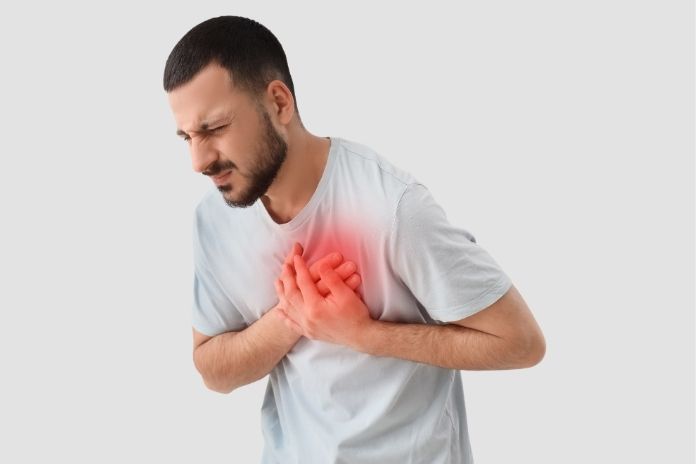
- A 34-year CARDIA study found men’s heart disease risk starts accelerating around age 35, about 7 years earlier than women.
- The gap is largely driven by early coronary heart disease in men and biological factors such as differences in hormones and cholesterol.
- Early screening and healthy habits in your 30s can significantly lower the long-term risk of heart disease.
Heart disease has traditionally been thought of as something that happens to men in their 50s or 60s, and this has influenced our opinion about heart disease and heart disease screening. However, recent studies indicate that the biology of heart disease begins much earlier and that age 35 may be an important milestone for men’s heart disease risk.
Many researchers studying premature cardiovascular disease in men find that the timeline may begin earlier than previously believed.
Men and women tend to have similar cardiovascular risk until about age 35. After that, men’s risk rises faster and remains higher than women’s. Researchers call this pattern the sex gap in heart disease. It highlights the importance of early prevention and heart health monitoring in men during their 30s.
This article takes a closer look at what the long-running CARDIA study discovered about men’s heart health. It also explains why this risk gap appears in the mid-30s and what men can do early to protect their hearts.
Read More: Signs of a Heart Attack vs. Panic Attack: When to Call 911
What the 34-Year CARDIA Study Found
The Study Design — Why This Evidence Is So Strong
The CARDIA study at Northwestern was one of the most in-depth “look-ins” into heart health. It began in the mid-1980s with a cohort of 5,112 healthy adults aged 18-30. Participants came from four major cities in the United States and represented both Black and white ethnic groups.
The study is significant because it began when none of the participants had any signs of heart problems. Most heart-related research begins when people are already in their middle years, and some signs of heart problems have already occurred.
The CARDIA study at Northwestern helped scientists to examine how risk factors evolve and when the gender differences in coronary heart disease first emerge.
Repeated clinical examinations, blood tests, and health assessments have been conducted over the years, with a median follow-up of approximately 34 years. This type of research allowed scientists to examine how heart health develops in people as they transition from young adulthood into middle age.
Because the study followed the same individuals over such a long period, it offered a rare opportunity to pinpoint the age at which men’s heart health turning point first occurs and to better understand whether men’s heart disease risk is different from that of women.
The Numbers — A Risk Gap That Begins Around Age 35
In early adulthood, men and women looked remarkably similar in terms of their risk of heart disease. In their 20s and 30s and even into their early 30s, the risk of heart disease was virtually identical between the sexes.
But then, around age 35, something changed. From that point forward, men’s risk of heart disease started to build more quickly. This supports the concept that men’s cardiovascular risk becomes apparent at a younger age during the mid-30s.
When researchers looked at the cumulative data, they saw that men reached the 5% risk of heart disease seven years before women. In other words, men reached the 5% risk of heart disease around age 50.5, while women did not reach that mark until around 57.5.
The difference was even greater for coronary heart disease, which occurs when the arteries that supply blood to the heart become narrowed or blocked. In that case, men reached the 2% risk of coronary heart disease at an early onset around age 48, while women did not reach that level of risk until about age 58.
The cumulative data also revealed a noticeable split in predicted risk. By age 50, the 10-year risk of cardiovascular disease was about 6% for men, while it was about 3% for women. This finding reinforces the reality that men have heart attacks earlier than women, a pattern observed across multiple cardiovascular studies.
The percentages might not be terribly high, but the issue is how quickly they rise. That rise begins in the mid-30s, marking the onset of coronary heart disease sex differences and the broader sex gap heart disease pattern that persists into adulthood.
Which Cardiovascular Conditions Drove the Difference
The study also examined which cardiac outcomes accounted for the difference between men and women. The most important cause was coronary heart disease, where plaque accumulates in the arteries supplying the heart.
Over the years, this accumulation reduces arterial diameter and can deprive the heart muscle of blood. When a plaque bursts or an artery is blocked, a heart attack occurs.
In contrast, there was no difference in the risk of stroke between the two sexes during the time frame of the study. There was also no difference in heart failure until later in life, as most people had not yet reached the age when heart failure is more prevalent.
Overall, the trends indicate that the earlier difference in cardiovascular risk between men and women in younger populations is mainly because of the earlier onset of coronary heart disease in men and the broader issue of premature cardiovascular disease in men.
Read More: Signs of a Heart Attack vs. Panic Attack: When to Call 911
Why Men’s Risk Climbs Earlier
The Estrogen Advantage Women Carry
One of the primary reasons why men tend to develop heart disease at a relatively younger age has to do with the role of estrogen on the heart and blood vessels. Before menopause, there appears to be a certain estrogen cardioprotective effect in women. This hormonal advantage plays an important role in explaining why men get heart disease earlier than women.
Estrogen interacts with various systems in the body to slow the progression of atherosclerosis.
Estrogen is also known to increase HDL, or “good” cholesterol, and decrease LDL, or “bad” cholesterol, which is associated with the buildup of plaque in the arteries. It also helps blood vessels coordinate their responses, thereby improving endothelial function and causing them to relax and dilate.
Research studies conducted under the Women’s Ischemia Syndrome Evaluation have found that women with lower levels of estrogen tend to have a significantly higher incidence of coronary artery disease. The takeaway from this research is clear: the estrogen cardioprotective effect is an important part of what causes the sex gap in heart disease.
Testosterone’s Double-Edged Role in Men
Hormonal biology can contribute to heart risk in males in the form of testosterone. According to a study conducted at Harvard Medical School, higher testosterone levels are associated with lower HDL cholesterol levels in men. This relationship is often described as the testosterone HDL cholesterol effect.
Since HDL helps clear excess cholesterol from the blood and transport it to the liver, lower HDL levels are associated with an increased risk of arterial plaque formation.
This cholesterol deficit starts early in life. As boys enter puberty and testosterone levels rise, HDL levels decrease to adult male levels. As a result, adult males have 20% lower HDL cholesterol than women of the same age.
This biological pattern helps explain why men get heart disease earlier than women and contributes to men’s cardiovascular risk at a younger age.
Beyond Hormones — What Traditional Risk Factors Don’t Explain
The major lesson from the CARDIA study at Northwestern is that the difference in heart disease risk between men and women persisted even after adjusting for traditional risk factors. This includes adjustments for body mass index, blood pressure, smoking status, physical activity, dietary quality, blood glucose, and non-HDL cholesterol.
Even after adjusting for all of these, men were more likely to experience cardiovascular risk factors earlier. This suggests that the sex gap in heart disease likely involves additional factors, such as hormonal influences, genetic differences, vascular biology, and immune or inflammatory mechanisms.
The Prevention Gap: Why Many Men Miss the Early Window
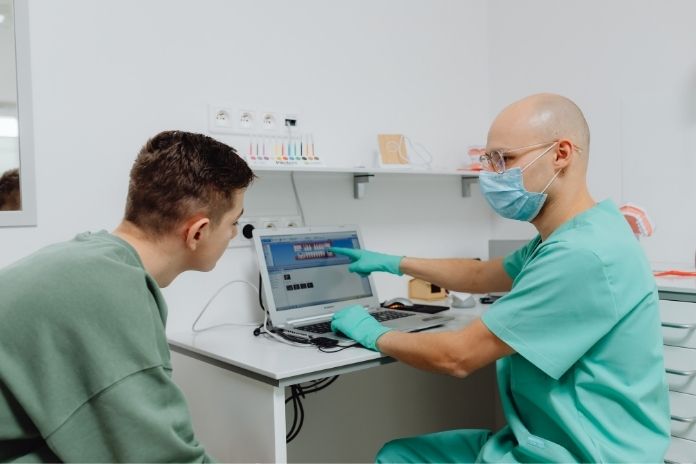
Men Are Four Times Less Likely to Attend Routine Checkups
Although biology accounts for only part of the early risk pattern, lifestyle and health habits also play a significant role in men’s preventive heart care.
Compared with women, young men are much less likely to visit a doctor for routine preventive care. Women regularly interact with the healthcare system through reproductive health visits, which provide natural opportunities for screening and counseling about long-term health risks.
Men in their 30s, on the other hand, may not visit a doctor unless something acutely hurts or fails them. As a result, important cardiovascular risk factors such as cholesterol, blood pressure, and blood sugar levels can quietly get out of range for years without being noticed.
Screening Guidelines Are Shifting — But Slowly
Due to the lack of regular screening, the men’s heart health turning point at age 35 often passes unnoticed.
To address this gap, the American Heart Association has revised its PREVENT risk equations to enable cardiovascular risk estimation from age 30 to 79. These risk prediction equations combine biological and lifestyle risk factors to estimate both short- and long-term risk.
By starting assessments earlier, there is a real opportunity to identify heart attack risk in men in their 30s and prevent premature cardiovascular disease in men before symptoms appear.
What Happens After Menopause
Women’s Advantage Disappears—The Risk Converges
Although women initially have some hormonal advantages, these advantages decline with age. After menopause, estrogen levels decline significantly, and the cholesterol profile changes. LDL levels increase, and HDL levels may decrease. Even the composition of arterial plaques may become more unstable.
With all these changes, the cardiovascular risk of a woman progressively increases after menopause. By the time she is about 65 years old, the lifetime risk of heart disease in a woman begins to converge with that of men.
This indicates that heart disease risk for men and women depends greatly on age and hormonal status.
Read More: Signs of a Heart Attack That Could Show Up a Month Before
What Can Men in Their 30s Do to Reduce Risk?

Concrete, Evidence-Grounded Actions — Not Generic Advice
This is confirmed by the CARDIA study at Northwestern, which found that the 30s are indeed a real opportunity for prevention.
Preventive cardiology involves being familiar with one’s own health statistics. Monitoring your blood pressure, cholesterol (both good and bad), fasting blood sugar, and weight is important for detecting men’s cardiovascular risk at a younger age.
Risk assessment tools such as the PREVENT risk equations and AHA assist physicians in estimating the risk of cardiovascular disease in the near future and over the long term.
Your lifestyle plays a significant role in your long-term heart health. Exercise strengthens blood vessels, increases good cholesterol, and lowers inflammation in the arteries. Smoking accelerates plaque buildup and significantly increases the likelihood of coronary heart disease in men with early onset.
Cardiologists now emphasize preventive cardiology strategies such as the American Heart Association’s Life’s Essential 8. If adopted early, these habits can greatly reduce heart attack risk in men in their 30s and prevent premature cardiovascular disease in men later in life.
Conclusion
The findings from the long-running CARDIA study challenge the traditional belief that heart disease primarily emerges in later adulthood.
Instead, the research shows that for men, heart disease risk at age 35 marks a meaningful shift in the trajectory of cardiovascular health. Around this age, men’s risk begins accelerating faster than women’s, eventually leading to an earlier onset of coronary heart disease in men.
Scientists continue to investigate what causes the sex gap in heart disease, including hormonal influences, cholesterol differences, and genetic factors.
For men entering their 30s, engaging with preventive healthcare, understanding cardiovascular risk factors, and addressing heart attack risk in their 30s can dramatically alter the long-term course of heart health.
Rather than a warning sign of inevitable disease, age 35 should be viewed as a starting line for proactive heart health, a moment when informed choices can protect the cardiovascular system for decades to come.
References
- American Heart Association. (n.d.). PREVENT™ calculator: Predicting risk of cardiovascular disease events. American Heart Association.
- American Heart Association. (2023). Life’s Essential 8: Updating and enhancing the American Heart Association’s construct of cardiovascular health. Circulation.
- Bhatia, R. T., et al. (2021). Sex differences in cardiovascular disease risk and outcomes. Journal of the American College of Cardiology.
- Harvard Health Publishing. (2020). Testosterone and the heart. Harvard Health Publishing.
- Khan, S. S., et al. (2024). PREVENT equations for cardiovascular disease risk prediction. Circulation.
- ScienceDaily. (2026, January 30). Study finds men’s heart disease risk begins accelerating at age 35.
- Shaw, L. J., et al. (2010). Insights from the Women’s Ischemia Syndrome Evaluation (WISE) study. Journal of the American College of Cardiology.
In this Article