This past week, I faced a rather uncomfortable situation. The urgency to pee never seemed so high, and I was confused. My frequent bathroom visits made me think I have a Urinary Tract Infection. However, this straightforward assumption is not always right. Let’s see why.
You’re running back to the bathroom every five seconds. You can’t stop thinking that you have to pee, even though you just went. Possibly, there’s pressure or pain in your lower abdomen. You think it’s a urinary tract infection (UTI), but when your test results return, they’re normal again.
So, what’s going on?
If you’re stuck in this frustrating cycle of experiencing persistent urinary urgency without any signs of infection, it might be time to consider another possibility: Overactive Bladder (OAB).
Although UTIs and OAB may appear to be similar on the surface, they are two very different conditions. Misinterpreting one for the other not only means you get the incorrect treatment, and making your discomfort last longer.
In this article, we’ll understand the differences between UTI and OAB, including causes, symptoms, diagnosis, and treatment, so that you can understand your bladder health better and receive the right treatment.
Read More: 13 Useful Home Remedies For Treating Urinary Tract Infections
What Is a UTI?

A Urinary Tract Infection (UTI) is a very frequent infection, especially in females. It occurs when germs, usually Escherichia coli from the intestine, enter the urethra and begin to multiply within the bladder.
The infection can be confined to the bladder (a condition referred to as cystitis), but if it is not treated, it can ascend to the kidneys and lead to more severe complications such as pyelonephritis.
What makes UTIs fairly easy to identify is the clear-cut symptom cluster. Most individuals experience a burning sensation during urination, a sudden and frequent need to urinate (even if a very small amount of urine comes out), and alterations in the color or odor of urine. Cloudy, smelly, or even bloody urine is all quite possible. Pressure, pain, or discomfort in the lower abdomen or pelvis can also be experienced, particularly with bladder infections.
When a UTI progresses to the kidneys, symptoms become noticeable. Fever, chills, nausea, vomiting, and flank or back pain usually follow upper urinary tract infections.
Diagnosis is typically uncomplicated. A urine culture can identify the bacteria and white blood cells, which verify an active infection. Treatment is a brief antibiotic course, selected according to the bacteria found and sensitivity to antibiotics. People recover within a few days of treatment.
What Is Overactive Bladder (OAB)?

In contrast to a UTI, Overactive Bladder (OAB) is not an infection caused by bacteria. Rather, it’s an ongoing condition where the bladder muscles involuntarily contract and result in an urgent and irresistible urge to empty the bladder, even if the bladder is not full.
OAB is more common than most people know. The Urology Care Foundation says that it occurs in millions of men and women and can have a big influence on daily life and sleep. However, since it has overlapping symptoms with UTIs, OAB is often underdiagnosed or misdiagnosed.
Individuals with OAB generally experience eight or more daytime urinations and many nighttime ones. The nighttime one is called nocturia. The sensation may develop so strongly and suddenly that it results in urge incontinence, during which one loses a trickle of urine before making it to a bathroom. Notably, OAB symptoms do not have the burning discomfort or abnormal urinary modifications encountered with UTIs.
There is no one test for OAB. Diagnosis is based on a thorough assessment of patterns of symptoms, lifestyle, and ruling out other conditions, such as infections or structural abnormalities in the urinary system. Patients may be asked to maintain a diary, recording how often and how much they void, and any leakage episodes.
Key Differences Between UTI and Overactive Bladder
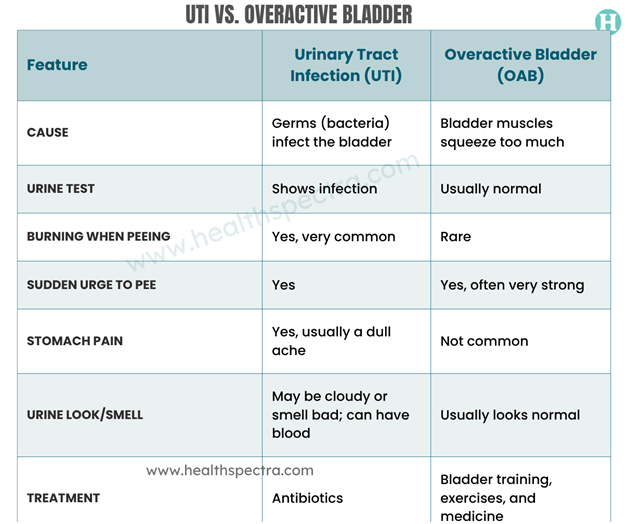 Although there is some overlap, UTIs and OAB are distinct in a number of significant respects, particularly cause, symptom profile, and treatment plans. Let’s discuss UTI vs. OAB in detail.
Although there is some overlap, UTIs and OAB are distinct in a number of significant respects, particularly cause, symptom profile, and treatment plans. Let’s discuss UTI vs. OAB in detail.
The Spread:
- UTIs are infectious. They start when bacteria penetrate the urinary tract, frequently resulting in painful urination, cloudy urine, and lower abdominal pain.
- OAB develops from non-infectious causes such as nervous signaling abnormalities or bladder muscle dysfunction. As a result, urine tests usually return clean despite continued symptoms.
Discomfort:
- A second major difference is the burning or discomfort. Dysuria is among the most frequent complaints in UTIs.
- In OAB, frequency and urgency are prominent, but burning is uncommon or non-existent.
Urinary Incontinence:
- Incontinence is also differently involved with each condition. Minor leakage may sometimes occur with UTIs due to bladder irritation.
- With OAB, however, urge incontinence, losing control before one can get to a toilet, is far more likely.
Treatment Plan:
- The treatments are vastly different. UTIs need to be treated with antibiotics in order to get rid of the infection.
- OAB, on the other hand, is treated with behavioral techniques, bladder retraining, pelvic floor therapy, and, in some instances, medications that relax the bladder muscles.
Read More: 11 Essential Oils for Urinary Tract Infection (UTI) for Faster Recovery
What If You Have UTI-Like Symptoms but Your Tests Are Negative?

This is a familiar situation. Several people visit the physician with the typical UTI symptom complex, urgency, frequency, and pain, only to learn their urine tests are negative for infection. When you face this time and time again, you might get frustrated and feel unsure.
But here’s the catch: not every bladder discomfort arises from infection. If your tests are repeatedly negative, it’s time to check out conditions that can imitate UTIs. These include
- Overactive Bladder (OAB): Characterized by urgency, frequency, and incontinence, without infection.
- Interstitial Cystitis (IC): Also known as bladder pain syndrome, this is a chronic condition that results in pelvic pain, pressure, and bladder pain.
- Vaginal Infections: Yeast infections or bacterial vaginosis may create burning or urgency.
- Pelvic Floor Dysfunction: Tight or out-of-sync pelvic muscles may worsen bladder control and produce similar symptoms.
If you find yourself trapped in this cycle, don’t just depend on those repeated doses of antibiotics. You require a more thorough assessment to determine the real cause of your symptoms and avoid unnecessary treatment.
How Is OAB Diagnosed?

Diagnosis of OAB starts with a thorough history of your symptoms. A urologist or gynecologist will probably ask you how many times you have to urinate during the day, if you wake up at night to urinate, and if you’ve ever leaked urine when you felt an intense urge.
You might be asked to keep a voiding diary for a few days. This allows your provider to see the frequency, timing, and amount of urination and any food, drink, or activity-related patterns that may be associated with them.
Then, urine tests are done not to diagnose OAB itself, but to exclude infection or blood in the urine.
In more serious cases, particularly when initial measures don’t improve things, additional testing may be prescribed. This may include:
- Bladder Ultrasound: To screen for inefficient emptying of the bladder
- Urodynamic Tests: These measure how well your bladder and urethra hold and pass urine
- Cystoscopy: A camera procedure to examine the interior of the bladder if structural issues are suspected
Occasionally, if pelvic floor problems are suspected, you might be referred to a pelvic health physical therapist.
Treatment of Overactive Bladder vs. UTI

Since the underlying causes are distinct, the treatments for these two ailments are not the same.
Treatments for OAB:
- Bladder Retraining: Scheduling visits to the bathroom and slowly lengthening the time between trips helps the bladder learn to retain urine for more than a brief time.
- Pelvic Floor Therapy: Kegels and other exercises can strengthen muscles that control urination. Biofeedback or physical manipulation by trained pelvic floor therapists can also promote faster recovery in people with OAB.
- Lifestyle Changes: Staying away from caffeine, alcohol, artificial sweeteners, and spicy foods may decrease bladder irritation. Proper fluid management and avoiding high amounts of alcohol help.
- Medications: Medications such as antimuscarinics (e.g., oxybutynin) or beta-3 agonists (e.g., mirabegron) relax bladder muscles and reduce symptoms.
- Nerve Stimulation Treatments: In cases of severe or refractory OAB, therapies like percutaneous tibial nerve stimulation (PTNS) or sacral neuromodulation might be an option.
Treating a UTI
- Antibiotics: Most bladder infections are cleared by a short treatment (typically 3–5 days for an uncomplicated infection).
- Flushing: Drinking lots of water washes bacteria out.
- Pain relief: Pain and urgency can be relieved with over-the-counter pain medication or urinary analgesics such as phenazopyridine while treatment is ongoing.
- Preventive Measures: Cranberry supplements and D-mannose have shown some potential in preventing recurrent UTIs, though they do not treat active infections.
Read More: All That You Need To Know About Urinary Incontinence – Get Educated!
When to See a Doctor

Not every urinary symptom needs emergency attention, but some signs shouldn’t be ignored. It’s important to seek medical care if:
- Your symptoms last more than a few days without improvement
- You’ve been treated for a UTI, but symptoms persist or recur.
- You have frequent urination at night that disturbs your sleep.
- You experience incontinence, especially if it’s new or worsening.
- There is bloody urine.
- You feel pain or pressure in your lower abdomen.
- You get fever, chills, or flank pain, which may be signs of a kidney infection.
Don’t wait or self-diagnose. A proper evaluation will ensure you’re not chasing the wrong problem with the wrong solution.
Final Thoughts
Bladder problems feel annoying, humiliating, and wearying, but relief is found in proper diagnosis.
Although UTIs and Overactive Bladder share similar symptoms, such as urgency and frequency, their causes and treatments are far apart. UTIs are bacterial infections that usually improve with antibiotics. OAB is a chronic condition of losing bladder control that needs behavior therapy, medications, and possibly physical therapy.
If your test results continue to come back normal, but the symptoms continue, it may be time to rethink things, ranging from infection to overactivity.
Discuss with your doctor. Inquire about further assessment for OAB. Through correct diagnosis, focused treatment is available, and you can once again resume living without constantly looking around for where the next restroom is.
References
- https://www.emedicinehealth.com/fastest_way_to_get_rid_of_a_bladder_infection/article_em.htm
- https://www.ncbi.nlm.nih.gov/books/NBK567751/
- https://emedicine.medscape.com/article/459340-medication
- https://www.sciencedirect.com/science/article/pii/S0301211524004056
- https://www.webmd.com/urinary-incontinence-oab/overactive-bladder-making-diagnosis
- https://rungtahospital.com/urinary-tract-infection
In this Article
























