is an Angiogram?

An angiogram, also known as coronary angiography, is a diagnostic test that helps doctors see how blood flows through the coronary arteries. It’s part of a broader process known as cardiac catheterization, where a thin, flexible tube called a catheter is inserted into a blood vessel, usually in the groin, arm, or wrist, and carefully guided toward the heart.
“A coronary angiogram is the gold standard for diagnosing a blockage in an artery supplying the heart,” says Dr. Tariq Dayah, an interventional cardiologist at Houston Methodist. “It’s an invasive test, though, so we have to have convincing evidence that blockage is likely, whether that’s an abnormal stress test, EKG, or CT angiogram, or the person’s symptoms are severe enough.”
Once in position, a special contrast dye is released. Using X-ray imaging, doctors can then track the dye to identify areas where arteries are clear, narrowed, or completely blocked. This real-time picture is one of the most accurate ways to assess heart health and circulation.
When Doctors Recommend It
An angiogram is usually not the first step in diagnosing heart problems; it comes after initial, less invasive tests suggest something is wrong. Doctors may recommend the procedure if:
- You have unexplained chest pain (angina), either during exertion or at rest.
- Stress tests, echocardiograms, or ECGs show abnormal results.
- You experience ongoing shortness of breath, dizziness, or irregular heart rhythms.
- You already have a history of coronary artery disease, and new symptoms are developing.
By confirming where the blockages are and how severe they may be, an angiogram helps cardiologists decide whether medication, angioplasty, or bypass surgery is the best treatment.
Risks and Considerations
Although an angiogram is generally considered safe, it is still an invasive procedure and carries some risks. Common but minor issues include bleeding or bruising at the catheter insertion site. Some people may experience allergic reactions to the dye or temporary kidney strain as the body flushes it out.
Rare complications, such as irregular heartbeats, heart attack, or stroke, can occur, but these are uncommon in otherwise stable patients. For most people, the clarity and precision an angiogram provides far outweigh the risks, especially when heart disease is suspected.
What Is an Angioplasty?
Angioplasty, also known as percutaneous transluminal coronary angioplasty (PTCA) or percutaneous coronary intervention (PCI), is a minimally invasive procedure designed to restore blood flow in blocked or narrowed coronary arteries. While an angiogram identifies the problem, angioplasty actively fixes it.
In many cases, both procedures are coordinated: the angiogram pinpoints the blockage, and the angioplasty immediately opens it. In emergencies, such as a heart attack, doctors can perform both procedures in a single visit to quickly restore blood flow and reduce heart damage.
How Angioplasty Works
The process involves a few precise steps:
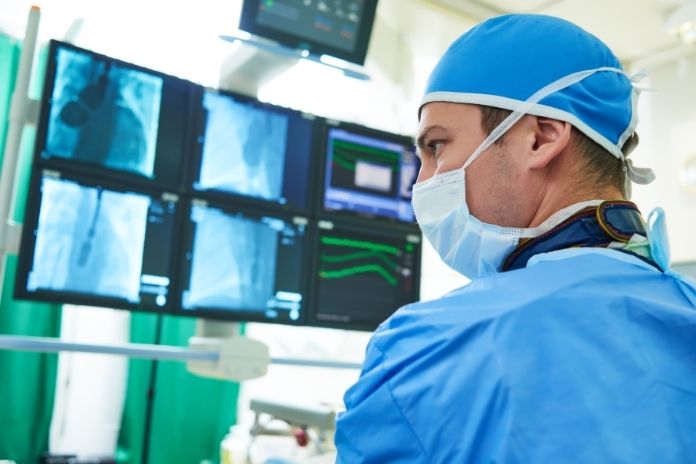
- A thin balloon catheter is guided through a blood vessel to the site of the blockage.
- Once positioned, the balloon is gently inflated, compressing plaque and widening the artery.
- In most cases, a stent, a small mesh tube, is inserted to keep the artery open for a long time.
This combination of balloon dilation and stent placement ensures the artery stays unobstructed, reducing symptoms like chest pain and lowering the risk of future cardiac events.
Risks and Considerations
Angioplasty is generally safe, but as with any procedure, it carries some risks. Possible complications include bleeding at the catheter site, damage to blood vessels, blood clots, irregular heart rhythms, or, rarely, a heart attack or stroke.
Most patients recover quickly, often returning home the same day or after an overnight observation, depending on the complexity of the procedure. Post-procedure care includes medication to prevent clot formation and lifestyle adjustments to protect the stent and overall heart health.
Key Differences Between Angiogram and Angioplasty
While angiograms and angioplasties are often discussed together, they serve very different purposes in heart care. Understanding the distinctions can help patients know what to expect and why each procedure is necessary.

What This Means for Patients
The angiogram identifies the problem, whereas angioplasty is the intervention that solves it. While an angiogram alone can guide treatment plans, angioplasty directly improves blood flow and can prevent heart attacks or ongoing chest pain. Both procedures require careful monitoring and follow-up, but knowing the differences helps patients mentally prepare for what’s diagnostic versus what’s therapeutic.
When You Might Need an Angiogram
“A coronary angiogram is used to get a lay of the land,” said Arun Kumar, MD, an interventional cardiologist at MU Health Care. “We check to see if there are any artery blockages, how severe they are, and what needs to be treated and what can be left alone with good lifestyle choices.”
Doctors typically recommend an angiogram when non-invasive tests or symptoms suggest that the heart’s blood vessels may not be delivering enough oxygen-rich blood. Common indications include:
- Persistent chest pain (angina): Especially if it occurs at rest or during minimal exertion and isn’t explained by other diagnostic tests.
- Abnormal ECG or stress test results: These tests can indicate reduced blood flow or electrical disturbances in the heart, prompting further investigation with an angiogram.
- Shortness of breath or unexplained fatigue: Difficulty breathing during everyday activities or unusual tiredness may signal that the heart is struggling to pump effectively.
- History of heart attack or coronary artery disease: Patients with previous cardiac events may need an angiogram to assess the severity of blockages, plan interventions, or evaluate stent or bypass effectiveness.
Angiograms serve as a precise roadmap, allowing cardiologists to see exactly where arteries are narrowed or blocked. This clarity guides treatment decisions, from lifestyle changes and medications to procedures like angioplasty or stent placement. By identifying problems early, angiograms can help prevent major cardiac events and improve long-term heart health.
When You Might Need an Angioplasty
Angioplasty is usually recommended when there is a clear need to restore blood flow to the heart. Common scenarios include:
- Significant coronary blockage: If an angiogram shows a narrowing of 70% or more in a major coronary artery, angioplasty can relieve the obstruction and reduce the risk of a heart attack.
- Acute heart attack (acute coronary syndrome): In emergency situations, angioplasty can be lifesaving by quickly reopening the blocked artery and minimizing heart muscle damage.
- Persistent symptoms despite treatment: When chest pain, shortness of breath, or other heart-related symptoms don’t improve with medications and lifestyle changes, angioplasty can offer relief.
- Assessment of overall heart health: Cardiologists consider the patient’s overall condition, the number of affected vessels, and imaging results to decide if angioplasty, with or without stent placement, is appropriate.
Angioplasty not only relieves immediate symptoms but can also prevent future cardiac events. It’s often combined with medications and lifestyle adjustments to maintain long-term heart health and improve quality of life. By addressing blockages promptly, patients can regain normal activity levels and reduce the stress on their hearts.
Research shows that angioplasty is typically reserved for cases where coronary artery stenosis reaches approximately 70% or more, a level considered hemodynamically significant. Below that threshold, the procedure is generally not recommended
Risks and Recovery for Angiogram and Angioplasty
Both angiograms and angioplasties are generally safe, minimally invasive procedures, but they do carry some risks. Being aware of these helps patients make informed decisions and take appropriate precautions.
Common Risks
- Bleeding or hematoma: Bruising or swelling can occur at the catheter insertion site, typically in the groin, wrist, or arm.
- Infection: Rare, but possible at the puncture site. Proper sterile technique minimizes this risk.
- Allergic reaction to contrast dye: Mild reactions include itching or rash, while severe reactions are very uncommon.
- Kidney stress: Contrast dye can affect kidney function, especially in patients with pre-existing kidney disease. Adequate hydration before and after the procedure helps reduce this risk.
- Serious cardiovascular events: Arrhythmias, heart attack, or stroke are extremely rare but potential complications.
Procedure Recovery
- Angiogram: Usually an outpatient procedure. Patients are monitored for vital signs and puncture site healing and are advised to avoid heavy lifting for at least 24 hours. Many can resume normal activities the next day.
- Angioplasty: Recovery is slightly longer. An overnight hospital stay allows for observation, especially for bleeding or vascular complications. Gradual return to physical activity typically occurs over 7–14 days, depending on stent placement and overall heart health.
Long-term Care and Lifestyle Considerations
- Medications: After angioplasty, patients often take antiplatelet drugs such as aspirin and P2Y12 inhibitors (e.g., clopidogrel), along with statins to manage cholesterol and reduce future risk.
- Lifestyle changes: Adopting a heart-healthy diet, engaging in regular physical activity, maintaining a healthy weight, and quitting smoking are critical for long-term cardiovascular health.
- Cardiac rehabilitation: Structured programs combine monitored exercise, education, and counseling to improve heart function, reduce recurrence risk, and enhance quality of life.
In essence, both procedures are powerful tools for diagnosing and treating coronary artery disease, but recovery and ongoing care are essential for maximizing benefits. Following medical guidance and incorporating heart-healthy habits ensures the best outcomes and supports long-term cardiovascular wellness.
Read More: 7 Heart-Healthy Habits You Can Adopt in Under 5 Minutes a Day
How to Prepare for Each Procedure

Proper preparation can make angiograms and angioplasties smoother and safer. Understanding what to expect before and on the day of the procedure helps reduce anxiety and ensures the medical team can perform the procedure effectively.
General Preparation
- Fasting: Patients are typically instructed not to eat or drink for 6–8 hours before the procedure to reduce the risk of complications from sedation.
- Medication review: Bring a complete list of current medications. Blood thinners or certain heart medications may need adjustment, so always follow your doctor’s guidance.
- Essentials to bring: Identification, insurance documents, and any relevant medical records. Wear comfortable clothing that’s easy to remove and won’t restrict access to the catheter site.
On the Day of the Procedure
- Hospital setup: You’ll change into a gown, and sedation or local anesthesia is provided to ensure comfort during the procedure.
- Angiogram: The doctor uses X-ray imaging to observe blood flow and detect any blockages in the coronary arteries. The catheter is guided through a blood vessel to the heart, and contrast dye highlights the arteries.
- Angioplasty: If a blockage is found, the same visit may proceed with balloon inflation to open the artery. Often, a stent is placed to keep the vessel open. The procedure combines diagnostic imaging with therapeutic intervention, sometimes in one seamless session.
Practical Tips
- Arrange for someone to drive you home if sedation is used.
- Wear minimal jewelry and avoid makeup or nail polish that could interfere with monitoring.
- Stay hydrated up to the allowed fasting window, as it helps kidney function, especially if contrast dye is used.
By following these preparation steps, patients reduce procedural risks and ensure a smoother experience. Being informed, organized, and relaxed contributes to safer outcomes and faster recovery.
Read More: Dietary Guidelines for a Healthy Heart: Foods That Support Cardiovascular Health
Which One Is Right for You? (Doctor’s Perspective)
The decision between an angiogram and angioplasty hinges on individual symptoms, test results, and overall heart health. An angiogram serves as a diagnostic tool to visualize blockages or narrowing in the coronary arteries. If significant issues are detected, an angioplasty may be recommended to treat the condition by widening the narrowed arteries.
In emergency situations, such as during a heart attack, both procedures can be performed in a single session. The angiogram identifies the blockage, and the angioplasty immediately addresses it, restoring blood flow to the heart muscle.
For non-urgent cases, seeking a second opinion can provide reassurance and ensure that all treatment options are considered. However, in critical situations, timely intervention is crucial, and combining both procedures can be life-saving.
Doctor’s Opinion:
Dr. Gregory Frey, M.D., an interventional cardiologist at Mayo Clinic, emphasizes the importance of individualized care: “Each patient’s situation is unique. While angiograms provide valuable diagnostic information, the decision to proceed with angioplasty should be based on a comprehensive assessment of the patient’s symptoms, overall health, and the severity of the coronary artery disease.”
This approach ensures that patients receive the most appropriate and effective treatment tailored to their specific needs.
Conclusion
In short, think of it this way: an angiogram is your heart’s detective, mapping blockages and identifying problems, while an angioplasty is the fixer, restoring blood flow and preventing serious complications. Understanding the difference empowers you to make informed decisions about your heart health, reducing anxiety and improving readiness when facing cardiac concerns.
These procedures, when used appropriately, can not only relieve symptoms but also prevent further heart damage and, in many cases, save lives. Yet the most powerful step is prevention. A heart-healthy lifestyle, emphasizing a balanced diet rich in vegetables, fruits, and whole grains, consistent physical activity, stress management, and maintaining a healthy weight, can dramatically lower the risk of coronary artery disease and reduce the likelihood of needing invasive interventions.
Early recognition of symptoms is crucial. Chest pain, shortness of breath, fatigue, or unusual discomfort should never be ignored, because timely evaluation can make the difference between a manageable condition and a life-threatening event. Partnering with your cardiologist, adhering to prescribed medications, and embracing lifestyle habits collectively offer the strongest defense for your heart.
At the end of the day, knowledge, vigilance, and proactive care create a heart-smart approach that goes beyond procedures. By taking small but consistent steps, you not only protect your arteries but also enhance your overall quality of life, confidence, and long-term well-being.
References
- https://my.clevelandclinic.org/health/diagnostics/4977-angiography
- https://en.wikipedia.org/wiki/Angiography
- https://www.medicalnewstoday.com/articles/326825
- https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/angiogram
- https://www.nhs.uk/tests-and-treatments/angiography/
- https://www.ncbi.nlm.nih.gov/books/NBK557477/
- https://www.bhf.org.uk/informationsupport/heart-matters-magazine/medical/tests/angiogram
- https://www.nhsinform.scot/tests-and-treatments/scans-and-x-rays/angiography/
- https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/angioplasty-and-stent-placement-for-the-heart
- https://my.clevelandclinic.org/health/treatments/22060-angioplasty
- https://en.wikipedia.org/wiki/Angioplasty
- https://www.mayoclinic.org/tests-procedures/coronary-angioplasty/about/pac-20384761
- https://medlineplus.gov/ency/article/007473.htm
- https://www.nhs.uk/tests-and-treatments/coronary-angioplasty/
In this Article















