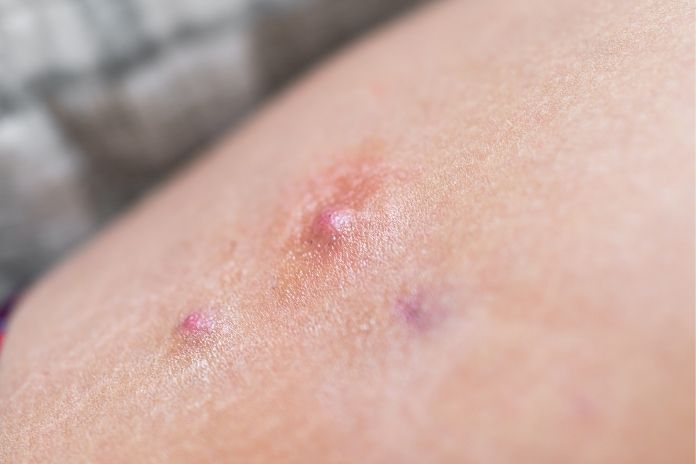
If you have experienced hidradenitis suppurativa (HS), you may already be familiar with the painful nodules, lumps, and abscesses that develop in your armpits, groin, and other moist skin areas where skin rubs against each other. When these lesions burst, fluid can sometimes get trapped under the skin. As the skin develops scar tissue over time, tunnels or tracts form, and they may continue to drain as they heal.
Because this process is complex, a single cream cannot clear HS. It is a chronic, inflammatory disorder that affects the body as a whole and usually requires a long-term, multi-step treatment approach.
In the early or milder stages of HS, doctors often prescribe topical antibiotic creams to help calm inflammation and reduce flare-ups. These creams help reduce surface bacteria, control secondary infection, and calm inflammation. However, topical antibiotics are rarely a standalone solution, and they are most effective when combined with treatment, lifestyle changes, and proper skin care.
Read More: Top 8 Psoriasis Creams: Soothing Skincare Solutions for Flare-Ups
What Causes HS and Why Antibiotic Creams May Help
Similar to acne, hidradenitis suppurativa is probably caused by a hereditary or acquired breakdown of the hair follicle epithelium that makes it “leaky,” allowing more normal skin germs to pass through the skin barrier and triggering an immunological response.
The skin microbiota is influenced by hormones, nutrition, smoking, and obesity, all of which can exacerbate inflammation. Therefore, by inhibiting inflammatory proteins, altering hormone levels, or decreasing hair density, medicinal treatments for HS aim to lower the bacterial burden on the skin and the overreactive immune response to these bacteria.
Blackheads, pimples, and boils are common symptoms of HS, which is treated similarly to acne in its early stages. However, HS can develop into a chronic condition that leaves bacterial tunnels beneath the skin’s surface and irreversible scars.
Antibiotic creams reduce the risk of bacteria getting into the open or draining lesion. Keeping sores clean and reducing inflammation helps them heal faster. Some topical antibiotics also reduce the disgusting odour from draining HS lesions and prevent minor flare-ups from worsening.
How Antibiotic Creams Work in HS

Doctors frequently use antibiotics as part of HS treatment, even though HS is not infectious and is not caused by an infection. In addition to their well-known ability to combat bacteria, some antibiotics can help reduce skin irritation and edema.
The medication helps reduce an overactive immune response, which doctors refer to as an anti-inflammatory impact. Antibiotics could be helpful for:
- Reducing bacteria on the skin that might irritate.
- Speeding the healing of nodules (particularly when combined with colchicine).
- Lowering bumps or stopping new ones from occurring.
- Reducing inflammation throughout the body and beneath the skin.
- Controlling symptoms such as drainage, pus, and odor.
A topical antibiotic, applied directly to the skin, may be helpful for mild to moderate HS. If you have moderate to severe HS, your dermatologist might recommend an oral antibiotic. Additionally, flare-ups can be treated or avoided using oral antibiotics.
Hidradenitis suppurativa is a chronic (long-term) inflammatory disease. “It can be excruciating,” says Dr. Anthony Fernandez, MD, PhD, a dermatologist at Cleveland Clinic in Ohio. “Aside from medical and surgical treatments, weight loss is another step you can take to manage HS.”.
Top Criteria for Choosing an Antibiotic Cream
Selecting the right antibiotic cream for Hidradenitis Suppurativa (HS) is vital to controlling symptoms without worsening the condition. Not all are appropriate for regular or prolonged use. Anyone with HS often has sensitive, inflamed skin that can react badly to certain topical antibiotics.
The following factors should be considered while selecting an antibiotic cream:
Gentle Formula and Minimal Irritation: Skin affected by HS is often more sensitive to friction and irritation. The ideal topical antibiotic cream should be fragrance-free with non-comedogenic ingredients that help manage dry, burning, irritated, and stinging skin.
Safety for Repeated or Short-Term Use: When used correctly, the product should not pose a risk of allergic reactions or antibiotic resistance and is safe for repeated use as instructed.
Dermatologist Advice: Most of the time, pick a lotion a dermatologist has recommended or prescribed. A professional choice means the antibiotic is suitable for your HS.
Read More: If Sunscreen Is So Good for Your Skin, Why Do So Many People Still Skip It?
Top Antibiotic Creams for Hidradenitis Suppurativa

1. Clindamycin Topical
Several studies have demonstrated the effectiveness of topical clindamycin in treating HS. Topical clindamycin can function similarly to oral tetracycline in patients with mild HS. It is very effective in treating HS bumps near the skin’s surface, but less effective in treating deeper-seated tunnels, abscesses, or nodules in people with more serious conditions.
Topical clindamycin is available as a liquid solution or cream. It is typically administered twice daily to the affected HS areas and left to absorb.
2. Mupirocin
Mupirocin ointment treats bacterial skin infections by killing bacteria on the skin and preventing their growth. Gently rub the ointment into the affected skin, and wash your hands before and after application.
This drug should be applied externally only. Just wash your hands before using them if you are treating a hand infection. Keep it out of your eyes. Rinse your eyes well with cool tap water if you do.
Use it at the same time each day as instructed on the prescription label. Never use it more than what has been medically recommended. Even if you feel better, follow your care team’s instructions and take the medication for the entire prescribed duration.
3. Fusidic Acid Cream
Fusidic acid is a highly lipophilic antibiotic. Its fat-soluble nature allows it to penetrate the skin effectively. It can reach deeper layers of the skin and concentrate in inflamed tissue, helping it work where the infection is active.
The medication acts by stopping the growth of pathogenic germs. Similar principles apply to sodium fusidate, a salt of fusidic acid. Topical fusidic acid treats both superficial and deep skin infections.
It effectively treats skin infections caused by staphylococci, streptococci, and other bacteria sensitive to fusidic acid. Sodium fusidate ointment or cream containing fusidic acid is an antibiotic that rapidly treats skin surface infections, particularly minor ones.
4. Neomycin/Bacitracin/Polymyxin
The combination of bacitracin, polymyxin, and neomycin is available as a topical ointment. It is usually applied one to three times a day, depending on your doctor’s instructions.
Bacitracin ointment, polymyxin, and neomycin are available over the counter. Your doctor may, however, provide you with specific instructions on how to use this drug to treat your medical condition.
Pay close attention to the instructions on the container or those your doctor has given you, and ask them or your pharmacist to clarify any parts you do not understand. Use the neomycin, polymyxin, and bacitracin mixture precisely as prescribed. Please don’t take more or less of it, or use it more frequently than your doctor has prescribed or as stated on the packaging.
Use this drug only on the skin. Do not swallow the combination of neomycin, polymyxin, and bacitracin, and do not let it enter your nose or eyes.
A combination of bacitracin, polymyxin, and neomycin is used to treat minor skin injuries. However, you should not use this medication on deep cuts, puncture wounds, animal bites, severe burns, or injuries affecting large areas of the body.
If you have these injuries, you should contact your physician or seek immediate medical attention. It could be necessary to use an alternative course of treatment.
5. Chlorhexidine Cream or Wash
A suggested topical treatment for hidradenitis suppurativa is a chlorhexidine wash, which can help lower the bacterial load and lower the risk of infection and inflammation.
North American clinical management guidelines for hidradenitis suppurativa, published in the Journal of the American Academy of Dermatology in 2019, state that the medical management approach includes topical treatments such as chlorhexidine.
Based on the evidence available at the time of the review, the guidelines provide a therapy algorithm.
Applying a 4% chlorhexidine gluconate wash to the affected areas once a day while showering will help with mild-to-moderate hidradenitis suppurativa. Apply the wash to the affected areas, leave it on for 1 to 2 minutes, then rinse thoroughly.
Chlorhexidine should, however, not be applied to open wounds or in proximity to the mouth, ears, or eyes. Chlorhexidine reduces surface bacteria and breaks down bacterial cell membranes, which can exacerbate flare-ups of hidradenitis suppurativa.
Read More: Why Your Moisturizer Isn’t Working (And How to Layer Skincare the Right Way)
6. Retapamulin
Doctors approve the topical antibiotic retapamulin for the treatment of specific bacterial skin infections. Apply retapamulin ointment in a thin layer to the affected skin twice daily for five days, ideally at the exact times each day.
Pay close attention to the instructions on your prescription label, and if you have any questions, ask your doctor or pharmacist. Retapamulin should be used precisely as prescribed. Don’t take more or less of it, or take it more frequently than your doctor recommends.
During the first several days of retapamulin treatment, the affected skin area should start to improve in appearance. Call your doctor if, after taking this medication for three to four days, your symptoms worsen or do not get better.
7. Antibiotic + Anti-inflammatory Combinations
To treat minor symptoms, a topical antibiotic in liquid or gel form may be used. Topical antibiotics are the name for these medications. Your doctor may prescribe antibiotic pills, such as doxycycline (Monodox), clindamycin (Cleocin), or rifampin (Rimactane), or a combination of these medications for more widespread illnesses.
Another name for rifampin is rifampicin. Doctors may prescribe antibiotics for months to patients with serious illnesses.
8. Natural Antimicrobial Creams
- Menthol-Based treatments:
Vicks VapoRub and other menthol-based treatments may help relieve discomfort and irritation. One participant described how they manage itching when trying to fall asleep.
- Aloe Vera Cream:
Aloe vera cream’s anti-inflammatory, calming, and wound-healing qualities may make it worthwhile for HS. Some people may experience skin sensitivity with ointments, which might worsen discomfort. Always test a small amount of product on skin before applying it widely.
Always consult your physician before using any new products, and avoid using these ointments on open wounds.
- Baths with Bleach and Epsom Salts:
Bathing might be a practical over-the-counter therapy option because HS affects the skin. Baths may help if you experience symptoms all over your body. Two bath treatments that could benefit your skin are bleach baths and Epsom salt baths. Itching, discomfort, and skin inflammation can all be reduced with a bleach bath.
Bleach baths are still a popular therapeutic choice for patients with HS, especially during flare-ups, despite a lack of studies on their efficacy.
For those with HS, Epsom salt baths are another popular treatment option. Magnesium sulfate, commonly known as Epsom salt, may help ease nerve pain and relax your muscles.
- Antiseptic Washes:
Using antiseptic cleansers when bathing may be beneficial for those with HS. Apply these washes to the areas of skin affected by HS. If you’ve ever had surgery, your doctor may have suggested washing your body the day before with an antiseptic or antibacterial product.
However, many patients with HS also use washes daily to help prevent infection.
How to Use Antibiotic Creams Safely for HS

- Cleanse First: If recommended by your dermatologist, always start by gently cleansing the affected area with a mild, unscented cleanser or an antiseptic wash.
- Apply Thin Coat: Use your fingertip to apply a thin layer of the prescribed cream, lotion, or gel to the affected spots.
- Avoid Excessive Closure: Do not cover the treated area with a tight bandage or a close-fitting dressing unless otherwise instructed by a medical practitioner.
- Avoid Harsh Cleansers: Use only a mild cleanser. Scrubbing the skin after the treatment can irritate it.
- Frequency: The doctor knows what is best for your health, so you should always follow their instructions.
Read More: Best Hyaluronic Acid Moisturizers: Hydrate and Plump Your Skin for a Youthful Glow
When Topical Antibiotics Are Not Enough
Antibiotics are not the only treatment option, but they can help regulate HS flare-ups and reduce inflammation.
Biologics:
Biologic medications can target the immune system more directly. As of right now, three biologics have been approved by the US Food and Drug Administration (FDA) to treat HS:
- Adalimumab and its biosimilars (Humira)
- Bimekizumab, or Bimzelx
- Cosentyx (secukinumab)
Patients receive biologics as subcutaneous (under-the-skin) injections, which they often administer at home.
Additional Oral Drugs:
Doctors may prescribe the oral retinoids, such as isotretinoin or acitretin. If the flares of the condition coincide with hormonal changes, medications that affect hormones, such as finasteride, spironolactone, or hormonal birth control, may be beneficial.
Surgery and Additional Operations:
Doctors may consider specific methods for more severe circumstances. These consist of:
- Excision through surgery – Eliminates injured tissue
- Deroofing, also known as unroofing, opens and drains tunnels beneath the skin
- Targeting HS lesions with laser therapy lowers the risk of recurrence
Lifestyle and Adjunctive Measures That Help HS Healing
People with HS can better control their disease and lessen its contribution to a diminished quality of life by using self-management strategies and lifestyle adjustments.
Daily Skincare: If you have HS, keep up a mild skincare regimen. Avoid skin scrubs and use non-soap cleansers. To reduce bacteria, use antiseptic cleansers such as benzoyl peroxide (5–10%)—introduce them gradually to prevent irritation.
Pain Management: Pain management is a very crucial part of HS treatment. Cold compresses ease swelling. Ibuprofen and acetaminophen may ease discomfort somewhat, but for chronic, ongoing pain, you may need specialized medication from a pain specialist.
Nutrition and Weight Management: Keeping active and maintaining a healthy weight are essential for good health and well-being. The effects of HS treatments and whether nodes reduce in size when you lose weight remain unknown. Researchers don’t know how diet affects HS. Consider using an app or journaling food if you think certain foods might be triggering your HS symptoms.
Read More: 5 Must-Have Glycolic Acid Exfoliators to Smooth and Renew Your Skin’s Surface
Red Flags: When to Seek Medical Help

Effective treatment of hidradenitis suppurativa depends on early diagnosis.
Consult a dermatologist if:
- It hurts.
- Makes moving challenging.
- Doesn’t get better in a few weeks.
- Returns just after a few weeks of therapy.
- Appears in multiple places.
- Flares up very frequently.
A dermatologist can develop a treatment plan for you. A boil is not the only symptom of hidradenitis suppurativa; many sufferers also have other diseases.
A medical and surgical dermatologist-led healthcare team is beneficial for patients with hidradenitis suppurativa. When necessary, more experts are involved.
Conclusion
The treatment of Hidradenitis Suppurativa is more about recognizing a problem and acting wisely in the face of it than it is about discovering a “magic” cream. Topical antibiotic creams help wounds heal, control surface bacteria, and soothe the pain of mild flares.
Applied correctly and at the right time, they can prevent minor inconveniences from becoming significant suffering, because HS is a complex inflammatory condition; topical treatment alone is often inadequate for its driving factors. Knowing when creams can help and when to step up to a higher level of treatment can dramatically influence long-term results.
References
- Mayo Clinic. (March 21, 2025). Hidradenitis suppurativa: Diagnosis and treatment.
- Everyday Health. Colleen de Bellefonds. (Updated on January 2, 2025). 7 Dermatologist-Approved Skin-Care Tips for Hidradenitis Suppurativa
- HS Connect. Cristina Curp. (August 21, 2025). Medication Treatments for Hidradenitis Suppurativa: What You Should Know.
- Dermatology Advisor. Colby Stong. (February 20, 2025). Hidradenitis Suppurativa Treatment Guidelines Issued for Special Populations.
- UMass Chan Medical School Hidradenitis Suppurativa Center. Treatments.
- Max Mugambi. (Updated on December 12, 2025). Antibiotics for HS: What you need to know.
- DrOracle Medical Advisory Board & Editors. (2025, November 5). What is the recommended topical antibiotic treatment for hidradenitis suppurativa?
- Valerie Emuakhagbon, MD. (2023, November 8). Hidradenitis suppurativa (HS): Understanding your treatment options.
- Steven Daveluy, MD, FAAD. Topical medications and washes
- Cleveland Clinic. Mupirocin cream or ointment.
- National Library of Medicine. (Last Revised: June, 20, 2024). Neomycin, polymyxin, and bacitracin topical: MedlinePlus drug information:
- DrOracle Medical Advisory Board & Editors. (Updated: April 23, 2025). Is chlorhexidine (CHG) wash effective for hidradenitis suppurativa (HS)?
- National Library of Medicine. (2025, September 15). Retapamulin: MedlinePlus drug information
- Anastasia Climan, RDN, CDN and Mikayla Morell. (2024, October 29). 5 over-the-counter treatments for hidradenitis suppurativa to try.
In this Article