Medicines quietly become part of a daily routine. Tablets in the morning. Capsules in the night. Something for a headache, something for acidity. Over time, they stop feeling like treatment and start feeling like a habit. And that is exactly where medication mistakes slip in.
Most people do not misuse medicines on purpose. These are not reckless decisions. They are small assumptions.
We assume timing does not matter much.
We assume over-the-counter medicines are always safe.
We assume side effects are just “part of treatment.”
We assume that if something worked once, it will work again.
In reality, common medication errors happen in homes every single day, across age groups, education levels, and health conditions. The issue is not carelessness. It is familiarity.
This article is not about blame. It is about awareness. Because once you see these mistakes clearly, they become surprisingly easy to avoid.
9 Medication Mistakes We Didn’t Know We Were Making
1. Taking Medications at the Wrong Time of Day
Many prescriptions say “once daily.” That line quietly misleads people.
Timing of medication matters more than most realise. Many medicines are prescribed with timing for a reason, not convenience. Some medicines work with your body clock. Others fight against it if taken at the wrong hour.
- Blood pressure medicines may cause dizziness if taken in the morning for some people, especially the elderly.
- Acid reflux medications often work best before meals, not after pain starts.
- Certain medicines irritate the stomach lining when taken on an empty stomach.
The mistake is assuming that once a day means any time is normal. It often does not.
Correct timing improves absorption, reduces side effects, and sometimes decides whether the medicine works at all.
2. Mixing Medications Without Checking Interactions

This is one of the most dangerous medication safety mistakes, and also one of the most common.
People usually inform doctors about prescription drugs. They forget to mention:
- Pain relievers
- Cold and flu syrups
- Herbal supplements
- Vitamins
Some quiet but risky combinations include:
- Multiple pain relievers with the same active ingredient
- Cold medicines along with blood pressure drugs
- Supplements affecting the absorption of thyroid or heart medicines
Most drug interactions do not cause dramatic reactions. They cause subtle harm, increased blood pressure, liver stress, excessive drowsiness, and stomach bleeding.
A pharmacist is not just a billing counter. Pharmacists catch interaction risks doctors may not see in a 5-minute consultation. This is why experts strongly caution against self-directed trial and error.
When choosing a medicine, “it’s really geared toward your symptom,” explains Dr. Brittany Chan, a pediatrician. That’s why, she says, “your best bet is asking your doctor or pharmacist. They can always guide you down the right road based on your symptoms, as opposed to just arbitrarily trying trial and error. We want to be very conscious and thoughtful about what we put in our bodies and for what reason.”
3. Using Over-the-Counter Medications More Often Than Recommended
“OTC” sounds safe. Familiar. Mild.
But over-the-counter medication errors cause more long-term damage than many prescription mistakes.
Common examples:
- Daily painkiller use for back pain or headache
- Regular antacids after meals
- Sleep aids used every night
Overuse signs people ignore:
- Needing a higher dose for the same relief
- Rebound pain or acidity
- Fatigue, kidney strain, liver issues
Pain relievers especially carry silent risks. The damage builds slowly, without warning pain.
OTC does not mean unlimited. It means limited use without a prescription.
4. Stopping a Medication Too Soon
Feeling better is not the same as being better. Many people stop medicines once their symptoms reduce, especially antibiotics.
This is common with:
- Antibiotics
- Acid reflux medicines
- Antidepressants
- Blood pressure medicines after improvement
The problem is that symptoms often improve before the condition stabilises.
This creates two problems:
- Infection not fully cleared
- Resistant bacteria survive
Antibiotic misuse is not only a public health issue. It directly affects future treatment effectiveness for the same person. The mistake is treating symptoms instead of treating the disease duration.
Unless a doctor advises otherwise, finishing the course is not optional. It is part of the treatment itself.
5. Doubling Up After Missing a Dose
Missed dose creates anxiety. People try to “correct” it. Taking a double dose to compensate for the missed dose is one of the most common dosage errors.
Why this is risky:
- Sudden overdose effects
- Blood level spikes
- Increased side effects without extra benefit
Most medicines have forgiveness windows. The body tolerates one missed dose better than a sudden overdose. General safe approach for a missed dose (not a medical order):
- If you remember soon, take it
- If it is close to the next dose, skip the missed one
- Never double unless specifically instructed
Consistency matters more than compensation.
6. Ignoring Side Effects or Assuming They’re Normal
Many people tolerate discomfort silently. They assume that:
- Dizziness is a weakness
- Mood change is stress
- Bloating is a food issue
- Sleep disturbance is a lifestyle
Some side effects are mild and expected. Others are early warning signals. Symptoms that deserve attention:
- Persistent dizziness
- New anxiety or mood swings
- Changes in bowel habits
- Unusual fatigue
Ignoring side effects does not make the body adapt. It makes the damage quieter. Ignoring side effects can lead to:
- Non-adherence later
- Organ stress
- Reduced quality of life
- Preventable complications
Doctors can often adjust the dose or timing to fix side effects, but only if told.
7. Storing Medications Improperly
Storage is rarely discussed. Medicines are sensitive to:
- Heat
- Humidity
- Direct sunlight
Bathrooms and cars are the worst places. Heat breaks chemical stability. Humidity degrades tablets. Light reduces potency.
Result? Medicine looks normal, but it works poorly. This leads people to think medicine “stopped working” and increases the dose unnecessarily.
Proper storage preserves effectiveness. Improper storage creates invisible failure.
8. Sharing Prescription Medications
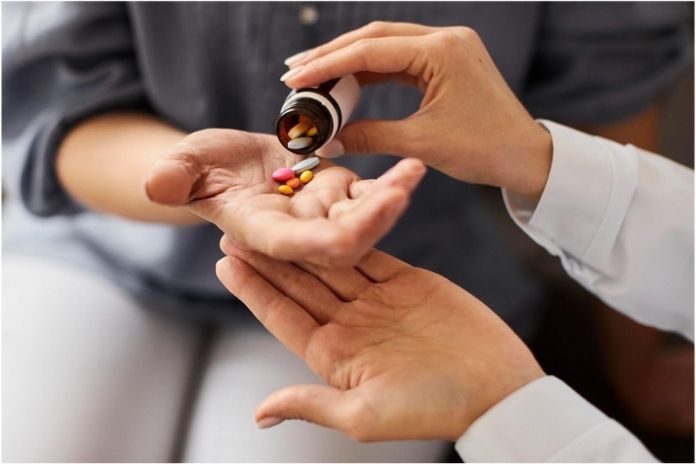
This is done with good intentions: “Try this, it helped me;” “We have the same problem.”
But prescriptions are personalised based on:
- Age
- Weight
- Other conditions
- Existing medications
What suits one body can harm another. There are also legal concerns, but more importantly, safety risks:
- Allergic reactions
- Incorrect dosing
- Masking serious illness
- Delay in the correct diagnosis
Sharing medicines is not kindness. It is guesswork.
9. Not Reviewing Medications Regularly With a Doctor or Pharmacist
Many people continue taking the medication they started years ago. Reasons:
- Condition feels stable
- The doctor didn’t stop it
- Fear of change
But conditions change. Bodies change. New drugs get added. This leads to polypharmacy, multiple medications without reassessment.
Risks increase with age:
- Drug interactions
- Memory issues
- Falls
- Kidney stress
Medication review helps to:
- Stop unnecessary drugs
- Reduce dose where possible
- Simplify schedules
- Identify interactions
A medication review is not an admission of weakness. It is maintenance. Even medicines that were once necessary may become outdated.
Read More: 7 Common Mistakes to Avoid When Using Birth Control Pills
Why Medication Mistakes Are So Common
Medication errors are not about intelligence. They happen because:
- Instructions are complex
- Multiple doctors involved
- Busy daily routines
- Poor explanation at the hospital or pharmacy counter
- Fear of asking “basic” questions
Healthcare often assumes understanding. Patients often assume compliance is enough. That gap creates mistakes. As cardiologist Dr. Daniel Munoz explains, “Medications can be tough to take. They can be complicated to take. Particularly, the more medications somebody is prescribed.”
This complexity is exactly why small, unintentional errors pile up over time, and why medication safety needs simple systems, not just good intentions.
Read More: 10 Proven Ways to Boost Your HDL Cholesterol Without Medication
How to Reduce Medication Mistakes

Small habits create big safety improvements.
- Maintain an updated medication list
- Show it at every consultation
- Ask the pharmacist questions during pickup
- Use pill organisers for long-term medicines
- Set reminders for timing-specific drugs
- Read labels again, even for familiar medicines
Medication safety is not about memorising names. It is about systems.
Read More: Treatment Options for Diabetic Eye Disease: From Laser Therapy to Medications
When to Seek Medical Advice
Do not wait for a crisis. Seek advice if:
- Symptoms worsen after starting the medicine
- You suspect a mixing medications issue
- You want to stop or change the dose
- New symptoms appear without explanation
- You rely on OTC medicines regularly
- You are unsure why you are taking a drug
Doctors and pharmacists are not the last options. They are partners.
Read More: 10 Tips for Managing Arthritis Pain Without Medication
Final Thoughts
Medicines are powerful tools. But power without understanding creates risk. Most prescription drug mistakes are not dramatic. They are quiet, repetitive, and invisible until damage appears.
Being careful with medicines is not paranoia. It is self-respect.
- Medication mistakes often come from routine, not negligence.
- OTC medicines contribute significantly to long-term harm.
- Timing and storage affect effectiveness more than people realise.
- Regular medication reviews reduce polypharmacy risks.
- Research gap remains in patient education around real-world medication use outside clinics.
FAQs
1. Are medication mistakes really that common?
Yes. Studies show most adults make at least one medication error yearly, often unknowingly.
2. Is it safe to take OTC medicines daily?
Daily use should be discussed with a doctor. OTC does not mean risk-free.
3. Can pharmacists really help with medication safety?
Absolutely. Pharmacists are trained specifically to identify interactions and dosing errors.
4. What should I do if I miss a dose?
Do not double. Follow general guidance or ask your doctor for condition-specific advice.
5. How often should medications be reviewed?
At least once a year, or whenever a new medicine is added.
References
- Agency for Healthcare Research and Quality. (2024, December 15). Medication Errors and Adverse Drug Events | PSNet. Ahrq.gov.
- Britten, N. (2009). Medication errors: the role of the patient. British Journal of Clinical Pharmacology, 67(6), 646–650.
- Centers for Disease Control and Prevention. (2024, May 15). Medication Safety and Your Health. Medication Safety Program.
- Tariq, R., Scherbak, Y., Vashisht, R., & Sinha, A. (2024). Medication dispensing errors and prevention. National Library of Medicine; StatPearls Publishing.
- Velo, G. P., & Minuz, P. (2009). Medication errors: Prescribing Faults and Prescription Errors. British Journal of Clinical Pharmacology, 67(6), 624–628.
In this Article















